 |
Dermatology and optometry are integrally related. Consider: Many conditions of the skin, such as rosacea, seborrhea, eczema and psoriasis, can significantly impact our patients visual health. Likewise, the skin of the lids and ocular adnexa may be affected by various hyperplastic and neoplastic disorders.
These lumps and bumps present an opportunity for optometry to diagnose and manage conditions beyond the purely refractive and ocular realm. Here, well look at five types of skin abnormalities you may encounter and the latest treatments with which to manage them.
Verrucae and Molluscum Contagiosum
Verrucaemore commonly known as wartsappear as one or more elevated, round to oval le-sions. They are usually white or yellow in color but may vary in pigmentation depending on the skin tone. Magnification reveals numerous filiform stalks of fibrovascular tissue that emanate from a larger, non-erythematous base. Tiny black dots near the surface of these projections represent thrombosed, dilated capillaries and are pathognomonic for this condition. The surface usually becomes keratinized over time.
Molluscum contagiosum is characterized by focal, round, dome-shaped nodules, that have a depressed or umbilicated center and are approximately 2mm to 3mm in diameter. The lesions generally appear white or pink in color and contain a translucent, cheesy material. Molluscum contagiosum may occur in clusters or groups, particularly in immunocompromised individuals. They may affect any aspect of the periocular skin but have a predilection for the lid margin.
Both verrucae and molluscum are viral in origin. Verrucae occur secondary to the human papilloma virusa double-stranded, non-enveloped DNA virus that is spread by direct contact. Molluscum contagiosum is associated with a large DNA poxvirus that is transmitted in similar fashion.
 |
|
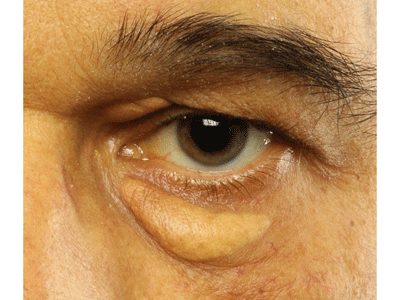
Non-surgical therapies for xanthelasma may include chemical removal with trichloracetic acid. |
Two topical medications recently have shown success in treating both verrucae and molluscum. One agent, Cantharone (cantharidin, Dormer Laboratories), is a vesicant derived from a species of beetle. Cantharidin causes a blistering reaction at the base of the lesion, resulting in overlying necrosis and shedding of the verruca or molluscum. However, cantharidin-induced blisters can cause extreme discomfort, so it may not be practical for all patients. Cantharone is available for physician use only via http://dormer.com/physicians/, though it is not FDA approved for prescription in the United States.
Another agent, Aldara (imiquimod 5% cream, 3M) is an immunomodulatory agent approved in the United States for the treatment of external genital warts, actinic keratosis and certain basal cell carcinomas. However, dermatologists often use this medication off-label for other skin lesions, including verrucae and molluscum contagiosum.
Aldara turns on the immune system at the site of application, inducing a macrophage-mediated inflammatory response. The bodys immune system cannot accomplish this naturally because the underlying viral entities do not normally pop up on the bodys immune radar. Aldara is typically applied three times per week for viral lesions, and therapy may take anywhere from four to 16 weeks. The package insert suggests that Aldara not be used in or near the eyes, although several cases of successful periocular use without incident have been reported.1,2
Xanthelasma
Xanthelasma represent a cutaneous deposition of lipid-laden macrophages. They are associated with elevated serum lipids in about half of patients.3 Xanthelasma are usually seen near the inner canthus of the upper or lower eyelid. They appear as oval or elongated yellowish plaques just beneath the skin. Patients who have xanthelasma are usually past age 40, and women are affected nearly twice as often as men.4
While xanthelasma are essentially benign, many patients opt for removal due to cosmetic concerns. Treatment modalities may include chemocautery, electrodesiccation, cryotherapy, CO2 or argon laser ablation and, as a last resort, surgical excision. Scarring may result from laser or cryotherapy, while chemical cautery with trichloracetic acid tends to produce less scarring.
Actinic Keratosis
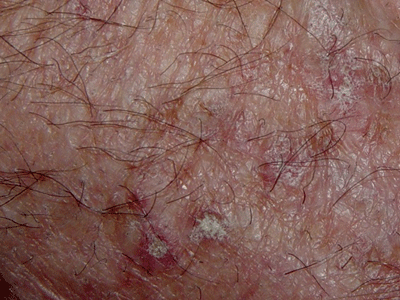
Actinic keratosissometimes called solar keratosisis associated with chronic sun exposure and is commonly encountered in patients past age 50 who have fair skin. Clinically, the keratoses usually appear as nondescript, reddish-brown scaly patches in sun-exposed areas of the hands and face and range from 3mm to 10mm in diameter. Actinic keratoses are significant because they are recognized precursors of squamous cell carcinomaa highly malignant form of skin cancer.
Isolated actinic keratoses may be treated with cryotherapy or curettage. However, because these le-sions are often widespread and insidious, topical therapy of a large surface area is generally preferred. Efudex (fluorouracil 5% cream, Valeant Pharmaceuticals) an antineoplastic antimetabolite that interferes with DNA synthesis, is the most common agent used to treat actinic keratosis. Applied to the skin, fluorouracil causes an inflammatory reaction within actinic keratoses, even those keratoses that cannot be visualized by the naked eye. The lesions become red and inflamed. Over time, this skin sloughs and is replaced by healthy tissue.
 |
|
Actinic keratosis responds well to topical therapy with the antimetabolite 5-fluorouraci. |
Basal Cell Carcinoma
Basal cell carcinoma (BCC) is the most common malignancy to affect the eyelids and ocular adnexa.5 The nodular and ulcerative varieties of BCC are most prevalent, appearing as raised, translucent or pearly areas with poorly defined borders. Common findings include overlying telangiectatic vessels, central atrophy, crusting or bleeding.
A less common superficial BCC may also be encountered. This presents as a scaly pinkish or reddish-brown patch, occasionally with a clear central area.
Overwhelmingly, the treatment for BCC is surgical. The Mohs micrographic techniquea tissue-sparing, frozen section controlled procedureis the preferred method for this and other cutaneous malignancies.
However, recent use of topical agents for localized BCC has yielded intriguing results. Both Aldara and Efudex are indicated for the treatment of superficial BCC. A recent report showed Aldara to be effective in two cases of periocular nodular BCC.2
Photodynamic therapy (PDT) using Metvix (methyl aminolevulinate 16.0% cream, PhotoCure ASA) is another non-invasive therapy that has shown promise for difficult-to-treat BCC. Metvix, which is currently only approved in the United States for actinic keratosis, induces tumor destruction through phototoxicity in light-exposed cells. This is similar to the mechanism used by Visudyne (verteporfin, Novartis Ophthalmics) in the treatment of subretinal neovascular membranes. Studies have shown that PDT with Metvix is rapid, effective and cosmetically superior to surgery for BCC.4,6
Awareness of both established and new therapies will enable you to provide your patients who have lumps and bumps with the most up-to-date and effective care, allowing them to once again feel comfortable in their own skin.
1. Brannan PA, Anderson HK, Kersten RC, Kulwin DR. Bowen disease of the eyelid successfully treated with imiquimod. Ophthalmol Plast Reconstr Surg 2005 Jul; 21(4):321-2.
2. Blasi MA, Giammaria D, Balestrazzi E. Immunotherapy with imiquimod 5% cream for eyelid nodular basal cell carcinoma. Am J Ophthalmol 2005 Dec; 140(6):1136-9.
3. Bergman R. Xanthelasma palpebrarum and risk of atherosclerosis. Int J Dermatol 1998 May; 37(5):343-5.
4. Gladstone GJ, Myint S. Xanthelasma. In: Fraunfelder FT, Roy FH, eds. Current Ocular Therapy, 5th Edition. Philadelphia: W.B. Saunders, 2000. 452-3.
5. Allali J, DHermies F, Renard G. Basal cell carcinomas of the eyelids. Ophthalmologica 2005 Mar-Apr;219(2):57-71.
6. Vinciullo C, Elliott T, Francis D, et al. Photodynamic therapy with topical methyl aminolaevulinate for difficult-to-treat basal cell carcinoma. Br J Dermatol 2005 Apr; 152(4):765-72.

