Q: I recently fit a large-diameter scleral lens (18mm) on a moderately severe keratoconus patient with adequate central clearance, but the lens decenters inferiorly. It seems to be creating some comfort issues (awareness and reduced wearing time). Any suggestions for the next lens change?
 |
|
|
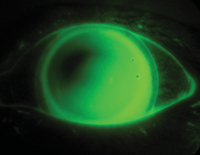
The superior nasal tear film thinning (dark fluorescein) appears due to higher elevation superiorly and nasally. The lens decenters inferiorly and temporally in this patient.
|
![]() A: Before changing lenses, you need to figure out the reason for the decentration, which is likely one of these two causes: the lens may have excess mass or vault, or the patient’s sclera is toric.
A: Before changing lenses, you need to figure out the reason for the decentration, which is likely one of these two causes: the lens may have excess mass or vault, or the patient’s sclera is toric.
Lens Mass/Vault
“Inferior lens decentration could be attributed to lens mass and bearing of the upper lid,” explains Greg DeNaeyer, OD, clinical director of Arena Eye Surgeons in Columbus, Ohio. Also, because the patient is complaining of discomfort with a decentered scleral lens, it’s likely that lens bearing on the superior nasal quadrant may be causing epithelial erosion, Typically, erosion will show up as staining under slit-lamp examination after lens removal.
Dr. DeNaeyer suggests several solutions to help alleviate the irritation. First, “increase the overall vault of the lens by steepening the base curve and/or mid-peripheral curves. This will take lens bearing off of the superior nasal cornea,” he says.
On the other hand, make sure you don’t have too much vault. “The more the lens lifts away from the eye, the greater the lid pressure on the lens,” says Jason Jedlicka, OD, from the Cornea and Contact Lens Institute of Minnesota in Edina. So, “decreasing the vault will reduce the lid pressures that drive the lens lower.” Of course, he adds, this can only be done if there is already more than enough vault to begin with.
Another possible method, says Dr. DeNaeyer, is to piggyback the scleral lens on top of a soft lens, which acts as a cushion between the area of bearing and the lens. A daily disposable is best suited for this method, and those made of silicone hydrogel in particular should be considered to achieve the greatest possible oxygen transmissibility. Switching the patient to hybrid lenses or specialty soft lenses may also aleviate the problem.
Reducing the lens mass could also help ease discomfort and decentration. To decrease the mass, Dr. Jedlicka suggests trimming the lens thickness, which would lower “the effect of gravity on the lens as well as the lid pressures on the lens.” However, make sure that decreasing the lens thickness does affect other aspects of the fit or cause other problems, such as flexure.
Alternatively, try a small-diameter scleral lens such as a 16mm mini-scleral. “The decrease in mass will often help to minimize decentration,”Dr. DeNaeyer says.
Toric Sclera
Aside from excessive lens vault and lens mass, another potential cause of inferior decentration could be toricity of the sclera.
“If the sclera is flatter along the 3 and 9 o’clock meridian,” Dr. Jedlicka explains, “the lens will not be able to sit on that meridian.” Displacement often results. “Unlike a corneal GP—which will often ride high with the lid—the scleral lens will instead settle inferiorly,” Dr. Jedlicka says.
Typically, he adds, this can be recognized through the observation of “tight fit/compression along the horizontal meridian and a looser fit in the vertical meridian.”
In these cases, switching the patient to a lens with a toric haptic can help with centration issues. Alternatively, lens diameter can be decreased to lessen the impact of toricity.

