 |
History
A 57-year-old Caucasian male reported to the office emergently following blunt trauma to his left eye caused by a falling 2x4. He was clearly in distress, suffering from pain, photophobia, lacrimation, hemolacria (bloody tears) and blurry vision. He had no previous ocular history and his systemic history was remarkable for hypertension, for which he was properly controlled with lisinopril. He denied allergies of any kind.
Diagnostic Data
His best-corrected entering visual acuities were 20/20 OD and 20/100 OS at distance and near with no improvement upon pinhole. His external examination is demonstrated in the gross photograph. His pupils were normal with no evidence of afferent pupil defect. The biomicroscopic examination of the anterior segment is demonstrated in the magnified photograph. No other testing or manipulation was done.
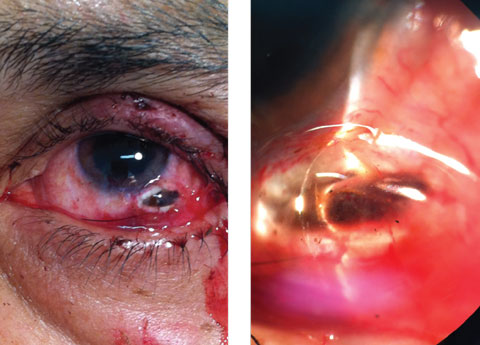 |
| This 57-year-old patient’s left eye shows the result of a blunt trauma. Can you diagnose him? Click image to enlarge. |
Diagnosis
There were no other additional studies necessary. The diagnosis in this issue is scleral laceration with ruptured globe. What is seen is a full-thickness penetrating scleral wound with incarcerated and evulsed vitreous and choroid. There is an accompanying grade I-microhyphema with cell and flare in the anterior chamber with scattered subconjunctival hemorrhage. The immediate first aide for these injuries is to cover the eye with a firm Fox eye shield. The eye should not be manipulated or pressured so as not to extrude any additional contents. The patient must be instructed not to rub it or pressure the surrounding adnexa. The patient must be transported to the nearest ocular trauma surgeon for repair.Trauma is one of the leading causes of monocular blindness worldwide.1-3 Men outnumber women is these catastrophic events significantly across the spectrum of age and geography. Initial visual acuity following the injury, wound length (greater than 5mm), retinal detachment and vitreous hemorrhage are all predictors of final visual outcome.2,3 Work-related injuries have a higher incidence of accompanying intraocular foreign debris.3 The trauma also induces premature cataractogenesis.3 Zone 3 injuries, presenting visual acuity of no light perception, afferent pupil defect and early signs of endophthalmitis were found to be significant predictors for requiring eventual enucleation.3
The Ocular Trauma Classification Group classifies wound locations into zones:
- Zone 1 injury involves the cornea and limbus
- Zone 2 injury involves the region 5mm or less posterior to the limbus
- Zone 3 injury involves the region exceeding 5mm posterior to the limbus.3,4
The system also classified open-globe and closed-globe injuries according to type of injury, mechanism of injury; grade of injury, by visual acuity in the injured eye at initial examination and the presence or absence of a relative afferent pupillary defect in the injured eye. The system was designed to be used by ophthalmic and nonophthalmic examiners who come into contact with ocular injuries.4
Penetrating injuries require the surgeon to complete wound exploration to remove all foreign matter and to determine the extent of the injury.6 Eyes with vitreous hemorrhage and retinal detachment will require three-port pars plan vitrectomy with retinal reattachment procedures and tamponade.6 Eyes with luxated lenses will require lensectomy with assessment for intraocular lens implantation. The Eye Injury Vitrectomy Study published seven risk factors that accurately predicted outcomes: globe rupture, zone 3, scleral wound greater than or equal to 10mm in length, ciliary body damage, severe intraocular hemorrhage, closed funnel retinal detachment or retinal prolapse and choroidal damage.6
In addition to the risks associated with the severity of the injury, ocular infection (post traumatic endophthalmitis) poses a separate but significant obstacle to recovery of structure and function.7 In one study, 571 eyes (571 patients) out of a total of 4795 eyes (4693 patients) developed endophthalmitis, with a rate of incidence measured at 11.91%.7 The study group determined that primary repair of the lesion within 24 hours of the event, intraocular tissue prolapse and the finding of self-sealing wounds demonstrated protective effects against the development of endophthalmitis.7 Gender, age, lens breach and posterior zone of wounds were not significant determinants.7 The study concluded that at discharge the proportion of eyes requiring enucleation/evisceration was higher in eyes with endophthalmitis than without endophthalmitis.7
Observation of the ruptured globe is the key to diagnosis. In cases that are unclear, exploratory surgical procedures are recommended as even multislice computed tomography misses identifying a significant number of ruptures.8,9
When a simple rupture is detected and repaired, operated eyes will typically be discharged with injected intravitreal antibiotic therapy and anti-inflammatory therapy with topical antibiotic, topical steroidal and topical cycloplegic treatment maintained as healing progresses.10,11 Cases involving choroidal rupture will require monitoring for the formation of choroidal neovascularization or cystic macular edema and all traumatic cases should be monitored for the formation of late traumatic glaucoma precipitated by trebecular meshwork failure.11,13-16 Cases involving vitreous hemorrhage may require three-port pars plana vitrectomy with retinal detachment repair including laser retinopexy, scleral buckling and retinal tamponade.12
The relative risk of developing traumatic glaucoma is significantly higher in cases that present with hyphema, elevated baseline intraocular pressure (IOP), angle recession of more than 180 degrees and lens displacement.16 The appropriate follow up medications for vitreoretinal/wound repair simultaneously assist hyphema resolution.14 Intraocular pressure must be monitored and governed medically at first, surgically when progression continues.13-16 As follow up visits continue the goal is to rule out complications with mending as well as assess the signs for the introduction of infection. Vascular endothelial growth factor inhibitors (VEGFI) have been successfully administered in cases where edema threatens vision or CNV develops.1
| 1. Romaniuk VM. Ocular trauma and other catastrophes. Emerg Med Clin North Am. 2013;31(2):399-411. 2. Bunting H, Stephens D, Mireskandari K. Prediction of visual outcomes after open globe injury in children: a 17-year Canadian experience. J AAPOS. 2013;17(1):43-8. 3. Bauza AM, Emami P, Son JH, et al. Work-related open-globe injuries: demographics and clinical characteristics. Eur J Ophthalmol. 2013;23(2):242-8. 4. Pieramici DJ, Sternberg P Jr, Aaberg TM Sr, et al; The OcularTrauma Classification Group. A system for classifying mechanicalinjuries of the eye (globe). Am J Ophthalmol 1997;123(6):820-31. 5. Pieramici DJ, Au Eong KG, Sternberg P Jr, Marsh MJ.The prognostic significance of a system for classifying mechanical injuries of the eye (globe) in open-globe injuries.J Trauma. 2003;54(4):750-4. 6. Feng K, Hu YT, Ma Z. Prognostic indicators for no light perception after open-globe injury: eye injury vitrectomy study.Am J Ophthalmol. 2011 ;152(4):654-662. 7. Zhang Y, Zhang MN, Jiang CH, et al. Endophthalmitis following open globe injury. Br J Ophthalmol. 2010;94(1):111-4. 8. Hoffstetter P, Schreyer AG, Schreyer C, et al. Multidetector CT (MD-CT) in the diagnosis of uncertain open globe injuries. Rofo. 2010;182(2):151-4. 9. Arey ML, Mootha VV, Whittemore AR, et al. Computed tomography in the diagnosis of occult open-globe injuries.Ophthalmology. 2007;114(8):1448-52. 10. Assi A, Chacra CB, Cherfan G. Combined lensectomy, vitrectomy, and primary intraocular lens implantation in patients with traumatic eye injury. Int Ophthalmol. 2008;28(6):387-94. 11. Seal DV, Kirkness CM. Criteria for intravitreal antibiotics during surgical removal of intraocular foreign bodies. Eye (Lond). 1992;6 ( Pt 5):465-8. 12. De Benedetto U, Battaglia Parodi M, Knutsson KAIntravitreal bevacizumab for extrafoveal choroidal neovascularization after ocular trauma.J Ocul Pharmacol Ther. 2012;28(5):550-2. 13. Bai HQ, Yao L, Wang DB, Jin R, Wang YX. Causes and treatments of traumatic secondary glaucoma. Eur J Ophthalmol. 2009;19(2):201-6. 14. Gharaibeh A, Savage HI, Scherer RW, et al. Medical interventions for traumatic hyphema.Cochrane Database Syst Rev. 201119;(1):CD005431. 15. Schlote T, Rohrbach M. Traumatic glaucoma--a survey. Klin Monbl Augenheilkd. 2005;222(10):772-82. 16. Sihota R, Kumar S, Gupta V, et al. Early predictors of traumatic glaucoma after closed globe injury: trabecular pigmentation, widened angle recess, and higher baseline intraocular pressure. Arch Ophthalmol. 2008;126(7):921-6. |

