 |
Q: In which cases would you still use a corneal gas permeable (GP) lens, rather than a scleral lens, to fit an irregular cornea with ectasia?
A: “Corneal GP lenses were the standard of care for over 50 years in [cases of] corneal ectasia and keratoconus,” says Jeffrey Sonsino, OD, of Optique Eyecare in Nashville, Tenn. Recent research, however, including the Collaborative Longitudinal Evaluation of Keratoconus (CLEK) studies, changed that benchmark. “[Following the studies,] we agreed that flat-fitting GP lenses were associated with higher risk of corneal scarring, which ultimately led to corneal transplant. In fact, around 40% of keratocones are still undergoing some form of either partial thickness or penetrating keratoplasty,” explains Dr. Sonsino.1-3
Newer vaulting lenses (i.e., sclerals and hybrids) alleviate this problem by offering a safer apical clearance type fit; they are expected to significantly reduce the prevalence of corneal transplants among patients.
That being said, corneal GP lenses still maintain an important role for managing keratoconus, despite the advantages of scleral lenses, says Gregory DeNaeyer, OD, of Arena Eye Surgeons in Ohio. “Corneal GP lenses center where the cornea is steep and therefore can be ideal for nipple topographies that have centered apices,” he explains. Patients with small apertures and deep-set eyes may also benefit from corneal GP lens wear, as these physical characteristics can impede success of a scleral lens fit.
Christine W. Sindt, OD, of the University of Iowa, points out that corneal GP lenses also offer higher tear exchange than scleral lenses, so patients with lid colonization or inflammatory product build-up may benefit from the reduced risk of infection. Additionally, significant scleral irregularity or toricity may make scleral lens use impossible, she adds.
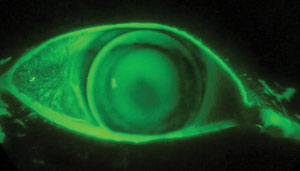 | |
| Corneal gas permeable lenses offer keratoconic patients a range of benefits despite their irregular corneal topography. Photo: Gregory DeNaeyer, OD. |
Cost factors must also be considered when selecting a lens: GP lenses are significantly less expensive than scleral lenses.
If maintaining endothelial cell count is a concern, corneal GP lenses are preferable over scleral lenses, as the latter can result in corneal edema due to reduced oxygen permeability, says Dr. Sindt. Research shows that at five years following corneal transplant surgery, average endothelial cell counts are only 786 cells/mm2, Dr. Sonsino notes.4
In closing, Dr. DeNaeyer offers some additional advice regarding stabilizing corneal GP lenses on these types of patients: fit corneal GP lenses with diameters larger than 9.5mm and consider piggybacking corneal GP lenses on a soft disposable lens for better comfort.
1. Keenan TD, Jones MN, Rushton S, et al. Trends in the indications for corneal graft surgery in the United Kingdom: 1999 through 2009. Arch Ophthalmol. 2012 May;130(5):621-8.2. Coster DJ, Lowe MT, Keane MC, et al. A comparison of lamellar and penetrating keratoplasty outcomes: a registry study. Ophthalmology. 2014 May;121(5):979-87.
3. Frigo AC, Fasolo A, Capuzzo C, et al. Corneal transplantation activity over 7 years: changing trends for indications, patient demographics and surgical techniques from the Corneal Transplant Epidemiological Study (CORTES). Transplant Proc. 2015 Mar;47(2):528-35.
4. Lass JH, Gal RL, Dontchev M. Donor age and corneal endothelial cell loss 5 years after successful corneal transplantation. Specular microscopy ancillary study results. Ophthalmology. 2008 Apr:115(4):627-32.

