 |
Q:
A patient presented for a cataract evaluation, but the most glaring finding was a large lesion on his nose. How do I approach this?
“A few questions come to mind when a patient has a lesion on their face,” says Blair Lonsberry, OD, professor of optometry at Pacific University College of Optometry. “When did it appear? Location? Is it pigmented? Has it changed recently? Ulceration? Race of the patient? Age of the patient?”
This patient’s race (Caucasian), age (over 60) and location (sun-exposed skin) would lead one to think of a basal cell carcinoma (BCC) or squamous cell carcinoma (SCC). The most frequent (over 75%) skin malignancy in humans is BCC, which arises from stem cells associated with hair follicles, and chronic sun exposure is the most important factor in their development.
“The average lifetime risk for Caucasian individuals to develop BCC is approximately 30%,” Dr. Lonsberry says. “The typical patient demographic is fair-skinned individuals, typically older (peak incidence is at 80 years old), and the lesions most commonly arise on the forehead, top of the ears, neck and shoulders (sun-exposed areas).”
Skin-deep Foes
BCC most commonly presents as a slow-growing, skin-colored nodule with a pearly, shiny appearance. “Blood vessels are typically noted ‘feeding’ or visible on the tumor surface, with larger tumors showing central ulceration,” Dr. Lonsberry notes. “The central ulceration happens as the tumor increases in size and the supportive feeder blood vessels supply the active growing tumor on the periphery. With no ‘normal’ blood vessels feeding the central portion of the tumor, it begins to ulcerate.”
 |
|
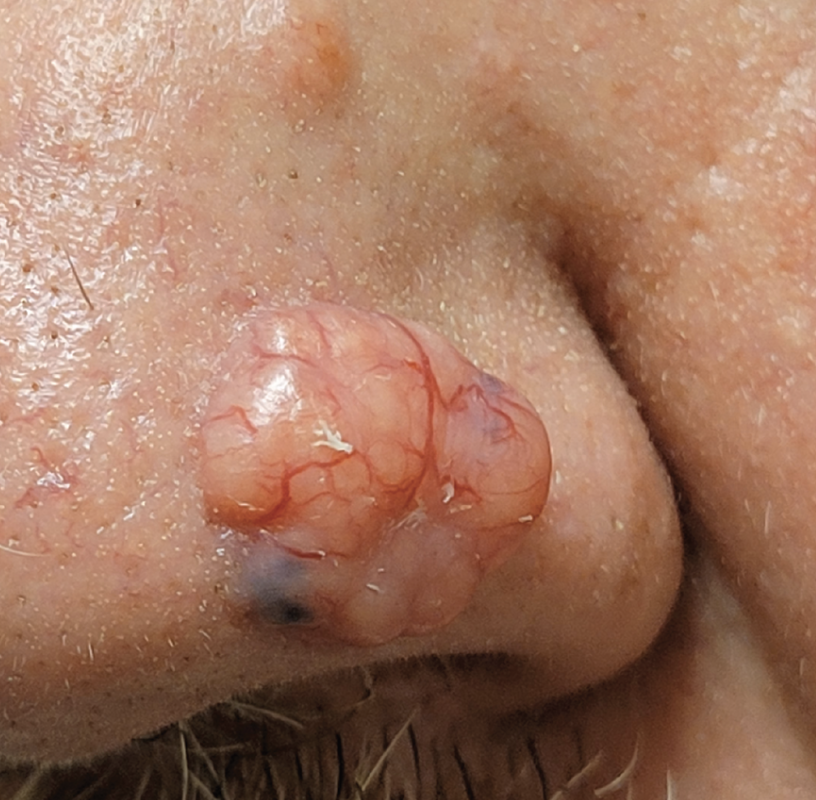
Fig. 1. SCC discovered during routine exam. Click image to enlarge. |
The classic BCC presentation is a tumor with “pearly borders with ulceration in the middle.” Metastasis is rare (<1% of cases), but it can progress to large, locally advanced and often deeply infiltrating tumors if not detected early, or if mismanaged or neglected.1,2 This lesion (Figure 1) doesn’t have the typical presentation but rather a thickened (hyperkeratotic), plaque-like appearance with telangiectatic vessels over the top.
Squamous cell carcinoma is the second-most common skin malignancy after BCC. “SCC most commonly appears after the age of 50 in areas of past sun exposure and typically occurs in light-skinned and light-eyed males who have a history of UV solar radiation exposure,” Dr. Lonsberry says. “It typically has a precursor lesion called actinic or solar keratosis, which then can exhibit tumor progression and has the potential to metastasize in the body.”
The most common areas for SCC are the face, nose, neck, bald scalp, extensor forearms, dorsal hands and shins. The typical presentation is a hyperkeratotic plaque with color varying from flesh-toned to erythematous with variable degrees of scale, crusting and ulceration. Another common finding is telangiectasias with or without active bleeding.3,4
Take a Sample
Conclusive diagnosis requires a biopsy with histopathology to determine the type of cells present as well as the staging and surgical borders. The most common surgical procedure for both BCC and SCC is Mohs micrographic surgery or resection with peripheral and deep exhaustive margin assessment. Mohs is recommended to achieve local control for high-risk and very-high-risk cutaneous squamous-cell carcinoma with very low rates of local recurrence.1,4
Our patient, who had never seen a dermatologist, was encouraged to see one immediately—and we booked it for him. Biopsy confirmed SCC. A Mohs procedure was scheduled. During the full-body exam, malignant melanoma was also found on his back, the detection of which could potentially save his life.
“Do not ignore non-ocular lesions on the face and other exposed skin,” Dr. Lonsberry advises. “We have the tools to look closely at skin abnormalities in the normal course of our eye exams.” Don’t leave appointments to chance, he advises. Make the appointments for them!
Dr. Ajamian is board certified by the American Board of Optometry and serves as Center Director of Omni Eye Services of Atlanta. He is vice president of the Georgia State Board of Optometry and general CE chairman of SECO International. He has no financial interests to disclose.
1. Fagan J, Brooks J, Ramsey ML. Basal cell cancer. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. www.ncbi.nlm.nih.gov/books/NBK470301/. Updated April 14, 2023. Accessed September 22, 2023. 2. Peris K, Fargnoli MC, Kaufmann R, et al. European consensus-based interdisciplinary guideline for diagnosis and treatment of basal cell carcinoma—update 2023. Eur J Cancer. 2023;192:113254. 3. Howell JY, Ramsey ML. Squamous cell skin cancer. [In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. www.ncbi.nlm.nih.gov/books/NBK441939/. Updated July 31, 2023. Accessed September 22, 2023. 4. Wysong A. Squamous-cell carcinoma of the skin. N Engl J Med. 2023;388(24):2262-73. |

