 |
In the midst of allergy season, optometrists can expect to see a rise in allergic conjunctivitis (AC). Approximately 20% to 40% of individuals, primarily young adults with a robust immune system, living in developed countries suffer from ocular allergies, with the incidence rising due to genetics, air pollution and pets.1-3 This commonly encountered condition requires understanding of the underlying pathological mechanisms, which trigger often debilitating symptoms.
Classification
AC has two main subtypes: seasonal allergic conjunctivitis (SAC) and perennial allergic conjunctivitis (PAC), with SAC constituting about 90% of cases.3 SAC typically lasts less than four weeks and occurs in response to seasonal allergens such as a genetically susceptible patient’s exposure to pollen.2,4 In contrast, PAC is more chronic, lasting greater than four weeks, and occurs in response to indoor allergens such as pet dander or dust mites that are present year round.2
Immune Mechanisms
Regardless of the classification, both subtypes are considered Type I immunoglobulin (Ig) E mediated, or immediate, hypersensitivity reactions.2,4,5 The process begins when a genetically predisposed individual is first exposed to a specific allergen, a process called sensitization. Neutrophils, macrophages and dendritic cells involved with the innate immune system interact with T-lymphocyte cells, producing cytokines that regulate both IgE and eosinophil proliferation. Activated T-cells interact with B-cells that have also encountered the allergen, producing antigen-specific IgE and the allergic and inflammatory response upon re-exposure.4,5
On second exposure to the allergen, these antigen-specific IgE receptors, present on mast cells on the surface of the conjunctiva, cause degranulation and release inflammatory mediators, primarily histamine.4,6,7 This leads to the signs and symptoms common for AC patients.
A patient’s susceptibility to certain allergens is complex and largely genetically determined. For example, an individual with no family history of allergy has roughly a 10% chance of developing an allergy, whereas 60% to 80% of children with both parents affected develop allergies.
In addition to genetics, a strong correlation exists between exposure in early in life, such as during prenatal development or infancy, and the development of allergic disease later in life. The first 12 to 18 months of life is a critical period for immune development, and exposure to a specific allergen may lead to the formation of memory T-cell responses that present later in life.8
The “hygiene hypothesis”—proposed to explain the increasing rise of atopic and allergic disease—suggests early exposure to infectious agents actually offered protection towards many immune-related disorders. With the decreasing incidence of infectious diseases in developed countries, an incidental rise in immune-mediated diseases has occurred. This is likely because the immune system has fewer potential targets to attack as part of its defense mechanisms, and so it looks for other environmental targets such as pollen or pet dander.9
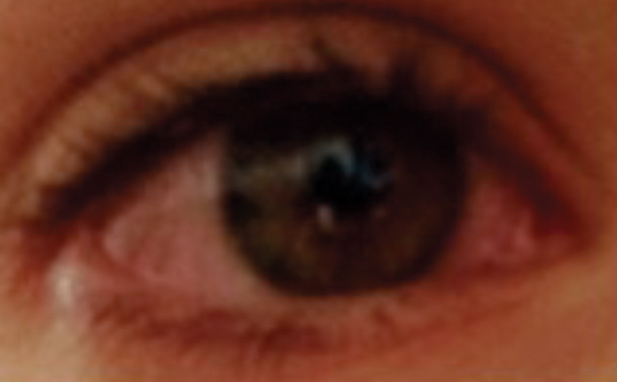 |
| Diffuse hyperemia/inflammation in a patient with allergic conjunctivitis. Photo: Alexandra Oszustowicz, OD |
Signs and Symptoms
The hallmark presentation of a patient with AC is bilateral pruritus. Additional signs include conjunctival hyperemia, tearing, eyelid edema and infraorbital edema or darkening, termed an “allergic shiner.”4 These manifestations arise from the activation of the histamine (H) receptors on the conjunctiva released by mast cells. H1 and H2 are the two main receptors in that area. H1 activation is responsible for itching, while H2 results in vasodilation leading to hyperemia, eyelid edema and chemosis. Recent evidence suggests that H4 receptors may also play a role in the signs and symptoms involved in ocular allergies, though information is limited.7
Table 1. Hypersensitivity Reactions and Ocular Presentations | |
| Type of Hypersensitivity | Examples of Ocular Diseases |
| IgE mediated | Allergic conjunctivitis |
| Cytotoxic IgG mediated | Myasthenia gravis, ocular cicatricial pemphigoid |
| Immune complex mediated | Steven Johnson’s syndrome, uveitis from systemic inflammatory conditions |
| Cell mediated | Contact dermatitis, herpetic keratitis, phlyctenulosis, corneal transplant rejection |
Additional Associations
Because allergic conjunctivitis is a manifestation of systemic allergies, 70% to 95% of patients with allergic conjunctivitis also present with rhinitis resulting from the same allergen.1,6 As such, patients treated with either oral or intranasal anti-allergy medications will find that their ocular symptoms also subside. This relationship is best described with the nasal ocular reflex theory, which suggests that the nasolacrimal duct acts as a physical connection from the nasal cavity to the ocular cavity, and that histamine release from mast cells in the nasal mucosa can initiate both the rhinitis and conjunctivitis.6
ODs will no doubt run into patients with ocular manifestations of systemic allergies, especially during this time of the year. Understanding the immunologic changes at play will allow the clinician to choose the right treatment options to target the various cells and receptors.
While this may seem like a rather benign condition, the symptoms are often debilitating for patients. It is also implicated in the possible pathogenesis of corneal ectasia, as excessive eye rubbing may alter corneal collagen, further highlighting the importance of this condition.10
1. Williams DC, Edney G, Maiden B, Smith PK. Recognition of allergic rhinitis in patients with allergic conjunctivitis. World Allergy Organization Journal. 2013;6(4):1-3. |

