 |
Eyelid lacerations may not be the most common walk-in appointment, but it when it is in your chair, it really doesn’t matter whether it is common or not. These wounds can be messy, and optometrists are tasked with evaluating, and sometimes treating, them.
A thorough understanding of the eyelid anatomy and lacrimal system is necessary when evaluating an eyelid laceration. You’ll need it to accurately assess whether an immediate referral to an oculoplastic lid surgeon is called for.
Anatomy
Beginning with the exterior upper eyelid, just under the epidermis lies the orbicularis muscle, which closes the eyelid. Below the orbicularis muscle is the orbital septum. This fibrous tissue is the anatomical division separating the preseptal and postseptal portions of the eye. Behind the orbital septum is orbital fat, the levator aponeurosis and Müller’s muscle.
Finally, you will see the palpebral conjunctiva lining the interior of the upper eyelid.
The lacrimal drainage apparatus is located in the medial canthus. Superior and inferior puncta on the lid margin drain through the canaliculus (approximately 8mm to 10mm) to the nasolacrimal sac. This sac lies in a fossa in the anterior portion of the medial orbital wall. The nasolacrimal sac drains via the nasolacrimal duct into the nasal cavity.
Triage Care
When a patient with a recent ocular trauma arrives, gather a thorough history to determine the origin of the trauma and whether the patient lost consciousness with the incident. Next, an examination of the eye and orbit will determine the severity and rule out other traumatic complications, such as an orbital fracture, foreign bodies, corneal lacerations or abrasions, hyphema, an open globe or trauma to the retina. When a penetrating foreign body, ruptured globe, severe blunt trauma or a loss of consciousness is suspected, a CT of the brain and orbits is warranted.
Once the trauma evaluation is complete and you determine that the patient has no other sight-threatening injuries, address the lid laceration itself. Eyelid lacerations are classified into two categories—complicated and simple.
When to Refer
Complicated lid lacerations should be referred to an oculoplastic surgeon for repair, along with any patients who may require sedation.
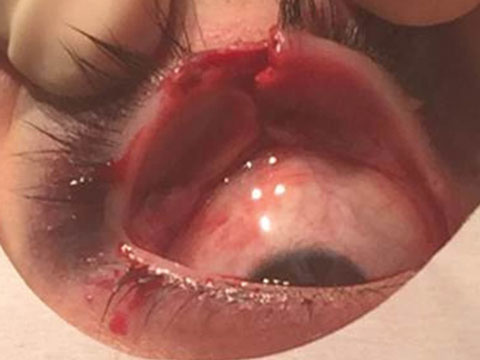 |
| This lid laceration was the result of a mishap during a basketball game. Photo: Alan G. Kabat, OD |
Full-thickness eyelid lacerations pass through the entire eyelid. If your patient has a full-thickness laceration, pay special attention to the underlying bulbar conjunctiva and be extra careful to rule out a penetrating ocular foreign body.
A laceration involving the eyelid margin requires a referral because of the complexity of the anatomy at the eyelid margin. These cases need to be referred out to decrease the chances of scarring or notching of the eyelid. If orbital fat is visible, the laceration has breached the orbital septum. This is an alarming finding because it indicates the postseptal orbital space is at risk for infection.
If your patient presents with a ptosis, it is possible the levator muscle could be damaged. This can lead to chronic ptosis or permanent levator damage. When eyelid lesions are medial, it is important to determine whether or not the lacrimal system is involved. Any involvement to the structures of the lacrimal system, such as the puncta, canaliculi, nasolacrimal sac and nasolacrimal duct, should be managed by an oculoplastic lid surgeon. Lacerations with poor alignment can lead to scarring, disfigurement of the eyelid and poor eyelid function, so these are best managed with a referral as well.
When to Treat
A simple lid laceration that is small, superficial and horizontal can be managed in-office. If the laceration is small, it may heal without anything more than a topical antibiotic ointment. Lacerations more than a quarter of the length of the eye can be treated with surgical or butterfly tape, or with a tissue adhesive.1 In some cases, sutures may be the best option. If you determine sutures are necessary, follow these steps:
Irrigate the wound. Use a sterile saline and check the eyelid laceration for any retained foreign body.
Prepare the wound. Apply betadine in a circular motion starting at the laceration edge and working away from the laceration. Ensure adequate hemostasis, if needed light pressure or possibly a cotton tip applicator soaked in phenylephrine can help to stop the bleeding.
Apply surgical tape. This can be applied perpendicular to the laceration. The surgical or butterfly tape should be placed on one side of the wound and gently pulled across the laceration so that the edges of the wound come as close together as possible without overlapping. Multiple butterfly strips may be necessary to bring the edges of the wound together the entire length of the laceration.
Tissue adhesive. A cyanoacrylate tissue adhesive can be a particularly effective way of closing a simple eyelid laceration. Bringing the edges of the laceration in apposition, without overlap, them apply the glue along the full length of the laceration and allow it to dry. Take special care not to get any of the adhesive in the eye.2
Prophylactic care. A tetanus booster is recommended at minimum every 10 years. Additionally, consider broad-spectrum antibiotics (cephalexin 250mg to 500mg PO QID) based on the likelihood of wound contamination. Follow-up evaluation can be scheduled in five to seven days to ensure appropriate healing and no complications.
The OD’s role is to assess the nature of the laceration to determine if the patient has a complicated laceration in need of a surgical consult or if it is a simple laceration to be managed in office. Applying basic first aid skills and infection prophylaxis will keep you a cut above the rest.
Drs. Krein and Krein are assistant professors at Northeastern State University in Oklahoma.
|
1. Handschel JG, Depprich RA, Dirksen D, et al. A prospective comparison of octl-2-cyanoacrylate and suture in standardized facial wounds. International Journal of Oral Maxillofacial Surgery. 2006;35(4):318-23. 2. Bruns TB, Worthington JM. Using Tissue Adhesive for Wound Repair: A Practical Guide to Dermabond. Am Fam Physician. 2000 Mar 1;61(5):1383-8. |

