 History
History
A 36-year-old white male presented to the emergency department with a chief complaint of ocular itching and redness that had persisted for two days. He also experienced tearing, photophobia and burning in both eyes.
The patient denied experiencing any trauma, but did report having a “cold” that began three to four days before the presentation of ocular symptoms.
His ocular history was remarkable for an esotropia, which was surgically corrected. His systemic history was unremarkable. He denied using any medications and reported no known allergies.
Diagnostic Data
His best-corrected visual acuity was 20/30 O.U. at distance and near through -1.00D spectacles. Pupils were equally round and reactive, with no afferent pupillary defect. Extraocular muscle movements were full and unrestricted in both eyes. Confrontation fields were full in all positions of gaze.
Refraction uncovered a slight increase in myopia of -1.25D, which yielded little change in acuity.
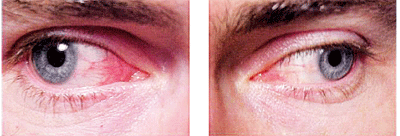
This 36-year-old patient presented
with a chief complaint of itching and redness in both eyes (O.D. left,
O.S. right). What is the proper diagnosis?
Slit lamp examination revealed mild, bilateral, external eyelid swelling; palpebral conjunctival papillae (grade 2+); moderate bulbar conjunctival injection; and punctate keratopathy. Both anterior chambers were deep and quiet.
His intraocular pressure measured 18mm Hg O.U. Dilated funduscopy of the posterior poles and peripheries was within normal limits in both eyes.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What’s the likely prognosis?
To find out, visit Review of Optometry Online, www.revoptom.com. Click on the on the cover icon, and then click “Diagnostic Quiz” under this month’s table of contents.
Thanks to Ha Pham Jibben, O.D., of Scottsdale, Ariz., for contributing this case.
Discussion
The diagnosis in this case is bilateral allergic conjunctivitis. We prescribed 1gtt Patanol (olopatadine 0.1%, Alcon) b.i.d. O.U. We also placed the patient on supportive therapy, which included Systane (Alcon) and cold compresses. We asked him to return for follow-up in two weeks.
At two-week follow-up, the patient reported good compliance and a marked reduction in symptoms. His visual acuity improved to 20/20 O.U. at distance and near. External examination of the adnexa revealed complete resolution of dermatologic edema. Slit lamp evaluation showed a 95% reduction in conjunctival and corneal irritation.
We asked the patient to titrate Patanol to q.d. and to use Systane b.i.d. and cold compress as needed for the remainder of the allergy season. We told him to return to the office immediately if he experienced new symptoms or lost vision.
The human allergic response yields various objective signs and physical symptoms. Ocular allergic conditions range from subtle—itchy, watery eyes with mild hyperemia—to extensive—inflammatory interactions between the ocular coats and adenexa. Patient symptoms often include itching, burning and tearing of the eyes, with a watery discharge. In most instances, the patient will report a history of allergies.1-4 The important observable clinical signs include tissue swelling (chemosis), red edematous eyelids, conjunctival papillae and a lack of palpable preauricular node.
The allergic response is classically considered an overreaction of the body’s immune system to immunogens or allergens.1-3 The response can be innate or acquired. The key component to the ocular allergic response is the mast cell. When mast cells interact with specific allergens, they degranulate and discharge mediators into the surrounding tissues.2 The primary chemical mediators include histamine, neutral proteases and arachadonic acid.2
There are many strata of ocular allergic reactions, so management is primarily aimed at reducing symptomatology. Perhaps the easiest and most effective treatment for allergic conjunctivitis is elimination or avoidance of the potentially offending allergen. Cold compresses, artificial tears and ointments can soothe and lubricate the ocular surface when applied on an as-needed basis.
Topical combination medications, such as Patanol and Pataday (olopatadine 0.2%, Alcon), Zaditor (ketotifen fumarate, Novartis), Alaway (ketotifen fumarate, Bausch & Lomb), Optivar (azelastine hydrochloride, MedPointe) and Elestat (epinastine, Allergan), combine the effects of mast cell stabilization with antihistaminic properties to arrest symptoms immediately and increase resistance to additional episodes. Pataday provides the advantage of being a true once-a-day preparation.
Topical non-steroidal anti-inflammatory drugs (NSAIDs), such as Acular (ketorolac tromethamine, Allergan) and Voltaren (diclofenac, Novartis), may also offer relief in moderate cases of ocular allergy. Topical steroidal preparations, such as Lotomax (lotoprednol etabonate, Bausch & Lomb), FML Forte (fluorometholone 0.25%, Allergan), Pred Forte (prednisolone acetate, Allergan), Flarex (fluorometholone acetate, Alcon) and Inflamase Forte (prednisolone sodium phosphate, CIBA Vision), are typically reserved for non-remitting presentations.1-4
Patients with a history of seasonal allergic conjunctivitis should be instructed to avoid those substances that precipitate symptoms, such as pet dander, dusty environments, and certain soaps or colognes.1-3 In severe cases, these patients may be treated four weeks in advance with loading doses of either topical mast-cell stabilizers or topical combination preparations to retard the degranulation process.4
Patients who are placed on supportive therapies should be followed as needed. Patients placed on topical NSAIDs should be followed every one to two weeks after the initiation of therapy. Patients placed on topical steroidal preparations should be seen one week after the start of therapy. Patients placed on topical steroids should be routinely monitored for changes in IOP for the duration of therapy.
1. Katelaris CH, Bielory L. Evidence-based study design in ocular allergy trials. Curr Opin Allergy Clin Immunol. 2008 Oct;8(5):484-8.
2. Bielory L, Friedlaender MH. Allergic conjunctivitis. Immunol Allergy Clin North Am. 2008 Feb;28(1):43-58, vi.
3. Abelson MB, Granet D. Ocular allergy in pediatric practice. Curr Allergy Asthma Rep. 2006 Jul;6(4):306-11.
4. Manzouri B, Flynn TH, Larkin F, et al. Pharmacotherapy of allergic eye disease. Expert Opin Pharmacother. 2006 Jun;7(9):1191-200.

