
Spring is upon usa magical time when automobiles mysteriously become coated in yellow and optometric offices get crammed with patients suffering from ocular allergy. Each spring, every optometrist in clinical practice deals with droves of allergy sufferers.
A nationwide survey found that more than half (54.6%) of all Americans tested positive to one or more allergens.1 Of these, 83% suffer ocular symptoms.
Some simple math will give you an idea of the extent of the problem as it relates to your practice. Simply multiply your total number of patients by 0.42. The resulting number indicates the number of patients who could benefit from your expertise in allergy.
The costs associated with allergic disease are extraordinarily high; one analysis estimated total treatment cost at $7.9 billion per year.2 And, considering that most of your patients with allergies also suffer from allergic conjunctivitis, the evidence of this problem is very real.3
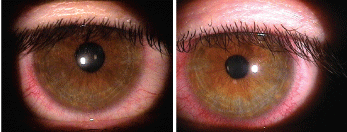
Eighty-three percent of individuals who test positive to one or more allergens also demonstrate ocular complications, such as seasonal or perennial allergic conjuntivitis. Courtesy: Mile Brujic, O.D.
Pathophysiology
In general, allergy is a complex disorder. Simply put, an allergic response is an unwarranted over-reaction of the bodys immune system to foreign substances (allergens), which the body perceives as a potential threat. The response can be innate or acquired.
Allergic disease is not an isolated presentation, but a unique interaction of an environmental allergen and an individuals innate physiologic response mechanism. Active ocular allergy is a very specific form of an inflammatory ocular surface disease.
The process is set in motion by IgE antibodies that are fixed to the surface of mast cells. When the IgE complex encounters an allergen, the cell membrane of the mast cell ruptures, which causes degranulation of the mast cells.
To use a football analogy, the quarterback in the allergic cascade is the mast cell. There are some 50 million mast cells in the human eye. Once activated, the mast cell dumps chemical markers, known as histamine, into nearby tissues and stimulates a variety of changes. Each mast cell contains five to 10 picograms (10-9) of histamine. There are three types of histamine receptors in the human body:
H1, which is found in gastrointestinal smooth muscle.
H2, which is found in cardiac tissue.
H3, which is found in the central nervous system and other functions, such as dilating arterioles and veins.
In the quiescent eye, most mast cells are located deep in the substantia propria. In an allergic state, the mast cells migrate to the more superficial tissue layers and release histamine. Histamine is non-selective; it stimulates all three of the receptors indiscriminately. The key to modulating an allergic event is to block these receptor sites and prevent the release of histamine by the cell. The H1 receptor is the most important subtype in the eye because it mediates itching and some vasodilatation.
The presence of an allergen on the conjunctiva initiates two simultaneous immune responsesone caused by the release of pre-formed inflammatory mediators, such as histamine from mast cells, and the other caused by the production of arachidonic acid and its conversion to newly-formed mediators, such as prostaglandins. Pre-formed mediators are released immediately upon exposure, whereas the release of newly-formed mediators is delayed roughly eight to 24 hours.4
Meanwhile, other mediators released from mast cells send out chemical signals that attract both red and white blood cells to the area. Once these cells arrive, they easily reach the conjunctival surface by moving through the dilated and highly permeable capillaries. The bodys other defense mechanism, referred to as the arachidonic acid cascade, produces three newly-formed inflammatory mediators: prostaglandins, cytokines and leukotrienes. These mediators are collectively known as eicosanoids.
There are two phases of allergic conjunctivitisearly and late. Think of early-phase reactions as a light switch that is turned on and then turned off by the natural process of the immune system or by medications.
Late-phase reactions occur in more severe allergic states and represent a cellular response to prolonged allergic challenge in conditions of vernal or atopic keratoconjunctivitis. Late-phase reactions are particularly troublesome for the patient because of the cellular response and tissue destructive effect of mediators released from degranulating neutrophils, eosinophils and basophils. So, late phase changes are like a light switch that is turned on and the immune system then has profound difficulty turning itself off.
Categories of Ocular Allergy
Allergic eye disease is typically divided into five primary subcategories:
Seasonal allergic conjunctivitis (SAC) is classified as an acute allergic condition and is typified by early-phase changes.5 SAC typically is caused by pollen released into the air by flowers, trees, grasses and weeds. Symptoms are most severe when the pollen counts are highestduring the spring and fall. A pollen count represents the concentration of all airborne pollen in a certain area at a specific time. The number is expressed as grains of pollen per cubic meter over a 24-hour period. The National Allergy Bureau provides local pollen counts, starting in March or April of a given year.6 As the pollen counts rise in your area, you can expect to see more patients suffering from SAC. For more about your local pollen count, visit: www.aaaai.org/nab.
Perennial allergic conjunctivitis (PAC) produces year-round symptoms because the causative allergens are always present. Dust mites and pet dander often cause PAC.7 Other common allergens that cause perennial allergic conjunctivitis are mold, air pollutants, smoke and cosmetics.6 It is important to note that PAC, depending on severity, can be classified as either acute or chronic.
Affected individuals often have a history of atopic disease. PAC is usually present from the time of infancy. However, ocular allergies, including PAC, can develop at any time in a persons life. Patients with PAC generally present with itching, conjunctival redness, chemosis, eyelid swelling and tearing; however, symptoms are often milder than those associated with SAC.
Atopic keratoconjunctivitis (AKC) is a perennial disorder. An AKC patient usually demonstrates a history of atopic dermatitis or eczema that has persisted since childhood. The condition frequently occurs in men aged 30 to 50 years.5 The primary symptom of AKC is intense bilateral itching of the lid skin, periorbital area and conjunctiva. Tearing, burning, photophobia, blurred vision and a stringy, rope-like mucus discharge may also be observed.5 Meibomian gland dysfunction and related dry eye are also generally associated with AKC.
Vernal keratoconjunctivitis (VKC) is primarily a disease of childhood that is seen predominately in boys and young men ranging from three to 20 years of age. Patients with VKC complain of intense itching and tearing; a hot, tight, sensitive feeling to eyes; and photophobia.5 Research has documented that histaminase deficiency exists with VKC.5 Histaminase is the enzyme that degrades histamine to its benign substrates. A VKC patient may also present with ptosis; conjunctival injection; large, non-uniform cobblestone papillae; limbal bumps; and Horner-Trantas dots.5
Giant papillary conjunctivitis (GPC) is an immune response, not a true allergy; however, the condition is still classified as an allergic reaction. It is caused by repeated mechanical irritation and is aggravated by concomitant allergy. GPC is associated with contact lenses, ocular prosthetics, exposed sutures, cyanoacrylate adhesive, extruded scleral buckles and ocular foreign bodies.
The vast majority of what we see in primary care is either seasonal or perennial in naturemore than 90% to 95% of all ocular allergies are characterized by SAC or PAC.6 SAC is more common than
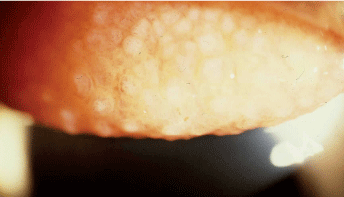
Giant papillary conjunctivitis (GPC), as seen in this patient, is caused by repeated mechanical irritation and is aggravated by concomitant allergy.
Diagnosis
When a patient presents with an acute red eye, the patient history often guides the exam. Of course, there is the old saying: If it itches, then its allergy. The patient may present with a family history of atopic disease, such as allergic rhinitis, bronchial asthma or atopic dermatitis. However, the chances that the patient will present to your office during an acute allergic episode are slim.
On examination, eyelid redness, edema and venous dilation can cause lower lids to appear darker than normal. This is often called the allergic shiner, and is caused by the effect of histamine on tissues periocularly. Be sure to ask about nasal discharge, sinusitis and congestion-rhinitis. Bilateral bulbar conjunctival chemosis (gelatinous) and mild injection may be observed. Often, fine papillae can be seen on the superior tarsal papillae.
We must differentially diagnose ocular allergy from other causes of acute red eye, such as infectious keratitis or acute anterior uveitis.
The most common differential of allergy, however, is dry eye. But, that is like the chicken and the egg question: Which came first? The two conditions often co-exist because the dry eye patient typically does not produce enough tears to wash offending allergens out of the eye. In addition to patient history, the clinical signs aid in the differential diagnosis. Dry eye presents with grittiness, burning and signs of ocular surface disease, as well as staining of the cornea and conjunctiva. An infectious process shows discharge.
The Eye is a Window to Allergy Why is the eye so often involved in allergic cases? In short, the eyes lack the filters that the nose and lungs possess. The conjunctiva represents the upper extremity of the respiratory system and maintains a drainage system into the nose through the nasolacrimal duct. The ocular surface can be considered a relatively large collection window, an area of several hundred square millimeters, that permits entry of allergens into the body. Allergens, allergic mediators released from mast cells and antiallergy eye drops drain into the nose by way of this pathway and contribute to nasal symptomatology.
Treating Ocular Allergy
Ocular allergy treatment often requires a multi-prong approach.
Avoid allergens. The first line of therapy for allergic conjunctivitis is to avoid contact with allergens as much as possible. This means that those individuals afflicted with seasonal allergies should shy away from outdoor activities during pollen season.
Air conditioning or air purification can benefit sufferers of both seasonal and perennial ocular allergies. Patients with PAC caused by pet dander should consider keeping their cats and/or dogs off of their beds and pillows and out of the bedroom entirely. Dust control may provide some benefit by reducing the interior allergen load.
Treat topically. When treating ocular allergy, treat both signs and symptoms. Prescribe an agent with a long duration and broad mechanism of action. Also, be certain to employ an agent with minimal side effects. Treat allergic conjunctivitis topically to avoid systemic effects and to bring about rapid recovery. Systemic antihistamines have been shown to cause ocular dryness, and have the potential to exacerbate ocular allergy due to diminished dilution and flushing of antigen and inflammatory mediators.8
Avoid OTC vasoconstrictors. While topical ocular therapy has been shown to reduce rhinitis symptoms (e.g., sneezing, runny and itchy nose and blocked nostrils), many patients first try over-the-counter antihistamine/decongestant drops, such as Naphcon-A, Vasocon-A and Visine-A.
But, patients who take OTC drops may not fully understand the potential chronicity of their condition and the importance of focused, controlled treatment. While OTC agents enjoy a long-standing safety record, their duration of action is limited to two to three hours and they typically require frequent dosing.6 In fact, allergic conditions can be made worse by the presence of preservatives and other chemical agents contained in OTC drops.
Target topical treatment. Topical antihistamines are effective for rapid relief of itch. Antihistamines have the ability to occupy histamine receptors because of their high affinity to H1 receptors, thus preventing the destabilization of the mast cell wall. In doing so, they prevent binding of histamines, which blocks the key triggers related to allergen-induced itching. However, q.i.d. dosing is tedious, and some patients often complain of irritation.
Mast-cell stabilizers can be prescribed for patients with known allergies and should be used before allergy season begins. These agents take several weeks of use before maximum effect is achieved and require a loading period before efficacy is observed.
Four Questions On Allergy In cases of suspected ocular allergy,four specific questions may help steer you in the right direction: Do you ever have episodes of intense itching, along with varying degrees of tearing, redness and swelling that are related to specific activities? Do you, your parents or other family members have allergies or a history of allergy? Has a doctor ever prescribed (or have you ever purchased) any eye drops for itching and redness? Has a doctor ever prescribed (or have you ever purchased) oral antihistamines (e.g., Claritin [loratadine, Schering Corporation]) for sneezing, wheezing, runny nose, or other symptoms?
Combined antihistamine/mast-cell stabilizers are the most commonly prescribed agents for allergic conjunctivitis. These medications are considered the standard of care for ocular allergy; they do not require loading and can be used throughout the entire allergy season.10 Several of these combination medications, such as ketotifen, are now available OTC.
These drugs might have synergistic properties. A study conducted in 1999 showed that selected topical ocular drugs with antihistaminic activity might offer therapeutic advantages by inhibiting proinflammatory cytokine secretion from human conjunctival epithelial cells.11 Also, topical combination agents have not been found to cause ocular surface drying.12
But, the best results are obtained when topical agents are used as adjunctive therapy with oral meds for greater effect. A study at the
Ocular allergy is a highly prevalent eye diseaseone that patients often self-diagnose and self-medicate. While the disease process itself is rather complex, the treatment is very straightforward and highly successful, particularly for seasonal and perennial allergic conjunctivitis. In our experience, primary eye-care providers are not initiating therapy early enough and not offering to make a difference in their patients daily life. The most effective therapy for seasonal and perennial allergy is a combination medication that provides mast-cell stabilization, anti-histamine and anti-inflammatory effects.
Make a commitment to spend a few moments discussing treatment benefits with your patients and help rid them of long-term issues related to allergy.
Dr. Bowling is center director at VisionAmerica, a surgical comanagement center in
1. Gergen, PJ, Turkeltaub, PC, Kaovar, MG. The prevalence of allergic skin test reactivity to eight common aeroallergens in the
2. Stempel DA, Woolf R. The cost of treating allergic rhinitis. Curr Allergy Asthma Rep 2002 May;2(3):223-30.
3. Bielory L. Update on ocular allergy treatment. Expert Opin Pharmacother 2002 May;3(5):541-53.
4. Bonini S. Allergic conjunctivitis: the forgotten disease. Chem Immunol Allergy 2006; 91:110-120
5. Ono SJ,
6. The
7. Abelson M. Allergic Diseases of the Eye.
8. Abelson M, Welch DL. An evaluation of onset and duration of action of Patanol (olopatadine hydrochloride ophthalmic solution 0.1%) compared to Claritin (loratadine 10mg) tablets in acute allergic conjunctivitis in the conjunctival allergen challenge model. Acta Ophthalmol Scand Suppl 2000;(230):60-3.
9. Crampton HJ. A comparison of the relative clinical efficacy of a single dose of ketotifen fumarate 0.025% ophthalmic solution versus placebo in inhibiting the signs and symptoms of allergic rhinoconjunctivitis as induced by the conjunctival allergen challenge model. Clin Ther 2002 Nov;24 (11):1800-8.
10. Bielory L. Differential diagnoses of conjunctivitis for clinical allergist-immunologists. Ann Allergy Asthma Immunol 2007 Feb;98(2):105-14; quiz 114-7, 152.
11. Yanni JM, Weimer LK, Sharif NA, et al. Inhibition of histamine induced human conjunctival epithelial response by ocular allergy drugs. Arch Ophthalmol. 1999 May;117(5): 643-7.
12. Torkildsen G,
13. Lanier BQ, Abelson MB, Berger WE, et al. Comparison of the efficacy of combined fluticasone propionate and olopatadine versus combined fluticasone propionate and fexofenadine for the treatment of allergic rhinoconjunctivitis induced by conjunctival allergen challenge. Clin Ther 2002 Jul;24(7): 1161-74.

