Indeed. Several studies have shown that uncorrected visual problems are linked to poor academic performance. And, poor academic performance has been linked to low self-esteem and behavioral problems.
Besides myopia, hyperopia and astigmatism, primary-care optometrists must be aware of non-refractive conditions that are common in school-aged children. The five most common: amblyopia, ocular motor dysfunction, accommodative insufficiency, convergence insufficiency and convergence excess.
These five conditions are very manageable, because they are:
Prevalent in the school-aged child and therefore easy to pinpoint.
Easy to test for.
Successfully treated in one or two examination sessions (except for amblyopia, which requires intensive follow-up).
In this second installment of Review of Optometrys three-part series, Pediatric Practice, we will discuss how the primary-care optometrist can readily manage these conditions. Also, we will discuss when referral to a vision therapy specialist is warranted.
Amblyopia Management
In the only study, thus far, to measure a clinical population of children ages 6 to 18, the prevalence of amblyopia was found to be 7.8%.1 The causes of amblyopia are anisometropia, strabismus, a combination of strabismus and anisometropia and visual deprivation.2
When a school-aged child has decreased vision in one eye due to anisometropia, first rule out a path-ological cause, such as a tumor. If the cause is not pathological, give him a spectacle, contact lens or combination correction. The goal here is to get the child into the full correction necessary as quickly as possible. Then, have the child return for a follow-up visit six weeks later. (Six-week follow-up visits are the standard for the treatment of amblyopia.)
At the first follow-up, you may note that the patients vision has already improved. Assess visual acuity at both distance and near. (Be certain to use the same visual acuity methods at each exam for consistency.) Be sure that the child wears his correction full-time, and that he is comfortable with it.
A subjective refraction over the childs correction will allow you to decide if any further change in the correction is needed to produce better visual acuity. If you decide to make any corrections, wait until the next six-week follow-up to implement further treatment.
Once you are confident that your patient is wearing the best full-time correction, begin therapy. Before prescribing any form of therapy, discuss each one with the patient and his parent or guardian to find out which they prefer. The three possible options:
Occlusion therapy (patching of the preferred eye). If you use this option, tell the parent that the child must actively stimulate the poorer eye as much as possible. This can be done with active near-point activities, such as coloring, drawing, placing beads on strings, reading appropriate print-size books or even playing computer games that have small targets.
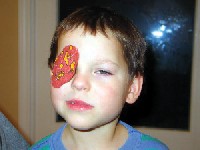 |
| When using occlusion therapy (patching of the preferred eye) to correct amblyopia, the child must actively stimulate the poorer eye as much as possible. A clinical pearl: children are less likely to remove patches that stick to their skin. |
The biggest question most practitioners have about occlusion therapy is how long the patient should wear the patch each day. The Pedi-atric Eye Disease Investigator Group addressed this topic in the Amblyopia Treatment Study 2A and 2B (ATS 2A, 2B). In the ATS 2A, the researchers found that children ages 3 to 7 who had severe amblyopia (20/100 to 20/400) achieved as good results with six hours of patching a day as full-time patching of the poorer eye.3 Children ages 3 to 7 who had moderate amblyopia (20/40 to 20/80) achiev- ed the same results with two hours of patching per day as with six hours of patching.4
Atropine eye drops (daily). Instillation of atropine 1% drops each morning in the patients good eye is also a successful therapy, as shown in recent studies. One study compared atropine with occlusion therapy in patients younger than age 7 who had amblyopia in the range of 20/40 to 20/100.5 One drop of 1% atropine once daily yielded equivalent results to a minimum of six hours of patching the preferred eye daily.
Atropine (weekends only, again in the morning). Another study compared daily atropine use with weekend atropine use in amblyopic children ages 3 to 7. The patients achieved similar positive visual acuity outcomes whether they received atropine daily or only on week-ends.6
I personally prefer occlusion therapy, using eye patches that stick to the patients skin. (Children are less likely to remove patches that stick to the skin.) With this method, I do not have to worry about any pharmacological adverse side effects, such as increased IOP, among others.
The goal of amblyopia treatment is to improve the visual acuity of the poorer eye, so that it equates to the acuity values of the preferred eye, or to get the patient within one or two lines of the target acuity. Regardless of which goal you aim for, you want to be able to maintain this improvement over time. Thus, once youve achieved the goal, close monitoring of the patients visual acuity with six-week follow-up visits is necessary.
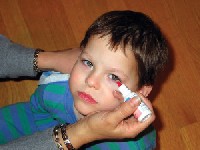 |
| The use of atropine drops is another way young amblyopia patients can achieve good visual acuity outcomes. |
If the patients acuity has reached a plateau at a level that is unacceptable to the patient, refer him to a pediatric optometrist for further management. This type of patient often exhibits eccentric fixation and needs more extensive treatment. (You may find the nearest specialist by checking out the following web sites: www.covd.org or www.oep.org.)
Treatment of strabismic amblyopia, a combination of strabismus with anisometropia amblyopia and treatment of visual deprivation amblyopia can be complicated endeavors. As a result, you may want to refer children who present with these types of amblyopia to a pediatric optometrist for evaluation and treatment.
The prevalence of ocular motor dysfunction in a clinical population of children ages 6 to 18 was found to be 0.7%.1 Children who have difficulties when reading, such as loss of place, skipping lines, skipping words and slow inefficient reading often have poor saccadic pursuit and fixation abilitiesforms of ocular motor dysfunction.7
Gross observation using appropriate targets, such as a small sticker, a small toy, or those targets employed by the Developmental Eye Movement test (DEM) (a test that measures eye movement and automaticity of number naming) and the Visagraph III Eye-Movement Recording System (a test that includes infrared goggles that plug into a computer and measure eye movement), can help you diagnose ocular motor dysfunction. For most primary-care optometrists, the DEM is a good test to incorporate into your practice, as it is inexpensive, quick and easy to administer. (You may even want to have one of your technicians administer the test prior to the examination.)
Once you diagnose ocular motor dysfunction, initiate either in-office or home-based vision therapy. The patient can do these simple home activities to improve his ocular motor function:
Put jigsaw puzzles together.
Solve simple mazes, crossword puzzles or word searches.
Fill-in all of the os on a newspaper page.
Track a moving target, such as a flashlight, in which the child holds a flashlight and chases the parents light with his own (flashlight tag).
Use a computer-based home-vision therapy program to work on pursuit and saccadic movements. (For examples, see http://homevisiontherapy.com or www.bernell.com.)
Use a highlighter or index card while reading to keep his place.
You can also send the patient home with letter charts, such as the Hart Chart. Ask him to read letters from the first column, then the letters from the 10th column, letters from the second column to the ninth column, etc. Finally, you can send home letter- or symbol-tracking paragraphs for the child to search for the alphabet in each paragraph.
Also, suggest that the parents talk with the childs teacher about moving him closer to the chalkboard, so that there are fewer visual distractions. This will make copying from the board easier.
The standard for significant improvement is the daily participation in three to five of the activities listed above. If, however, the child has been working faithfully on these activities and still has difficulties, refer him to an optometrist who specializes in office-based vision therapy.
The amount of time between office visits depends on both your comfort level with this non-refractive condition and the individual patients needs.
| Difficult Conditions to Treat The following conditions may be more challenging without a pediatric/binocular vision background. Strabismus. This patient is unable to align both eyes simultaneously under normal conditions. One or both of the eyes may turn in, out, up or down. The eye turn may be constant or intermittent.8 This condition is best managed by an optometrist who has experience in treating all aspects of the visual system that can occur with this condition. Such aspects include eccentric fixation and anomalous correspondence. Special testing and treatment techniques are necessary herethings you may not have access to in your office. Visual information processing disorders. A patient with these vision disorders has visual processing problems, which include categories such as visual-spatial, visual-analysis, visual-motor and auditory-visual integration skills. To test for these problems, you can use the Reversal Frequency Test, the Test of Visual Perceptual Skills-Revised or the Test of Visual Motor Integration. You may not have these tests available in your office, and these patients often need extensive long-term in-office visual processing therapy.9 Divergence excess. This is a visual condition in which the patient has more exophoria at distance than at near, along with a high AC/A ratio. This is more difficult to manage, as the patient will often exhibit suppression or diplopia at distance and will need more intensive in-office vision therapy to improve the condition.7 Divergence insufficiency. In this condition, the patient exhibits significantly more esophoria when looking in the distance than at near, and he exhibits a low AC/A ratio. This patient will need more intensive in-office vision therapy to improve the symptoms. If patients with any of the above conditions present to your practice, refer them to a pediatric/binocular vision specialist in their area. C.A. |
Accommodative Insufficiency
The prevalence of accommodative insufficiency in a clinical population of children ages 6 to 18 was found to be 6%.1 Symptoms of accommodative insufficiency are blurry vision from near work, headaches from near work,
eyestrain, fatigue and general avoidance of near work.8 The treatment for accommodative insufficiency in a primary-care practice involves:
Correction of the near refractive error. To determine the appropriate near correction for the patient, consider the negative relative accommodation (NRA) and the positive relative accommodation (PRA) findings. For example, if the NRA was +2.75D and the PRA was 0.75D, this would suggest an add of +1.00D to balance the NRA and PRA.
You may also use the monocular estimation method (MEM) retinos-copy finding as a starting point to determine the near-point correction. For example, if the MEM finding was +1.25D, the expected add would be +0.75 (since the normal MEM finding is +0.50).
Use either of these methods as a starting point to prescribe a trial frame to the patient. Change the lenses in 0.25D steps to determine which lenses feel the most comfortable to the patient when he is reading print in the size to which he is accustomed.
Types of lenses for near-point work. These can be reading-only glasses or bifocals. If the patient chooses reading-only glasses, emphasize the importance of wearing the glasses whenever he does extended near-point activities, such as reading, homework, test-taking and computer work.
If he seems uncertain of when to use the glasses or his parent does not feel that the child will use them consistently, prescribe a bifocal. Set the segment height at the lower pupil border to ensure that the child uses the bifocal when he reads.
When explaining the use of a bifocal lens, reassure the parent that that child will adapt to the bifocal very quickly and easily, and that he can get lenses without the lines if he prefers. (You may want to refer to the correction as a multifocal lens, because many people associate the term bifocals with geriatric patients only.)
Vision therapy. Reassess the patient three months after prescribing the near lenses to determine if his symptoms have resolved or have lessened with the use of the lenses. If the child is symptomatic or non-compliant at the follow-up visit, refer him to an optometrist who specializes in accommodative office-based vision therapy.
 |
| One of the ways a patient who has ocular motor dysfunction can work on pursuit and saccadic movements is by using a computer-based home vision therapy program. |
Convergence Insufficiency (CI)
The prevalence of CI in a clinical population of children ages 6 to 18 was found to be 5.3%.1 Patients with convergence insufficiency (CI) are often quite symptomatic.7
Although we most often associate double vision while reading with CI, many patients with this condition will not have this complaint. In fact, eyestrain, headaches after near work, blurry vision and fatigue are also common symptoms.7
The first step to treating any binocular vision dysfunction is to be sure that the patient is wearing his appropriate refractive correction. Once he is best corrected, consider office-based vision therapy. A recent report by the Convergence Insufficiency Treatment Trial Study Group found that office-based vision therapy was a successful treatment, while home-based pencil push-up therapy was no more effective than placebo treatment.8
If the child and his parents are not interested in vision therapy, are unable to afford it or do not live in an area where office-based vision therapy is available, use horizontal relieving prisms to reduce the patients symptoms. These two methods can determine the amount of base-in prism you can prescribe for reading:
Sheards criterion. Suppose, for example, a patient has 12.00 prism diopters (PD) of exophoria at near, base-out ranges of 15/20/12 and base-in ranges of 6/8/6. Prism needed = 2/3 phoria 1/3 compensating fusional vergence. The prism = 2/3(12)-1/3(15) = 3.00PD. Thus, you would prescribe 1.50PD base-in prism for each lens.
Percivals criterion. Lets again use the patient mentioned above. Prism needed = 1/3 (greater of the lateral limits) 2/3 (lesser of the lateral limits). The prism = 1/3(15) 2/3(6) = 1.00PD. Thus, you would prescribe 0.50PD base-in prism for each lens.
Whichever method you use, consider that prism to be a starting point. Give the patient a trial frame with the prism, so that he can assess his comfort. Then, increase or decrease the prism amount in the trial frame to determine the optimum comfort level of the patient. If there is a range of comfort, I give the lowest amount of prism that allows for patient comfort. Splitting the prism amount between the patients two lenses to keep the lenses cosmetically acceptable is customary.
If the child cannot verbalize any change in comfort, reassure the parent that the patient may need to get used to wearing the new glasses. Also, tell the parent that a better representation of the childs comfort with the glasses will occur after he has worn them for a while. (The amount of time depends on both your comfort level with this non-refractive condition and the individual patients needs). If the child is still symptomatic after the use of base-in prism for reading, strongly encourage the childs parents to consider office-based vision therapy.
Convergence Excess (CE)
In a clinic-based population of children ages 6 to 18, 8.2% were found to have convergence excess.1 Patients who exhibit symptoms of convergence excess (CE) often complain of eyestrain, headaches, double vision and blurred visionall of which are associated with near work. The first line of treatment is an appropriate refractive correction. Then, give the patient added plus lenses at near, usually in the form of a bifocal.
The amount of plus power necessary for near can be determined in three ways: NRA/PRA, MEM findings and accommodative convergence/accommodation (AC/A) ratio. Here is an example of using the AC/A ratio: A patient exhibits 6.00PD of esophoria at near, with an AC/A ratio of 4/1. We would expect +1.50D to bring the 6.00PD of esophoria down to a value of orthophoria.
After you determine the amount of plus, give the patient a trial frame. Then, assess his comfort level prior to a final correction.
Added plus lenses for reading are very effective treatments for CE. However, if the patient has some moderate esophoria at distance and at near, consider the use of a base-out prism for full-time wear. You can calculate a starting point to investigate the use of the prism using Sheard or Percival criterion as described above.
If the patient is still symptomatic after the use of lenses or prism, refer him for office-based vision therapy. This is often the case for patients with large amounts of esophoria or a combination of CE and other binocular conditions.
The amount of time between office visits depends on your comfort level with this non-refractive condition and the individual patients needs.
As primary-care optometrists, we can diagnose and manage these and other conditions. By doing so, we can ensure that these young patients have every opportunity to experience all the perpetual intoxications of youth.
Dr. Allison is an associate professor at the Illinois College of Optometry and is program coordinator for the colleges Binocular Vision and Pediatric Optometry Residency. She is also a diplomate in binocular vision, perception and pediatric optometry of the American Academy of Optometry and a fellow of the College of Optometrists in Vision Development.
Next month: In Pediatric Practice, Part 3, Dr. Allison will discuss how to assess convergence, eye movement and accommodative problems in the school-aged child.
1. Scheiman M, Gallaway M, Coulter R, et al. Prevalence of vision and ocular disease conditions in a clinical pediatric population. J Am Optom Assoc 1996 Apr;67(4):193-202.
2. Woodruff G, Hiscox F, Thompson JR, Smith LK. Factors affecting the outcome of children treated for amblyopia. Eye 1994;8(Pt 6):627-31.
3. Holmes JM, Kraker RT, Beck RW, et al. A randomized trial of prescribed patching regimens for treatment of severe amblyopia in children. Ophthalmology 2003 Nov;110(11):
2075-87.
4. Repka MX, Beck RW, Holmes JM, et al. A randomized trial of patching regimens for treatment of moderate amblyopia in children. Arch Ophthalmol 2003 May;121(5):603-11.
5. Pediatric Eye Disease Investigator Group. A randomized trial of atropine vs. patching for treatment of moderate amblyopia in children. Arch Ophthalmol 2002 Mar;120(3):268-78.
6. Repka MX, Cotter SA, Beck RW, et al. A randomized trial of atropine regimens for treatment of moderate amblyopia in children. Ophthalmology 2004 Nov;111(11):2076-85.
7. Scheiman M, Wick B. Clinical Management of Binocular Vision, 2nd ed. Philadelphia: Lippincott, Williams & Wilkins, 2002:3-52.
8. Scheiman M, Mitchell GL, Cotter S, et al. A randomized clinical trial of treatments for convergence insufficiency in children. Arch Ophthalmol 2005 Jan;123(1):14-24.
8. Optometrists Network. Strabismus: What is it?
www.strabismus.org/ (10 March, 2005).
9. Sheiman M, Rouse M. Optometric Management of Learning-Related Vision Problems. St. Louis: Mosby-Year Book, Inc., 1994: 298-305.

