Known primarily for use in cosmetic surgery, botulinum toxin, better known as Botox, enjoys growing popularity in eye care as a therapeutic agent. The toxins ability to cause denervation in unwanted muscle function makes it an intriguing option in cases of focal dystonia and other ophthalmic or neurologic disorders in which traditional therapies are of limited benefit.
In studies of patients who receive a botulinum toxin injection for ophthalmic or neurologic disorders, 69% to 100% demonstrate clinically significant improvement.1,2 Some of the most exciting work in this field occurs with patients who suffer from migraine, tension-type and chronic headaches; many respond positively to this treatment.
Here, well discuss the basics of botulinum toxin therapy, its clinical uses and contraindications, and patient management.
Potent Neurotoxin
Botulinum toxin is the most potent biologic neurotoxin known to man. As the causative agent of botulism, a potentially fatal condition that causes neuromuscular paralysis, botulinum is high on the list of possible bioterrorism attack methods.
In clinical settings, however, the doses of the poison are too small to constitute any sort of biohazard, and no special security precautions are necessary or mandated by law.
Botulinum toxin is produced by the bacteria Clostridium botulinum. There are seven serotypes of the toxin; five of these are effective at the human skeletal neuromuscular junction. There, the toxin induces paralysis by blocking the release of acetylcholine, the chemical that carries information between nerve cells. Thus, it inhibits the transmission of nerve impulses across the synaptic junction to the motor end plate.
Botulinum toxin enzymatically inactivates the proteins necessary for the synaptic vesicles to fuse into the neuromuscular junction. Once injected, the toxin rapidly and firmly binds at receptor sites on the acetylcholine-related nerve terminals. Neuromuscular transmission ceases, and the target muscle atrophies. But, the resulting localized muscle weakness does gradually reverse over time.
The botulinum toxins effect is usually seen two or three days following injection, with maximal effect occurring at approximately two weeks. This corresponds to the amount of time required for the toxin to bind to the motor nerve terminal, undergo internalization and block acetylcholine.
Recovery takes six to 14 weeks, depending on the specific serotype used, and occurs with the proliferation of new axonal nerve buds to the denervated muscle and the regeneration of muscle end plates. This regeneration develops a functional connection at the muscle-nerve junction and reactivates muscle activity.
Clinical Use
In 1973, botulinum toxin was first shown to be efficacious and safe when used to weaken extraocular muscles. It is beneficial in patients who have horizontal or vertical strabismus, infantile esotropia, acquired misalignment in thyroid ophthalmopathy, acquired nystagmus (to dampen the resulting oscillopsia), dissociated vertical deviation, sensory strabismus, paradoxical diplopia, and postsurgical over- and undercorrections.3,4
When treating strabismus, botulinum is used to cause temporary paresis of one extraocular muscle. This results in a permanent change in the antagonist muscle after the paresis has worn off. So, in esotropia, when the medial rectus muscle is injected, its temporary weakening allows the antagonist lateral rectus muscle to shorten and tighten.
When the medial rectus recovers, the increased stiffness of the lateral rectus realigns the eye in an improvedor even straightposition. With exotropia, injection of the lateral rectus likewise allows the medial rectus to tighten.
The advantages of using botulinum toxin to treat strabismus: its ease of administration, the use of a topical anesthetic, little or no postinjection discomfort, and the absence of postoperative recovery time. Recovery is unnecessary, since no surgical incision or residual scarring occurs. Instead, the technique used in electromyography is employed to position the needle precisely into the belly of the extraocular muscle.
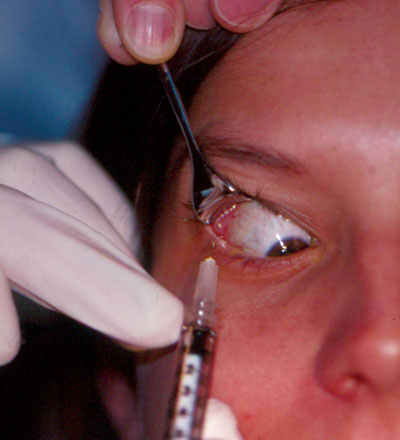
1. A transconjunctival injection directly into the lacrimal gland will temporarily eliminate excessive lacrimation (crocodile tears).
Botulinum toxin has many other applications. It may be used to induce a protective ptosis in cases of corneal compromise or ulceration in patients who have fifth or seventh cranial nerve palsies. Advantages of this chemical tarsorrhaphy, of sorts: The eyelid can be easily opened for instillation of medication or ocular examination, and there is no need for eyelid taping or suturing.
Upper eyelid retraction, often seen in thyroid eye disease, can be successfully treated by transcutaneous injection of botulinum toxin between the orbital roof and the levator palpebrae superioris muscle. Or, it can be treated via the transconjunctival route if the levator and Mllers muscles are injected.
Additional uses for botulinum toxin include:
A spastic and inwardly turned lower eyelid that has caused entropion. This can be treated by an injection into the orbicularis oculi muscle.
Aberrant movements due to facial nerve misdirection. These movements, as seen in patients with Bells palsy, can be treated by injecting the toxin into the affected muscles.
Aberrant regeneration that causes excessive lacrimation with chewing (crocodile tears). A transconjunctival injection directly into the lacrimal gland will temporarily eliminate the tearing (figure 1).5
Mild to moderate upper eyelid dermatochalasis. Botulinum toxin has proven effective for treating this condition following lateral infrabrow injection.6
Surgical facial wounds. The toxin is now being used to relieve tension in wounds by inducing immobilization of the adjacent musculature. This provides enhanced healing and improvement in the appearance of the resulting scar.7
Neurologic uses. Beyond its traditional role in muscle chemo-immobilization, new uses are emerging, such as control of the neuropathic pain of patients with post-herpetic neuralgia.8 Theoretically, botulinum toxin should inhibit peripheral and central sensitization by blocking the release of both acetylcholine for neuromuscular transmission and nociceptive (pain-transmitting) neuropeptides involved in the chronic inflammatory pain response.9-11
This mechanism has been put forth as the basis for its effectiveness in treating forms of headache. Migraine, tension-type, cervicogenic, cluster and chronic daily headaches have all responded favorably to botulinum toxin therapy.9-11
Dystonias
Perhaps the most popular use of this therapy is for dystonias of the face and neck. Dystonia is a syndrome dominated by involuntary sustained (tonic) or spasmodic (rapid or clonic), patterned, repetitive muscle contractions.
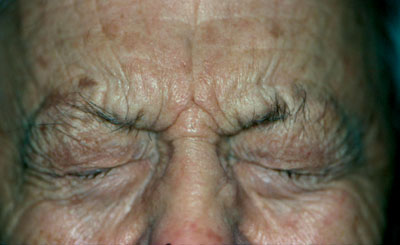
These contractions frequently cause twisting, flexing, extending and squeezing movements, or in some cases, abnormal postures. For example, benign essential blepharospasm (BEB), a common bilateral facial dystonia, involves the orbicularis oculi muscles and the procerus and corrugator musculature (figure 2). It usually occurs between ages 50 and 70 (mean age 56), and women with BEB outnumber men by three to one.12,13
BEB starts as variable episodes of increased blinking, progresses to involuntary spasms of eyelid closure, and can result in functional blindness in up to 12% of patients.12,13
BEB may be exacerbated by stress, fatigue, reading, bright sunlight or driving (especially the oncoming headlights of night driving). On the other hand, activities such as sleeping, relaxing, walking or talking and behavioral techniques and mannerisms (humming, singing, whistling, tapping the temple, solving puzzles or mathematical problems) can reduce the frequency and severity of the spasms.
2. Benign essential blepharospasm, a common bilateral facial dystonia, involves the orbicularis oculi muscles and the procerus and corrugator musculature.
When BEB is associated with intermittent lower facial movement, the disorder is known as Meige syndrome. These patients exhibit BEB with lip pursing, tongue protrusion, trismus (lockjaw) and speech difficulty. If the mandible is involved, then the patient has Brueghel syndrome. Blepharospasm is the central feature of both Meige and Brueghel syndromes.
Apraxia of lid opening (ALO) is a condition in which patients who have otherwise normal eyelids have difficulty opening their eyes at will. They raise their eyebrows (forceful contraction of the frontalis muscle) in an effort to raise their eyelids. ALO can coexist with BEB in the same patient, and in patients who have both disorders, a combination of therapiessuch as blepharoplasty, myectomy or aponeurosis repair in tandem with botulinum toxin injectionsappears to be the most effective approach.
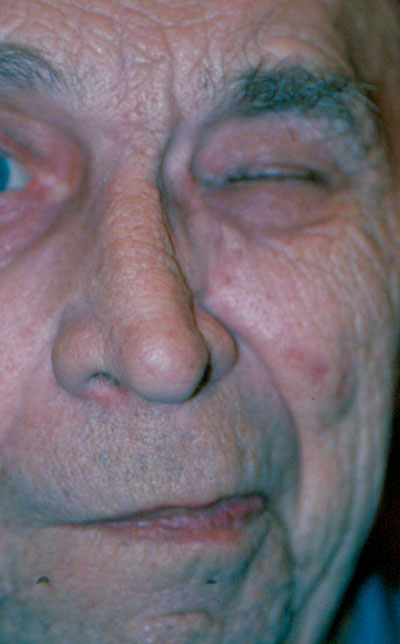
Hemifacial spasm is characterized by unilateral, periodic, tonic contractions of the facial muscles used in expression (figure 3). This condition occurs in middle-aged individuals and is more common in women. The cause of hemifacial spasm is most often microvascular compression or irritation of the facial nerve by an aberrant artery in the posterior fossa. However, because a cerebellopontine tumor may also be the cause, these patients must undergo magnetic resonance neuroimaging.
The use of botulinum toxin to treat torticollis, an involuntary dystonic posturing of the neck and head, differs from treatment of BEB and hemifacial spasm in several significant ways. First, a much higher dose is administered, resulting in a significant risk of local and distant spread of toxin. Second, the condition involves more muscles, some less accessible due to their location deeper in the neck. There is greater risk of diffusion into the pharyngeal musculature, which can result in dysphasia. Finally, aspiration, inability to maintain a patent airway, injection into the carotid artery or jugular vein, and neck laxity are other unique risks.
Use of an electromyographic needle for injection helps to ensure that the agent remains in the affected muscle (figure 4). The use of such a needle is unnecessary when treating BEB or hemifacial spasm.
Two Types of Toxin
There are currently two types of botulinum toxin available commercially in the
3. Hemifacial spasm is characterized by unilateral, periodic, tonic contractions of the facial muscles used in expression.
Botox is available in vials of 100 units in a powder form, and its manufacturer recommends hydrating the powdered toxin with sterile 0.9% nonpreserved saline. The saline must be injected slowly into the vacuum-sealed vial to prevent frothing or agitation, since mechanical disruption can cause toxin inactivation. Because this agent can deteriorate quickly after being reconstituted, it should be used within four hours.14
Although not recommended by the manufacturer, refrigeration of reconstituted Botox has been shown to maintain product potency for up to two weeks.15
The clinician determines the final concentration of the reconstituted Botox. The most commonly used dilution is 2.5 units per 0.1ml of volume at each injection site. To obtain this dosage, 4ml of saline is injected into the Botox vial, resulting in a concentration of 2.5 units/0.1 ml. Of that, 0.1ml or 0.2ml is typically administered at each treatment site.
Myobloc comes premixed in a clear, colorless-to-light yellow sterile solution. It is available in three dosing volumes: 2,500units/0.5 ml; 5,000 units/1 ml; and 10,000 units/2 ml. It remains stable under refrigeration for up to 21 months.12
Myobloc exists at a pH of 5.6 when in aqueous solution; this relatively acidic pH may cause increased discomfort during injection for some patients.16 Unlike Botox, which has an average therapeutic duration of 14 weeks, Myobloc has been shown to maintain its therapeutic effect for as little as six weeks.16
Complications
Because botulinum toxin binds quickly and tightly, there is little risk of the toxin entering the circulatory system. Poor injection technique or overdosage leads to the majority of complications, which generally stem from local spread of the agent to muscle tissue not intended for treatment.
After injection, blepharoptosis may develop in the upper eyelid or the glabellar region. Patients who have an abnormal orbital septum are particularly susceptible to this complication, due to penetration of the medicine into the levator palpebrae superiorus muscle. If eyelid ptosis occurs from an errant injection, a temporary lift can be achieved with Iopidine (apraclonidine, Alcon) drops. This agent stimulates Mllers muscle, providing an elevation of about 2mm.
Patients who undergo injection in the lower eyelid will experience paralytic ectropion if they have pre-existing horizontal laxity and impending involutional ectropion. This complication can lead to postoperative complaints of tears spilling onto the medial cheek.
4. Use of an electromyographic needle for injection helps to ensure that the agent remains in the affected muscle.

Too large a dose on the orbicularis oculi musculature may result in corneal compromise. Blink rate could then decrease, resulting in lagophthalmos. Also, some patients report drooling and/or biting the inside of their mouths for a short period post-injection. This indicates that excessive medication was placed in the cheek area, the nasal labial fold or the corner of the mouth.
Another potential error: injection of the toxin inside the bony orbital margin too near the origin of the inferior oblique muscle at the infraorbital rim. This can lead to paresis of the inferior oblique muscle and vertical diplopia.
Other reported side effects include flu-like symptoms, headache, respiratory infection, nausea, pain and ecchymosis (bruising). Bruising occurs most frequently in older patients who take aspirin, nonsteroidal anti-inflammatory agents, Coumadin (warfarin, Bristol-Myers Squibb), vitamin E or gingko biloba.
Contraindications
Prior to using botulinum toxin, some well-established contraindications must always be observed. Botulinum toxin should not be used in patients who have neuromuscular disorders, such as myasthenia gravis, Lambert-Eaton syndrome or amyotrophic lateral sclerosis (ALS, or Lou Gehrigs disease).
Likewise, patients who use or may be exposed to certain medications should be excluded. These include the aminoglycoside antibiotics (gentamycin, streptomycin); drugs used during anesthesia (succinylcholine); antimalarials (chloroquine, hydoxychloroquine) and D-penicillamine, which is used to treat rheumatoid arthritis.
Botulinum toxin also is not recommended for pregnant women or nursing mothers, nor should injection occur in areas in which the overlying skin shows signs of infection or inflammation. Because Botox and Myobloc both contain human serum albumin to stabilize the active ingredient, those allergic to eggs should not receive this agent.
O.D.s should consider injections of botulinum toxin when they encounter patients who suffer from the conditions described above. Botulinum toxin offers many advantages over traditional surgery. Patients may be familiar with the toxins use in cosmetic surgery, so there is less chance of anxiety about its ophthalmic applications. Often, patients will thank you for steering them in the right direction.
Dr. Skorin is the staff ophthalmologist at Albert Lea Eye Clinic-Mayo Health System,
1. Botulinum toxin therapy of eye muscle disorders. Safety and effectiveness.
2. Assessment: the clinical usefulness of botulinum toxin-A in treating neurologic disorders. Report of the Therapeutics and Technology Assessment Subcommittee of the
3. Crouch ER. Use of botulinum toxin in strabismus. Curr Opin Ophthalmol 2006 Oct;17(5):435-40.
4. Helveston EM, Pogrebniak AE. Treatment of acquired nystagmus with botulinum A toxin. Am J Ophthalmol 1988 Nov 15;106(5):584-6.
5. Montoya FJ, Riddell CE, Caesar R, Hague S. Treatment of gustatory hyperlacrimation (crocodile tears) with injection of botulinum toxin into the lacrimal gland. Eye 2002 Nov;16(6):705-9.
6. Cohen JL, Dayan SH. Botulinum toxin type A in the treatment of dermatochalasis: an open-label, randomized, dose-comparison study. J Drugs Dermatol 2006 Jul-Aug;5(7):596-601.
7. Gassner HG, Brissett AE, Otley CC, et al. Botulinum toxin to improve facial wound healing: a prospective, blinded, placebo-controlled study. Mayo Clin Proc 2006 Aug;81(8):1023-8.
8. Liu HT, Tsai SK, Kao MC, Hu JS. Botulinum toxin A relieved neuropathic pain in a case of post-herpetic neuralgia. Pain Med 2006 Jan-Feb;7(1):89-91.
9. Mauskop A. The use of botulinum toxin in the treatment of headaches. Pain Physician 2004 Jul;7(3):377-87.
10. Anand KS, Prasad A, Singh MM, et al. Botulinum toxin type A in prophylactic treatment of migraine. Am J Ther 2006 May-Jun;13(3):183-7.
11. Silberstein SD, Gobel H, Jensen R, et al. Botulinum toxin type A in the prophylactic treatment of chronic tension-type headache: a multicentre, double-blind, randomized, placebo-controlled, parallel-group study. Cephalalgia 2006 Jul;26(7): 790-800.
12. Skorin L. Spasms, twitches and other eyelid glitches. Clin Refract Optom 2006; 17: 14-25.
13. Patel BC, Anderson RL. Essential blepharospasm and related diseases. Focal Points Clinical Modules for Ophthalmologists.
14. Physicians Desk Reference, ed 59.
15. Sloop RR, Cole BA, Escutin RO. Reconstituted botulinum toxin type A does not lose potency in humans if it is refrozen or refrigerated for 2 weeks before use. Neurology 1997 Jan;48(1):249-53.
Ophthalmology 2000;18:1-13.
16. Ramirez AL, Reeck J, Maas CS. Botulinum toxin type B (MyoBloc) in the management of hyperkinetic facial lines. Otolaryngol Head Neck Surg 2002 May;126(5):459-67.
17. Moriarty KC. Botulinum Toxin in Facial Rejuvenation.

