 A 52-year-old Hispanic female presented with poor vision in her right eye that had persisted for the past month. She reported no visual problems with her left eye. She exhibited no signs of pain or discomfort.
A 52-year-old Hispanic female presented with poor vision in her right eye that had persisted for the past month. She reported no visual problems with her left eye. She exhibited no signs of pain or discomfort.
Her systemic history was significant for HIV, which was diagnosed approximately seven months earlier. The patient reported taking multiple HIV medications, but did not know their names. She was unaware of her CD4 count or viral load. Additionally, the patient has type I herpes simplex virus (HSV), for which she takes acyclovir.
At her last eye examination two years ago, her best-corrected visual acuity measured 20/20 OU.
At this examination, her uncorrected visual acuity measured 4/200 OD and 20/20 OS. Confrontation fields showed generalized constriction 360° OD and full to careful finger counting OS. The pupils were equally round and reactive, with a strong afferent defect OD.
The anterior segment of the right eye was significant for fine keratic precipitates on the endothelium and trace to 1+ cells in the anterior chamber. The iris and lens were unremarkable. There were 2+ cells in the vitreous. The anterior segment of the left eye was completely unremarkable. Intraocular pressure measured 11mm Hg OU.
Dilated fundus examination of the right eye showed a hazy view of the retina (figure 1). We also obtained a spectral-domain optical coherence tomography (SD-OCT) scan of the patient’s right eye (figure 2).
The fundus examination of the left eye was completely normal.
Take the Retina Quiz
1. How do you account for the anterior segment changes OD?
a. Spillover.
b. Active anterior uveitis from an infectious process.
c. Active anterior uveitis from a noninfectious process.
d. Resolved anterior uveitis.
2. How would you classify the fundus changes seen in her right eye?
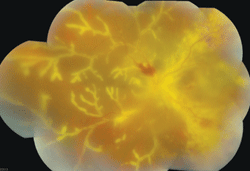
1. The posterior pole and peripheral montage of our patient’s right eye. Note the dramatic presentation throughout the retina.
a. Retinal vascular process.
b. Infectious process.
c. Infiltrative process.
d. Inflammatory process.
3. Which term commonly is used to describe the presentation observed in her right eye?
a. Periphlebitis.
b. Candle wax drippings.
c. Retinal vasculitis.
d. Frosted branch angiitis (FBA).
4. What is the correct diagnosis?
a. Cytomegalovirus (CMV) retinitis.
b. Acute retinal necrosis.
c. Toxoplasmosis.
d. Syphilis.
5. What is the most appropriate treatment?
a. Observation.
b. Referral to infectious disease specialist.
c. Antiviral therapy.
d. Antibiotic therapy.
For answers, see below.
Discussion
The dramatic changes seen in our patient’s right fundus represent FBA due to CMV retinitis. FBA was first reported in 1976 in a healthy, six-year-old Japanese boy who presented with panuveitis and severe retinal vasculitis. The florid, translucent perivascular exudate inspired the descriptive term “frosted branch angiitis.”1,2
More than 75% of FBA cases have been documented in Japan, with fewer than 20 confirmed diagnoses in the US.1,2 At one time, FBA was thought to predominantly affect fit, healthy individuals.1 Today, however, the condition is known to occur as a secondary outcome of severe infectious or inflammatory disease––CMV is one of the most common.1-3
In our patient, a fulminant retinal vasculitis and periphlebitis could be seen 360° throughout the fundus, which lent a frosted appearance to the perivascular exudate. Additionally, there was a full-thickness retinitis located adjacent to the optic nerve, which extended nasally along the superior and inferior arcades. This represents active CMV retinitis. Further, we detected generalized disc edema and retinal hemorrhages scattered throughout the fundus.
The right macula appeared thickened on clinical examination.
We confirmed this finding on SD-OCT at the location of the serous detachment. The CMV retinitis was responsible for the vitreous cells and the spillover into the anterior chamber, which gave us the somewhat hazy view into the retina.
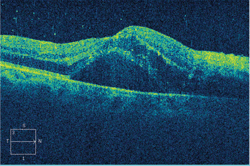
2. A SD-OCT scan through our patient’s right macula. What does this finding represent?
The pathogenesis of FBA is not completely understood, but likely depends on the underlying inflammatory disease. Some researchers have speculated that FBA is caused by a hypersensitivity to various infective agents.1,2
More specifically, this hypothesis suggests that the CMV elicits a periphlebitis via a type 3 hypersensitivity reaction to the pathogen’s particles.1 The reaction likely occurs within the retinal vascular endothelial cells, causing disruption of the microtubule support and endothelial function impairment.2
In the literature, most cases of FBA have presented bilaterally and were more common in females.1,2 Although our patient is female, the condition presented unilaterally. This is not much of a surprise, however, considering that the CMV was present only in that eye.
CMV retinitis is the most common ocular complication seen in patients who are diagnosed with HIV. The condition typically develops in patients whose CD4 counts are below 50, or even much lower. CMV was prevalent during the early years of the AIDS epidemic, developing in up to 40% of AIDS patients.3
Fortunately, since the advent of HAART (highly active antiretroviral therapy) more than a decade ago, researchers have documented a 55% to 95% decline in the incidence of CMV retinitis cases.3
CMV retinitis may be present anywhere in the retina. Posterior pole lesions exhibit a characteristic white, hemorrhagic appearance with retinal necrosis and edema, while the peripheral lesions are more indolent and nonhemorrhagic.
Our patient exhibited a combination of both presentations. With the use of several effective antiviral medications—including ganciclovir, foscarnet, valganciclovir and cidofovir—the treatment for CMV retinitis has become fairly standard.
Anti-CMV treatment should be individualized based on the presentation’s location and severity, as well as the patient’s current level of immune suppression, concomitant medication regimen and ability to comply with treatment. Therapy is induced at high doses for two to three weeks or until the retinitis stabilizes, followed by a maintenance dose.
Even though our patient did not know her CD4 count (or her viral load), we assumed that it was very low. We referred her for an immediate intravitreal injection of ganciclovir, and sent her to a local hospital to be admitted for further evaluation and treatment.
1. Walker S, Iguchi A, Jones NP. Frosted branch angiitis: a review. Eye (Lond). 2004 May;18(5):527-33.
2. Silva RA, Albini TA, Flynn HW. Retinal Physician. It still happens today: bilateral frosted branch angiitis in cytomegalovirus retinitis. Available at:
www.retinalphysician.com/articleviewer.aspx?articleID=104854. Accessed August 15, 2013.
3. Jabs DA, Van Natta ML, Kempen JH, et al. Characteristics of patients with cytomegalovirus retinitis in the era of highly active antiretroviral therapy. Am J Ophthalmol. 2002 Jan;133(1):48-61.
Answers
1. a
2. b
3. d
4. a
5. c

