 History
History
A 45-year-old black male presented with a chief complaint of sudden visual decrease OU, which began two days earlier. His systemic history was remarkable for hyperlipidemia, hypertension and a 15-year history of type 2 diabetes mellitus.
Current medications included insulin, lisinopril and atorvastatin. He reported no known allergies of any kind.
Diagnostic Data
His best-corrected visual acuity measured 20/100 OU, with no improvement upon pinhole testing. Extraocular muscle motilities were full and smooth, and his pupils exhibited no evidence of relative afferent defect.
Confrontational visual fields revealed intact peripheral vision OU. Ishihara color vision testing was unremarkable. Amsler grid testing revealed central metamorphosia OU. Slit lamp examination uncovered healthy anterior segment structures.
Intraocular pressure measured 21mm Hg OD and 20mm Hg OS. Additionally, his blood pressure was 192/94mm Hg.
Your Diagnosis
How would you approach this case? Does the patient require any additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Thanks to Jennifer Q. Duan, OD, of Manassas, Va., for contributing this case.
Discussion
The diagnosis in this case is bilateral, non-ischemic central retinal vein occlusion (CRVO). Vein occlusion is a common retinal vascular disease. The average age of onset ranges between 60 and 65 years.1 Patients typically present with acute, painless vision loss in the involved eye(s).2,3 During the acute stage, the most commonly recognized characteristics include extensive areas of diffused intraretinal hemorrhages in all four quadrants (extending from the posterior poles to the periphery), dilated and tortuous retinal veins, and retinal edema. Depending on the severity of ischemia, the affected eye also may exhibit cotton wool spots, disc edema and an afferent pupillary defect.2,3
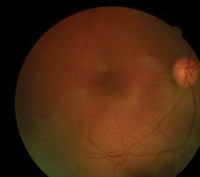
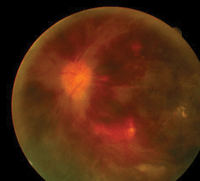
Fundus images (OD left, OD right) of our 45-year-old patient who complained of
sudden, bilateral vision loss two days earlier.
CRVO is strongly correlated with a host of systemic diseases and ocular conditions, including hypertension, diabetes mellitus, hyperlipidemia, atherosclerotic vascular disease, a history of tobacco use, increased body mass, abnormal rheological factors, elevated intraocular pressure and chronic open-angle glaucoma.4-7
It is fairly uncommon for CRVO to occur bilaterally or present in a relatively young individual. Therefore, in cases such as ours, a comprehensive work-up is recommended to determine the underlying cause. Also, be certain to screen for a hypercoagulable state, hyperviscosity syndrome, autoimmune disease and an inflammatory/infectious process.8,9
Initial testing includes fasting blood glucose, glycosylated hemoglobin, lipid panel, complete blood count, erythrocyte sedimentation rate, C-reactive protein, HIV status, platelet count, functional protein S and protein C assay, functional antithrombin III assay, antiphospholipid antibody titer, lupus anticoagulant, anticardiolipin antiobody titer, homocysteine level and activated protein C resistance.2,3,8,9
Central retinal vein occlusions may be classified as either ischemic or non-ischemic. Ischemic CRVOs are more visually devastating and often are associated with a poorer prognosis. Some clinical indicators include 20/400 visual acuity or worse, a positive relative afferent pupillary defect and more than 10DD of nonperfusion visible on fluorescein angiography.
Patients with non-ischemic CRVO should be evaluated every four weeks during the first six months after initial diagnosis to monitor for ischemic progression. The follow-up frequency may then be decreased to two to four times per year.10-12 Remember to evaluate the patient’s visual acuity and pupillary status, as well as monitor for neovascularization of the iris, angle, optic disc and retina, at follow-up.
Intravenous fluorescein angiography is required to confirm ischemic CRVO. Following diagnosis, retinal photocoagulation typically is indicated.2,3,6,10
We referred the patient for a retinology consult to rule out any additional testing or treatment modalities. The retinologist agreed with our diagnosis, testing strategy and follow-up plan. We scheduled the patient for re-evaluation in one month to rule out ischemic conversion as well as the development of retinal or anterior segment neovascularization.
Laboratory studies were ordered to quantify how effectively our patient’s current conditions were being managed, as well as to determine if he had any other underlying diseases. The studies were negative for new etiologies, indicating that––by exclusion––one of his current conditions (hyperlipidemia, hypertension or diabetes mellitus) was the culpable entity.
1. Garcia-Arumi J, Boixadera A, Martinez-Castillo V, et al. Radial optic neurotomy in central retinal vein occlusion: comparison of outcome in younger vs. older patients. Am J Ophthalmol. 2007 Jan;143(1):134-40.
2. Brown GC. Retinal Vascular Disease. In: Ho AC, Brown GC, McNamara JA, et al. Retina: Color Atlas and Synopsis of Clinical Ophthalmology. New York: McGraw-Hill; 2003:98-101.
3. Kaiser PK, Friedman NJ, Pineda R. Retina and Choroid. In: The Massachusetts Eye and Ear Infirmary Illustrated Manual of Ophthalmology. Philadelphia: Saunders; 2004:303-6.
4. Klein R, Moss SE, Meuer SM. The 15-year cumulative incidence of retinal vein occlusion: the Beaver Dam Eye Study. Arch Ophthalmol. 2008 Apr;126(4):513-8.
5. The Central Vein Occlusion Study Group. Baseline and early natural history report. Arch Ophthalmol. 1993 Aug;111(8):1087-95.
6. The Central Vein Occlusion Study Group. Natural history and clinical management of central retinal vein occlusion. Arch Ophthalmol. 1997 Apr;115(4):486-91.
7. The Eye Disease Case-Control Study Group. Risk factors for central retinal vein occlusion. Arch Ophthalmol. 1996 May;114(5):545-54.
8. Tomasini DN, Segu B. Systemic considerations in bilateral central retinal vein occlusion. Optometry. 2007 Aug;78(8):402-8.
9. Lahey JM, Tunc M, Kearney J, et al. Laboratory evaluation of hypercoagulable states in patients with central retinal vein occlusion who are less than 56 years of age. Ophthalmology. 2002 Jan;109(1):126-31.
10. Hayreh SS. Management of central retinal vein occlusion. Ophthalmologica. 2003 May-Jun;217(3):167-88.
11. Hayreh SS, Zimmerman MB, Podajsky PA. Incidence of various types of retinal vein occlusion and their recurrence and demographic characteristics. Am J Ophthalmol. 1994 Apr; 117(4):429-41.
12. Recchia FM, Carvalho-Recchia CA, Hassan TS. Clinical course of younger patients with central retinal vein occlusion. Arch Ophthalmol. 2004 Mar;122(3):317-21.

