Repeated dosing of ophthalmic antibiotics following intraocular injection permits the development of resistant bacterial strains, according to a study in the September issue of Archives of Ophthalmology.
“The use of topical antibiotics is promoting antimicrobial resistance, prompting an emergence of resistant strains,” says lead author Stephen Kim, M.D., assistant professor of ophthalmology and visual sciences at the Vanderbilt Eye Institute in Nashville, Tenn. “This is the first prospective study looking at this [specific application], and we were able to convincingly show cause and effect. There needs to be more rational thought when using topical antibiotics.”
In this randomized, controlled, longitudinal study, Dr. Kim and colleagues analyzed 48 eyes from 24 patients who received unilateral intraocular injection for the treatment of choroidal neovascularization. All patients received one injection every four weeks for at least four consecutive months, and then were followed for one year.
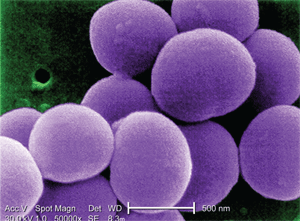
Repeated use of topical antibiotics following intraocular injection can foster the creation of resistant strains of staphylococcal bacteria, as seen here. Courtesy: CDC/Matthew J. Arduino, Dr.P.H.
After initial injection, patients were randomly assigned to receive one of four topical ophthalmic antibiotics: azithromycin 1%, ofloxacin 0.3%, gatifloxacin 0.3% or moxifloxacin hydrochloride 0.5%. Throughout the remainder of the study, patients used only their assigned antibiotic following each subsequent injection.
At baseline as well as after every injection, the researchers obtained cultures of the conjunctiva in both the treated and untreated contralateral eyes. Then, they tested the bacterial samples for susceptibility to 16 different antibiotics.
The researchers determined that repeated exposure to fluoroquinolone antibiotics was associated with the development of coagulase-negative Staphylococci (CNS) that exhibited significant bactericidal resistance to both older- and newer-generation fluoroquinolones. Additionally, repeated exposure to azithromycin was associated with significantly increased resistance to macrolides, but decreased resistance to both older- and newer-generation fluoroquinolones.
Further, the researchers noted that specimens of CNS from treated eyes exhibited a marked increase in multiple-drug resistance. More specifically, 81.8% of CNS specimens were resistant to at least three antibiotics, and 67.5% were resistant to at least five antibiotics.
Kim SJ, Toma HS. Antimicrobial resistance and ophthalmic antibiotics: 1-year results of a longitudinal controlled study of patients undergoing intravitreal injections. Arch Ophthalmol. 2011 Sep;129(9):1180-8.

