 Q: I see many young and middle-age patients in my office with normal pressures but large physiologic cups. I’m afraid I might miss something if I don't send them out. How do you handle this?
Q: I see many young and middle-age patients in my office with normal pressures but large physiologic cups. I’m afraid I might miss something if I don't send them out. How do you handle this?
A: “Normal-tension glaucoma in young patients (under 50 years) is relatively uncommon, unless other factors—like low blood pressure or migraines—are present,” says Michael Chaglasian, OD, associate professor at Illinois College of Optometry and chief of staff of the Illinois Eye Institute, in Chicago. “Normal-tension glaucoma is even more uncommon for people in their 20s or 30s, which suggests that your patient probably has physiological cupping.”
So, you don’t need to send out all such patients. But, to avoid missing any problems in them, Dr. Chaglasian suggests these steps:
• Measure the optic disc size. This can easily be done at the slit lamp with dilated view, he says. Use a vertical and horizontal beam of light to begin and end at the outer disc margins. Take the millimeter reading (located on most slit lamps) and multiply by 1.3 when using a 90D lens (with a 78D lens, take the reading as is).
“Large discs have a large physiologic cup,” so a large disc with a large cup is not universally a strong risk factor for glaucoma, Dr. Chaglasian says. For whites, disc size of 1.8mm2 is average, while greater than 2.2mm2 is large. Hispanics and blacks have a larger average disc size of about 2.2mm2.
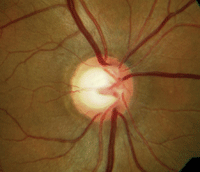
A 45-year-old patient with large physiological cupping, IOP of 21mm Hg—and normal visual fields.
• Look for symmetry. Strong symmetry of cupping and disc size suggests normal physiology, while asymmetry suggests glaucoma.
• Look carefully for focal notching. “Focal notching at the neuroretinal rim is a strong indicator of true glaucomatous damage,” Dr. Chaglasian says. While thinning of the rim tissue all around the cup may indicate glaucoma in some patients, it is more often physiological. Presentations of a disc hemorrhage or peripapillary atrophy do suggest glaucoma damage and require further investigation.
• Obtain a visual field. “Use a thresholding strategy for optimal sensitivity,” he says. “You don’t need blue-yellow technology.”
• Consider OCT imaging. “While OCT evaluation of the retinal nerve fiber layer and optic disc is excellent for many of these patients, it is not absolutely required,” Dr. Chaglasian says. If the disc is highly suspicious, then OCT, if available, can help identify retinal nerve fiber layer loss that is associated with early glaucoma.
“If all of your findings—IOP, optic nerve head, visual field—are normal and there are no other significant risk factors (such as family history, pachymetry of 500μm or less, etc.), then it is appropriate to follow the patient about once per year. These are cases that you don’t need to refer out,” he says.
• Take photos. “Baseline disc photographs may be the best test/procedure to get on these patients,” Dr. Chaglasian says. “Ten years from now, OCT instruments will be vastly different, but you’ll still have a digital photograph to refer to. It can be a lifesaver.”
• Consider something other than glaucoma. Patients who are under 50, have a repeatable visual field defect, have associated headaches or any other neurologic abnormalities, will most likely require further evaluation with neuro-imaging.
Q: If I do send them to a glaucoma specialist, when should I expect to see them back?
A: “If everything is normal, these patients should be returned immediately, or whenever they’re due for another visit,” he says. “Glaucoma specialists should not want nor do they need these patients in their practices.” However, if the specialist identifies disease or strong risk factors for glaucoma, the patient will likely require a few extra visits for further testing for the next two to four months.

