Annual Diagnostic Skills and Techniques IssueFollow the links below to read other articles from our update on diagnostic skills and techniques: |
Neuro-ophthalmic disease is often daunting for eye care practitioners, considering it can present with abnormalities in any part of the examination, and with features overlapping with many other ocular and systemic conditions. ODs don’t want to unnecessarily refer patients, but they also don’t want to miss a potentially serious or life-threatening condition.
Some of the reasons for unnecessary referrals to neuro-ophthalmic disease specialists include uncorrected or inaccurately corrected refractive error, uncorrected presbyopia, dry eye disease (DED), meibomianitis and hypoplastic or anomalous optic discs.
Necessary referrals are often missed when patients are asymptomatic or present with an early or mild form of a condition. Issues can also be overlooked when the provider does not perform a complete assessment or fails to correlate the constellation of signs and symptoms with a neuro-ophthalmic process.
Navigating where patients fall on this imaginary, and often blurred, line between a common presentation and a medical emergency can be challenging. Every presentation is unique, and clinicians must use their history-taking skills and clinical acumen to determine the appropriate level of concern for each patient.
All ODs should be familiar with neuro-ophthalmic presentations, because patients don’t know when they need a neurologist or a neuro-ophthalmic disease specialist—they rely on their trusted eye care provider to tell them when it’s necessary.
Here are some helpful hints—based on years of experience—to consider when dealing with a potential neuro-ophthalmic disease case. While not a comprehensive review of all the responsibilities and presentations one may encounter, it includes some pitfalls to avoid.
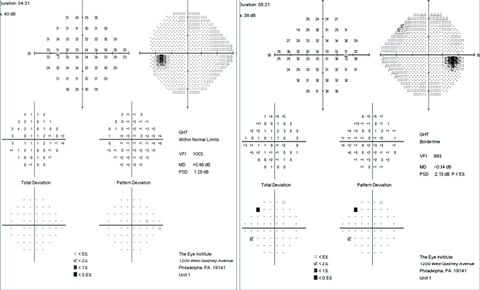 |
| Case 1. This 51-year-old woman presented with a complaint of daily right-sided head and eye pain, as well as worse vision in the right eye. Her VFs were normal with no RAPD. All other aspects of her afferent and efferent visual function were intact. Despite wearing progressive lenses, her vision was reduced more so at near than at distance in the right eye compared with the left eye. Careful refraction found that she was over-minused by 1.00D in the right eye. With the new prescription trial-framed, she felt her eyes were more relaxed and her vision was comfortable and symmetric. Click images to enlarge. |
Everyone’s a Suspect
Clinicians should always consider that every patient might have a neuro-ophthalmic disease process. While this is obvious for patients who present urgently with symptoms such as diplopia or sudden vision loss, clinicians should also be on the lookout for a neuro-ophthalmic disease process even in patients presenting for routine eye care without any specific complaints. It is important to fully assess the ocular health status in all patients. The combination of afferent and efferent visual function tests will help uncover an abnormality (Table 1).1,2
Table 1. Visual Function Tests | |
| Afferent | Efferent |
|
|
Not Always Cause for Alarm
Often, a routine exam can explain symptoms and help avoid unnecessary referrals. Some common, and often unspecific, signs and symptoms can be easily explained without the need for additional referral:
Frontal headaches and eye pain. Patients frequently present with headaches or eye pain that initially seem unexplained. However, careful consideration can minimize the need for neuroimaging or a neuro-ophthalmology consultation. A careful refraction is crucial, especially in younger patients, because seeing 20/20 doesn’t necessarily mean the patient is properly corrected. Patients are often referred for eye pain and frontal headaches, and the etiology is uncorrected hyperopia or over-minused myopic patients—symptoms are due to over accommodation. In patients with such complaints, be sure to fully relax the eyes before refining the refraction.
Basic refractive techniques, including initial maximum plus to maximum visual acuity and binocular balance, are essential, especially in pre- and early presbyopic patients. Always consider the potential for latent hyperopia in patients with unexplained eye pain and frontal headaches. Perform a cycloplegic refraction before considering additional workup or referral (Case 1).
Blur or transient vision loss. Patients complaining of nonspecific eye pain and blurry vision sometimes have DED, meibomianitis or both. Patients with these conditions may complain of what sounds like episodes of transient vision loss. Here, a detailed history is key. If the symptoms are related to DED, the patient typically reports that the episodes of vision loss last a few seconds and are relieved with blinking or use of a lubricating drop. A true episode of transient vision loss represents a transient ischemic attack and should be treated as a medical emergency—the patient should go to the hospital immediately for neuroimaging to rule out stroke.3,4
Visual field (VF) loss. Patients with significant DED may perform poorly on a formal VF due to ocular irritation and reduced blinking during the test. This often becomes more problematic as the test progresses, and they may do more poorly on the second eye tested. If it is truly a neuro-ophthalmic disease process, they should have a corresponding relative afferent pupillary defect (RAPD) in the eye that performed more poorly on the VF.5,6 Prior to performing a VF, patients with DED should instill lubricating drops. Also, make sure the patient understands they are allowed to blink normally during the test.
Eyelid edema or ptosis. Heavy eyelids that appear droopy may be a true ptosis or an anterior segment issue. Feel the upper lid margin for fullness suggestive of meibomianitis, and ask the patient if they have a stringy discharge in the medial canthus upon awaking. Even without visually blocked glands on the lid margins, try to manually express the glands. If you are unable to express a clear secretion, consider meibomianitis as a diagnosis. Meibomianitis is more likely to be a bilateral process, whereas some of the most concerning neuro-ophthalmic causes of ptosis such as cranial nerve (CN) III palsy and Horner’s syndrome tend to be unilateral. Myasthenia gravis can present with unilateral or bilateral ptosis. However, myasthenic ptosis is fatigable, so remember to test for worsening of the ptosis after two minutes of upgaze and test for improvement of the ptosis after two minutes of ice application. These would both be suggestive of myasthenia gravis.
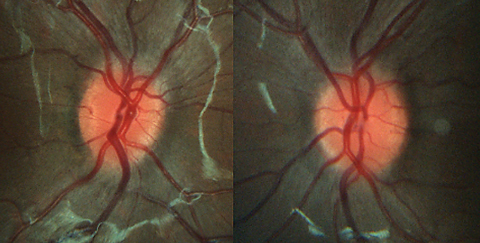
 |  |
 |  |
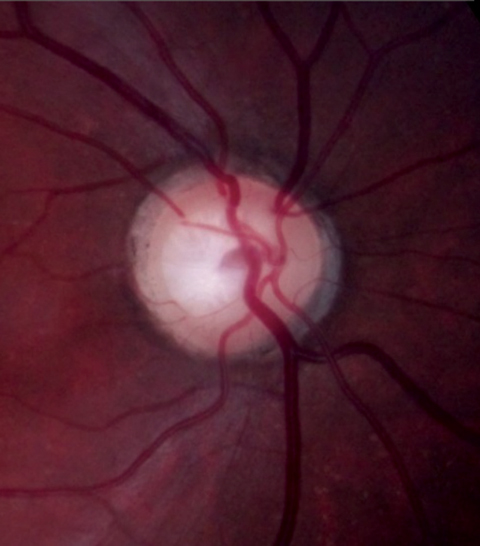
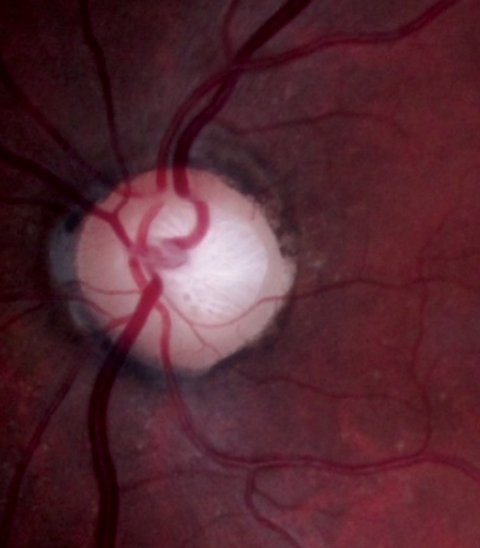
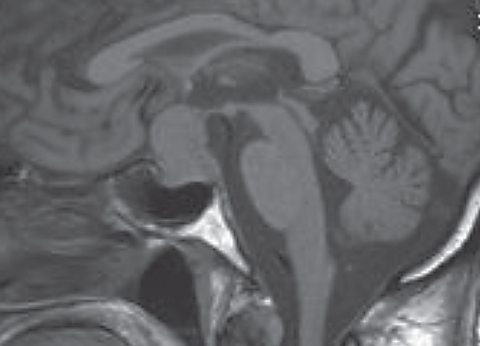 | Case 2. This 73-year-old man was being treated for glaucoma. However, his optic discs demonstrated diffuse neuroretinal rim pallor. In addition, his VF loss was only temporal and respected the vertical meridian, which is not consistent with glaucoma and more concerning for a sellar mass. Neuroimaging demonstrated a pituitary macroadenoma. |
Top 10 Neuro Tips
Some of the most common issues overlooked are mild papilledema, optic neuropathy, ocular misalignment, Horner’s syndrome and nystagmus. Several neuro-ophthalmic processes are medical emergencies and, when suspected, patients should be sent directly to the emergency department for immediate testing and treatment (Table 2). These 10 tips can help you get to the bottom of your patient’s concerns and manage their care properly:
1. Take a detailed history. Office staff should be prepared to triage phone calls about the need for urgent appointments. To avoid a delayed evaluation of a potentially emergent situation, clinicians must be aware of every call for an urgent or emergent appointment.
As the first step of any appointment, urgent or not, a detailed history should not be rushed. A few extra minutes in the beginning of the exam can provide a better sense of what is going on and avoids the risk of missing something urgent, emergent or even life-threatening.
Do not limit your questions to the eyes, as patients rarely think it is important to mention non-ocular signs and symptoms; also, do not ignore symptoms already being managed by another specialist. Perform a full review of systems and take a thorough medical, surgical, family and social history. Some important considerations include: alcohol, drug and tobacco use; poor nutrition and changes in appetite or weight; a history of cancer; pregnancy or recent birth (changes in the pituitary gland can occur in these patients); and symptoms of giant cell arteritis in patients over age 50.
For patients with recent hospitalizations, blood tests or imaging studies, staff should obtain the reports, as well as those from the patient’s other doctors. Do not assume someone else is handling everything; use these reports to determine if the patient needs further testing, treatment or referral. Even if they do not yet have any visual symptoms, a thorough history may aid in the timely diagnosis of important systemic conditions such as giant cell arteritis, myasthenia gravis, multiple sclerosis or stroke, to name a few.
Table 2. Suspected Conditions That Need Immediate Referral to an Emergency Department | ||
| Condition | Signs and Symptoms | Required Testing |
| Giant cell arteritis | Patients over age 50, with possible headache, eye or other pain, scalp tenderness, temporal artery tenderness, diplopia, jaw claudication, fever, loss of appetite, weight loss, joint aches, arteritic anterior ischemic optic neuropathy, CN palsies, homonymous hemianopia or any other new onset neurologic deficit | STAT ESR, CRP, CBC, platelets |
| Aneurysm | CN III palsy complete or partial, with pain and/or pupil involvement | MRA, CTA and/or angiogram |
| Papilledema | Indistinct disc margins, obscuration of vessels at disc margin, peripapillary wrinkles (Paton’s lines), axoplasmic stasis – with or without other symptoms | Brain MRI with contrast and MRV to R/O mass or venous sinus thrombosis |
| Pituitary apoplexy | Bitemporal visual field loss, junctional scotoma, incongruous homonymous hemianopia, headache, nausea, vomiting, fever | Brain CT/MRI |
| Carotid artery dissection | Painful Horner’s syndrome: ptosis and miosis | MRA, CTA, angiogram |
| Acute stroke | Transient vision loss, branch retinal artery occlusion, central retinal artery occlusion, homonymous hemianopia, facial palsy, sudden weakness or numbness on one side of body, slurred speech, skew deviation, INO, gaze palsy | CT then MRI of brain, carotid, and hypercoagulable evaluation, thorough cardiac evaluation |
2. Check blood pressure. Abnormal or asymmetric (between arms) blood pressure, pulse or both could help you identify the etiology of the clinical presentation. You can make a difference in the patient’s overall health if you discuss the importance of medication compliance, call and get them back to their primary care physician or cardiologist if overdue, or send them to the emergency department if warranted by extremely abnormal results.
3. Explain any reduced visual acuity. Even a visual acuity of 20/25 could signify an early neuro-ophthalmic disease process. Therefore, clinicians must explain reduced visual acuities by media opacities, macular changes or other processes. The degree of media opacity must match the level of visual acuity—a mild cataract, for example, should not cause significant vision loss. Additionally, symmetric lens changes and worse visual acuity in one eye need further explanation. Do not assume keratoconus is the cause of reduced vision in patients with scissor reflexes or high astigmatism on retinoscopy; if they do not have corneal striae, edema or scarring to account for the vision loss, another cause is at play. If no clinical finding justifies the level of visual acuity, further neuro-ophthalmic workup or referral is warranted.
4. Get a VF—today. If visual acuity is reduced even mildly or if the patient has visual complaints, even in the setting of 20/20 vision, be sure to get a formal VF that day to better assess the afferent visual system. A VF can be instrumental in determining if an afferent problem exists, can localize a problem to the suprasellar cistern or occipital lobe and can be crucial in determining the urgency of the condition. A wait could delay an important diagnosis and treatment.
A disease of the arcuate nerve fibers, glaucoma should manifest with nasal steps and proximal or distal arcuate defects. A glaucoma patient who has greater field loss temporally than nasally needs neuro-imaging to rule out a suprasellar mass (Case 2).
VFs can help clinicians anatomically localize any potential disease process. Clinicians should also match the VF to both the optic disc appearance and the degree of RAPD—if they do not match, consider that the VF may be inaccurate and repeat the test. Sometimes it is difficult to ascertain if there is indeed pallor of the neuroretinal rim, especially in patients who are highly myopic or those who are status-post cataract extraction with intraocular lens implants. All tests of afferent visual function are necessary to see if they support a diagnosis of optic neuropathy. Color vision testing can be helpful here. RAPD assessment will also be crucial; if an RAPD is present, it can localize a defect to the portion of the visual pathway shared with the light reflex pathway. An RAPD, which localizes anterior to the lateral geniculate nucleus, should lead to suspicion of a problem with the optic nerve, chiasm or tract.
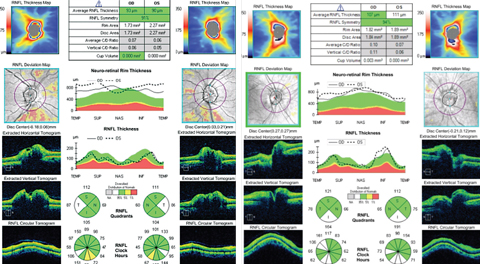 |
| Cases 3 and 4. Both of these patients demonstrate optic disc elevation as evidenced by a thick neuroretinal rim OU. However, the patient on the right is more concerning for papilledema due to the inferior RNFL thickening, as opposed to the temporal RNFL thickening in the patient on the left. In papilledema, the area of the disc that swells first is the one with the most nerve fibers, which is inferior. Since the thickness of the neuroretinal rim often follows the ISNT rule, it would be unlikely to have only the temporal RNFL thicker than normal in papilledema. Click images to enlarge. |
5. Assess for an RAPD. Always check pupil measurements yourself; do not delegate this task to a technician or student—and certainly do not dilate the patient before looking at the pupils. When assessing for an RAPD, be sure to use the proper endpoint—you are comparing the time to pupillary escape in each eye. An RAPD is present when asymmetry exists in this time to pupillary escape; the eye with the faster escape has the RAPD. Do not confuse the pupillary size to be a measure of an RAPD, as it is a measure of the efferent, not the afferent, visual system.
6. Measure pupils and eyelids. Measuring pupil sizes in both bright and dim illumination is necessary to assess for anisocoria. In addition, you must measure palpebral apertures to look for asymmetry. Do not approximate these measurements. When anisocoria is greater in dim illumination, or a pupil is smaller on the same side as the smaller palpebral aperture, consider Horner’s syndrome. If it is acute or associated with pain, emergent workup is warranted to rule out a carotid dissection. Otherwise, perform in-office apraclonidine testing to confirm or rule out the presence of Horner’s syndrome. Further referral and workup is warranted with a positive test—reversal of anisocoria within one hour after drop instillation.
If the pupils do not react well to a light stimulus, check the near reflex. A greater reaction to an accommodative target than to a light stimulus, or light-near dissociation, can be instrumental in making some important diagnoses, such as blind eye, tonic pupil, Argyll Robertson pupil, dorsal midbrain syndrome and aberrant regeneration of CN III.
You Are Not AloneWork together with the patient’s other doctors for the good of the patient. If you hear suspicious symptoms or see any abnormal findings, even if not eye-related, discuss them with the patient’s primary care physician, neurologist, emergency department doctor or other specialists involved in the patient’s care. Don’t be afraid to suggest a certain diagnosis that they have not yet considered, and be sure everyone is clear on who is taking the lead on ordering any necessary workup. Also, if you are referring the patient to a neurologist or neuro-ophthalmic disease specialist, communicate the reason for the referral. Supply them with the details of your examination so that, when they see the patient, they can assess for any interval change. If you think the situation is urgent, give comanaging physicians the courtesy of determining if they want to see the patient before their next available appointment. If you think the situation is emergent, consider sending the patient to the emergency department rather than making an outpatient referral. If you are not sure, make a call and ask the specialist’s opinion. If you do send the patient to the hospital, call ahead and make them aware that the patient is on their way, and alert them of the concerning symptoms or findings. Good communication develops strong relationships with other doctors in your community, which is helpful for both your patients and your practice. |
7. Use optical coherence tomography (OCT). Any amount of papilledema is a medical emergency. OCT testing and assessing for a spontaneous venous pulsation can help distinguish between mild papilledema and hypoplastic or anomalous discs or optic disc drusen. In papilledema, the swelling tends to begin inferiorly and superiorly. If an OCT shows retinal nerve fiber layer (RNFL) thickening only inferiorly, consider early papilledema; an OCT with only nasal RNFL thickening in the setting of a small disc is more suggestive of an anomalous disc, which should never show progressive thickening (Cases 3, 4 and 5). If any question exists that the presentation is an anomalous disc, repeat the OCT in a month to rule out interval progression. An accurate OCT is crucial for these patients, as a poor image with missing data can make the RNFL measurements falsely thin, masking early thickening in papilledema.
8. Ensure appropriate workup and treatment. When comanaging papilledema patients, make sure they have had a thorough workup to determine the etiology of the papilledema. This includes magnetic resonance imaging (MRI) of the brain with and without contrast and magnetic resonance venography (MRV) to rule out venous sinus thrombosis. After these tests, patients without contraindication should have a lumbar puncture to measure the opening pressure and analyze the cerebrospinal fluid contents. If ultimately diagnosed with idiopathic intracranial hypertension, patients need to be educated that it could still lead to severe vision loss and they must be watched carefully. If vision loss is occurring despite weight loss attempts and Diamox (acetazolamide, Duramed) use, the patient may need surgical consultation for possible optic nerve sheath fenestration, ventriculoperitoneal shunt placement or both.
 | |
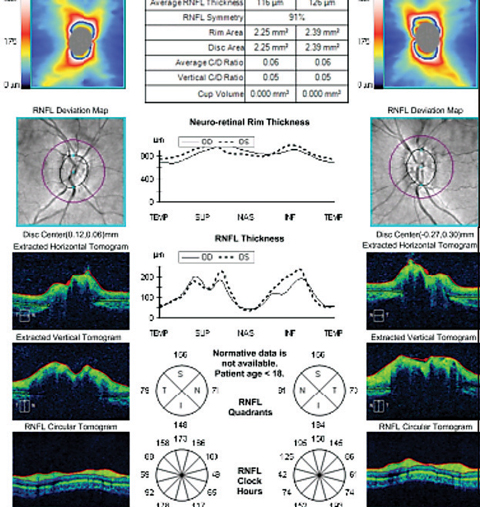 | Case 5. This five-year-old asymptomatic child has elevated optic discs. Although age-matched normals do not exist to help with OCT interpretation, clinicians can still appreciate that the average RNFL thickness, as well as the inferior and superior RNFL thicknesses, are greater than normal in this child. That, in combination with the lack of a spontaneous venous pulsation in either eye, is concerning for mild papilledema. Even without the presence of Paton’s lines or definite obscuration of the retinal vessels coursing over the optic disc margin, there is still concern for mild papilledema. Immediate neuroimaging revealed a malignant brain tumor. |
9. Perform cover testing in all gazes. Always accurately characterize patients’ symptoms of blur and diplopia, as patients often confuse these two symptoms. Ask enough questions to ascertain if the patient is experiencing true diplopia. If the diplopia resolves by covering either eye, it is true binocular diplopia, which is more concerning. Perform cover testing not just in primary gaze but in all positions of gaze, to determine if the results are comitant. All too often, clinicians only do cover testing in primary gaze, even though it is essential to assess cover testing in multiple positions of gaze to determine the etiology of the ocular misalignment. Clinicians must be familiar with the patterns of CN III, IV and VI palsies to be able to identify them on the cover testing results.
Other concerning manifestations of diplopia exist, however, and ODs should remember more obscure causes such as a skew deviation, which could also warrant urgent or emergent evaluation.
10. Test for torsion. As a general rule, a skew deviation or other brainstem motility finding is concerning for multiple sclerosis or other demyelinating process in a patient under age 50 and is suggestive of stroke in a patient over age 50. Skew deviation is often overlooked as a potential cause of diplopia and other non-specific complaints of visual disturbance. It is a vertical misalignment of the eyes and should be considered a differential diagnosis in any complaint of vertical diplopia or measurement of vertical ocular misalignment. One of the best ways to assess for an acute skew deviation is to look for the presence of torsion. Although not always the case, we typically expect to find incyclotorsion of the higher eye and excyclotorsion of the lower eye. This contrasts with a CN IV palsy, in which we would see a small amount of excyclotorsion of the higher eye.
When a patient complains of vertical diplopia or they have vertical ocular misalignment, clinicians should consider performing the Park’s three-step test and torsion testing. Although most tend to think of non-comitant deviations as more concerning, that’s not always true.
Skew deviations can have a vertical misalignment that is fairly comitant, and the magnitude does not have to be large. It is common to see a skew deviation in combination with internuclear ophthalmoplegia or nystagmus, so look carefully for these in any patient with a vertical misalignment. Any new onset nystagmus needs further evaluation.
If you consider that every patient could have a neuro-ophthalmic disease process, you are less likely to overlook something serious. If you do not consider such a diagnosis, you will never make such a diagnosis. To keep neuro diagnoses on your list of differentials, make your history and exam more thorough. Look at all of the patient’s test results in combination to see if they point to a problem with either the afferent or the efferent visual system. If you find a problem, or if you cannot explain your patient’s symptoms, additional neuro-ophthalmic workup and referral is imperative.
Dr. Malloy is the director of the Neuro-ophthalmic Disease Service at Pennsylvania College of Optometry, Salus University.
1. Malloy KA. Neuro-ophthalmic disease basics: Focus on the afferent visual system evaluation. Rev Optom. 2008;145(6):67-82. |

