 Q. I have a patient with a non-healing epithelial defect. What are my options?
Q. I have a patient with a non-healing epithelial defect. What are my options?
A. First, be sure you know what you’re dealing with. “Initially, be concerned if a correct diagnosis has been missed—such as with a parasitic or viral infection—and that’s the reason for the non-healing defect,” says corneal surgeon Rishi Parikh of Omni Eye Services, in Atlanta. “However, if this is not the case, then it is most likely a neurotrophic ulcer.
”First-line treatment for a neurotrophic ulcer is aggressive lubrication with preservative-free artificial tears and a bandage contact lens, Dr. Parikh says. Punctal plugs can also help with lubricating the eye. In addition, he says, discontinue any unnecessary drops because these could be toxic to the cornea and delay healing. “This approach helps heal the majority of cases. But be patient, as these heal much more slowly than a typical epithelial defect.” Occasionally, the defect remains despite this treatment. Options for a stubborn, non-healing defect include:
• Autologous serum drops. Autologous serum, which is created from the patient’s blood serum, contains growth factors, fibronectin and vitamins that support proliferation, migration and differentiation of the corneal and conjunctival epithelium. The drops have been found to be extremely useful in persistent epithelial defects and severe dry eye.1
“There is no standard regimen to use the drops, so it is generally titrated to the percentage and drop frequency based on the healing of the defect,” says Dr. Parikh. Unfortunately, it can be difficult to find a lab and compounding pharmacy that will make the drops for the patient. And, even when the drops are made, they may not be covered by insurance and will probably be fairly expensive, he says.
• Amniotic membrane graft (AMG). Harvested from placental tissue after a cesarean section, an AMG provides vital cytokines and growth factors that work to repair and regenerate the damaged ocular surface tissue of an epithelial defect. AMGs have also been used for many other purposes with good results, such as with filamentary keratopathy to more severe cases of Stevens-Johnson syndrome and severe chemical burns.2
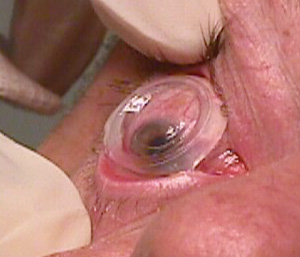 |
| A ProKera amniotic membrane graft is applied to an epithelial defect. A growing number of ODs are being reimbursed for this procedure.
|
Once the defect has healed, follow-up visits can be slowly extended out. When the patient returns to the optometrist, monitor for any early signs of dry eye such as punctate keratitis or complaints of foreign body sensation, Dr. Parikh says. If these signs occur, increase the frequency of the artificial tears and treat aggressively to prevent a new ulcer from forming.“
The best way to prevent the defect from occurring again is with aggressive lubrication with preservative-free tears and ointments,” Dr. Parikh says. Also consider permanent punctal plugs, and if autologous serum drops worked previously, maintenance serum drops can help prevent a subsequent occurrence. If this regimen fails and a recurrence occurs, surgical options—such as a lateral tarsorrhaphy or conjunctival flap—can be considered.
1. Tsubota K, Goto E, Shimmura S, Shimazaki J. Treatment of persistent corneal epithelial defect by autologous serum application. Ophthalmology. 1999 Oct;106(10):1984-9.2. Ricardo JR, Barros SL, Santos MS, et al. Amniotic membrane transplantation for severe acute cases of chemical ocular burn and Stevens-Johnson syndrome. Arq Bras Oftalmol. 2009 Mar-Apr;72(2):215-20.

