 |
|
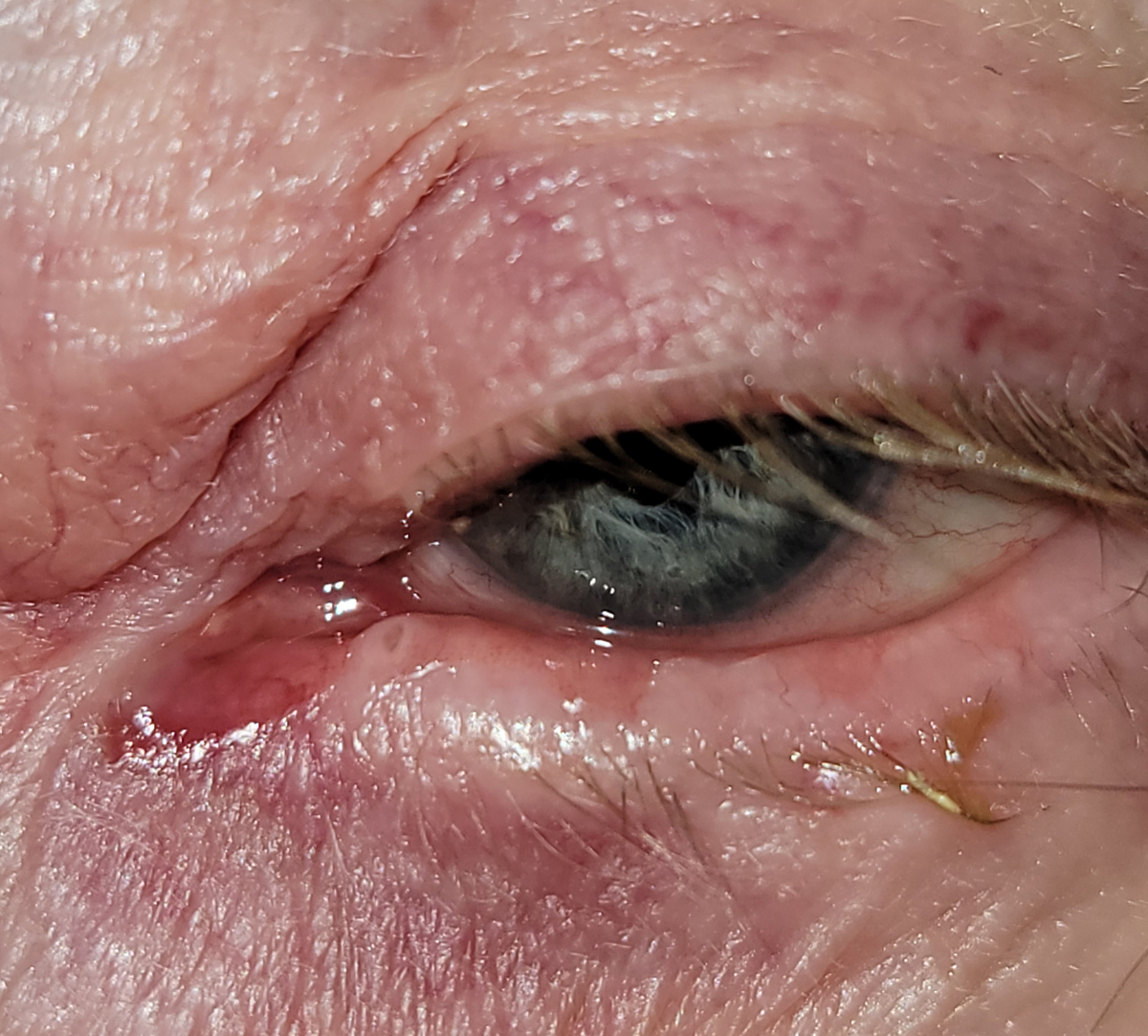
Lacrimal duct obstruction in glaucoma patients may result from chronic exposure to preservatives in topical medications. Photo: Christine Sindt, OD. Click image to enlarge. |
Glaucoma is an all-too-common disease, and with so many patients reliant on topical glaucoma medications, adverse effects are fairly common. One new study sought to clarify the development of ocular adnexal disorders in glaucoma patients using topical therapy, especially since their usage and outcomes have not been examined beyond small, cross-sectional observational studies. Specifically, this research focused on determining the risk of lacrimal drainage obstruction (LDO) and eyelid malposition as a result of topical med usage.
In a retrospective analysis of 16 years of patient data in Ontario, all patients initiating eyedrop treatment for glaucoma or those with suspected glaucoma but not receiving meds were eligible for inclusion in the retrospective analysis. Patients had to be 66 years of age or older. The study included 122,582 patients in the topical meds category and 232,336 in the non-treatment group.
Patients undergoing topical therapy displayed increased rates of entropion, trichiasis and LDO. This category also experienced increased hazards for entropion, trichiasis and LDO while displaying decreased hazard for ectropion. Despite this, the absolute differences in survival of these outcomes were small and uncommon between the two groups, noticeable mostly only after several years of therapy.
The researchers noted four reasons why the observed effects are important: (1) glaucoma is a common disease and large numbers of patients are treated with topical drugs; (2) use of such meds is frequently long-term; (3) therapies that avoid topical drug delivery are increasingly available; and (4) the question of an association between topical medication exposure and incidence of eyelid malposition or LDO remains unanswered in the literature.
Overall, patients using topical glaucoma drugs were more likely to have an increased risk of needing LDO repair (either by canalicular stenting or dacryocystorhinostomy), entropion repair and repair of trichiasis (by electrocautery or cryotherapy). The researchers assert that this is the first study to illustrate population-level evidence that topical glaucoma drug use is indeed associated with subsequent LDO surgery, as well as confirming obstruction may only happen years after therapy has started.
One explanation for these results is the upregulation of inflammatory pathways that underlies ocular surface disease. This type of display is somewhat normal in those who have been using topical agents long-term, as the preservatives used in many popular therapies trigger inflammatory symptoms.
In response, chronic topical preserved-drug exposure may change anterior segment tissue through chronic inflammation, leading to entropion and trichiasis; however, at the same time, vertical shortening and mechanical tethering of the posterior lamella may protect against ectropion. Thus, it is likely that iatrogenic inflammation is a mechanism common to ocular surface disease, eyelid malposition and LDO for glaucoma patients.
Considering these findings in a practical setting, the authors say they “support the growing role for therapies that reduce or delay [topical medication] use, such as laser trabeculoplasty and novel drug delivery systems.”
Quinn MP, Kratky V, Whitehead M, et al. Association of topical glaucoma medications with lacrimal drainage obstruction and eyelid malposition. Eye. December 6, 2022. [Epub ahead of print]. |

