 Corneal collagen crosslinking (CXL) uses riboflavin and ultraviolet light to strengthen the cornea in patients with keratoconus and post-LASIK ectasia by increasing the crosslinks within the collagen fibers. The procedure has not yet received FDA approval, but it has become a first-line treatment for keratoconus outside of the United States during the last five years. Regardless, there is widespread interest in CXL at this time, which will only increase once FDA approval is secured.
Corneal collagen crosslinking (CXL) uses riboflavin and ultraviolet light to strengthen the cornea in patients with keratoconus and post-LASIK ectasia by increasing the crosslinks within the collagen fibers. The procedure has not yet received FDA approval, but it has become a first-line treatment for keratoconus outside of the United States during the last five years. Regardless, there is widespread interest in CXL at this time, which will only increase once FDA approval is secured.
Here, we provide an overview of the corneal crosslinking procedure as well as discuss several important postoperative considerations. Also, we explore a case report that details the follow-up care of a keratoconus patient who underwent CXL.
Case Report
• History. A 34-year-old Indian female with a history of keratoconus presented for a follow-up examination and contact lens fitting after undergoing a CXL procedure. She reported decreased vision in her right eye that did not improve with either glasses or contact lenses. She reported poor comfort with small-diameter gas permeable contact lenses, even with 20/20 visual acuity O.U.
• Diagnostic data. Entering visual acuity with glasses was 20/40 O.D. and 20/30-2 O.S. Manifest refraction yielded 20/30 O.D. with -8.25 + 5.25 x 155 and 20/25 O.S. with -11.00 + 6.00 x 015. Pupils were normal, without evidence of afferent defect O.U. Slit lamp evaluation revealed 1+ meibomitis in each eye. The conjunctivae were normal in both eyes.
The corneas were clear in both eyes, without evidence of Vogt’s striae or a Fleischer ring. There was no corneal thinning in the right eye; however, we noted minimal thinning located inferiorly in the left eye. Central corneal thickness was 504µm O.D. and 501µm O.S.

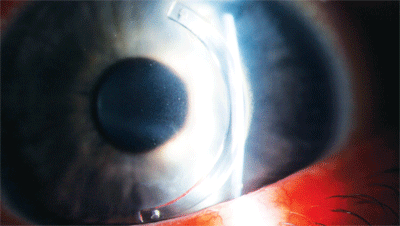
During a crosslinking procedure, this patient exhibited
riboflavin in the corneal stroma with an intact epithelium. Photo: Brian Boxer Wachler, M.D.
Intraocular pressure measured 16mm Hg and 17mm Hg by Tono-pen (Reichert) at 12:37 p.m. Dilated examination was within normal limits. Corneal topography demonstrated significant against-the-rule astigmatism in both eyes, with a steep simulated keratometry reading of 44.50D O.D. and 44.95D O.S. These K values were much more “normal” than the average K values for a patient with keratoconus.
• Discussion. After discussing contact lens options, the patient decided to proceed with a scleral lens fitting. We ordered a Jupiter design scleral lens (Essilor), with a 16.0mm lens for the right eye and 15.6mm lens for the left eye. Fortunately, the patient reported good vision (20/20+2 O.U.) and comfort with Jupiter scleral lenses.
Although CXL halts the progression of corneal ectasia, causes flattening of keratometry measurements and improves uncorrected and best-corrected vision, it does not altogether eliminate the need for glasses and contact lenses. Postoperative corneas are easier to fit with contact lenses due to a more regular (or less irregular) shape. Contact lenses designed for irregular corneas are still beneficial for patients with corneal ectasia after CXL. In this case, the patient was fit with a Jupiter scleral lens due to her history of poor comfort with small-diameter gas permeable contact lenses. The Jupiter scleral lens has been proven to provide acceptable visual acuity and comfort in patients with keratoconus.1
What is Corneal Crosslinking?
Investigations into the clinical utility of crosslinking in the corneal stroma as a conservative treatment for keratoconus began in the mid-1990s. Eberhard Spoerl, Ph.D., and Theo Seiler, M.D., Ph.D., showed that the cornea’s biomechanical behavior could be altered by irradiation using ultraviolet light with photosensitizers and by aldehyde reactions.2 Crosslinking is used frequently in the polymer industry to harden materials, as well as in bioengineering to stabilize tissue. Drs. Spoerl and Seiler treated porcine corneas with glutaraldehyde, Karnovsky’s solution (glutaraldehyde and paraformaldehyde) or riboflavin and UV-irradiation. Compared to untreated corneas, these procedures yielded increased corneal rigidity.
Corneal collagen crosslinking was first developed and introduced in 2003 by Gregor Wollensak, M.D., and colleagues.3 In patients with early keratoconus, CXL appeared to halt the progression of corneal ectasia.3 Dr. Wollensak showed that CXL flattens keratometry measurements and improves uncorrected and best-corrected visual acuity.3,4 Untreated eyes exhibited further steepening of keratometry readings and worsening of best-corrected visual acuity.5
The Procedure
The treatment procedure for CXL involves applying a topical anesthetic, then removing 7mm of the central corneal epithelium to allow a uniform diffusion of riboflavin into the stroma.6 Riboflavin is a water-soluble, non-toxic photosensitizer comprised of vitamin B2 that easily penetrates the corneal stroma in the absence of the corneal epithelium.
Next, the riboflavin 0.1% solution is applied prior to UVA irradiation to act as both a photosensitizer and a UV blocker.6 Homogenous UV irradiance of 3mW/cm2 and a wavelength of 370nm is used to irradiate the cornea for 30 minutes. An antibiotic ointment is applied postoperatively until the cornea has re-epithelialized.2
Keep in mind, however, that because 85% to 90% of UVA radiation is absorbed in the anterior 400μm of the cornea, CXL is not recommended for patients with corneas that are thinner than 400μm.6
Corneal crosslinking also can be performed without epithelial debridement (this procedure is often referred to as C3-R). One advantage to leaving the epithelium intact is that both the procedure and postoperative healing period are more comfortable for the patient.7 Additionally, patients who undergo C3-R may experience a shorter healing time as well as a lower risk for infection than patients who elect for CXL. However, C3-R may increase overall procedure time, because it could take longer for the riboflavin to penetrate into the corneal stroma.7,8
Nevertheless, epithelial debridement may be required to achieve stromal saturation of riboflavin during the procedure.2 Different techniques currently are being explored to make the epithelium more permeable. These can range from light surface scratching to chemically treating the epithelium with topical anesthetics or preservatives to facilitate better riboflavin penetration.
Postoperative Considerations
Following the procedure, healing generally is unremarkable, with the exception of slight transient stromal edema until corneal re-epithelization.2 In their clinical research, Drs. Spoerl and Seiler documented no corneal scarring, persistent corneal epithelial defects or changes in endothelial cell density.2 Corneal and lens transparency was not altered, nor was there evidence of cataract formation.2 Further, they observed no retinal damage.2 And, CXL did not alter patients’ ability to wear contact lenses postoperatively.
Still, you should look for several clinical findings when comanaging CXL patients:
This patient, who underwent a combination CXL/Intacs procedure, shows signs of epithelial erosion over the Intac. Photo: Mindy Toabe, O.D.
• Stromal haze. One report indicated that several patients experienced steroid-resistant stromal haze within two to three months after CXL treatment.8 Fortunately, none of the affected patients reported an associated loss in visual acuity.
Another study showed that 14 of 163 eyes developed significant stromal haze after C3-R.9 This haze, however, impaired uncorrected visual acuity and best-corrected visual acuity. Such postoperative stromal haze may be associated with the depth of the crosslinking procedure and the amount of keratocyte loss.2,8 Patients with advanced keratoconus are at higher risk of haze development due to thinner corneas and steeper corneal curvatures.8
• Stromal demarcation. Another common finding after C3-R is a thin stromal demarcation line over the entire cornea located at a depth of approximately 300μm.10
The demarcation line usually is visible beginning two weeks after treatment and does not cause any changes in the corneal endothelium, the lens or intraocular pressure. The stromal demarcation line may be due to changes in the refractive index or reflection properties of treated vs. untreated corneal tissue.8 Additionally, sterile infiltrates and central stromal scars may be present in patients after CXL.10
After CXL, patients’ refractive error must still be addressed. Keep in mind that corneal curvature may change during the first six months following the procedure, and repeated refractions, corneal topographies and contact lens adjustments likely will be required.
Regardless, corneal crosslinking may be able to delay or prevent the need for corneal grafts in patients with keratoconus. It may also be able to create a cornea that is more receptive to contact lenses.
In the case highlighted above, CXL stabilized the patient’s cornea, enabling a successful contact lens fit with good vision and comfort.
Thanks to Melissa Barnett, O.D., of the UC Davis Medical Center in Sacramento, Calif. for contributing this article.
1. Schornack MM, Patel SV. Scleral lenses in the management of keratoconus. Eye Contact Lens. Jan 2010;36(1):39-44.
2. Spoerl E, Huhle M, Seiler T. Induction of cross-links in corneal tissue. Exp Eye Res. 1998 Jan;66(1):97-103.
3. Wollensak G, Spoerl E, Seiler T. Riboflavin/ultraviolet-A-induced collagen crosslinking for the treatment of keratoconus. Am J Ophthalmol. 2003 May;135(5):620-7.
4. Vinciguerra P, Albe E, Trazza S, et al. Intraoperative and postoperative effects of corneal collagen cross-linking on progressive keratoconus. Arch Ophthalmol. 2009 Oct;127(10):1258-65.
5. Wittig-Silva C, Whiting M, Lamoureux E, et al. A randomized controlled trial of corneal collagen cross-linking in progressive keratoconus: preliminary results. J Refract Surg. 2008 Sep;24(7):S720-5.
6. Spoerl E, Mrochen M, Sliney D, et al. Safety of UVA-riboflavin cross-linking of the cornea. Cornea. 2007 May;26(4):385-9.
7. Koller T, Mrochen M, Seiler T. Complications and failure rates after corneal crosslinking. J Cataract Refract Surg. 2009 Aug;35(8):1358-62.
8. Mazzotta C, Balestrazzi A, Baiocchi S, et al. Stromal haze after combined riboflavin-UVA corneal collagen cross-linking in keratoconus: in vivo confocal microscopic evaluation. Clin Experiment Ophthalmol. 2007 Aug;35(6):580-2.
9. Raiskup F, Hoyer A, Spoerl E. Permanent corneal haze after riboflavin-UVA-induced cross-linking in keratoconus. J Refract Surg. 2009 Sep;25(9):S824-8.
10. Koller T, Mrochen M, Seiler T. Complications and failure rates after corneal crosslinking. J Cataract Refract Surg. 2009 Aug;35(8):1358-62.

