 History
History
A 76-year-old white female presented for an urgent visit with a chief complaint of bilateral foreign body sensation and irritation (OS > OD) that had persisted for two weeks. In the past, we saw the patient for complaints of seasonal ocular allergy and mild dry eye.
Additional ocular history included bilateral cataract extraction and blepharoplasty three years earlier. She denied any exposure to foreign bodies or harmful substances. Current ocular medications included Pataday (olopatadine hydrochloride 0.2%, Alcon) and artificial tears, as needed.
She had no contributory systemic history and reported no allergies to medications.
Diagnostic Data
Her best-corrected visual acuity measured 20/20 OU. External examination was normal, with no evidence of afferent pupillary defect. Refraction uncovered mild hyperopia with negligible changes to her habitual spectacle prescription. Biomicroscopy revealed normal lids and lashes OU.
Corneal findings included minimal inferior punctate staining OU and an irregular tear film. The bulbar conjunctiva was white and quiet OU. The anterior chambers were unremarkable.
Her IOP measured 16mm Hg OU. An undilated, 90D fundoscopic examination showed quiet grounds and normal posterior poles OU.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What’s the likely prognosis?
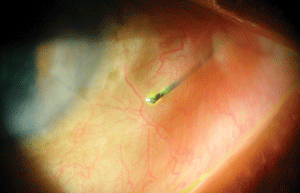
We uncovered the presence of a foreign object in our patient’s left eye. How did it get there?

Discussion
Upon lid eversion, we documented grade 1 palpebral conjunctival papillae O.U. Additionally, we performed sodium fluorescein staining and corneal lavage.
The diagnosis in this case is an exposed and embedded suture from a previous cataract procedure O.S.
With the patient’s upper lid everted, we used a jeweler’s forceps to determine if the suture was attached firmly to the tissue located within the lid.1
When no tissue adhesion was detected, we extracted the partial suture. Due to the adjacent inflammatory response from the exposed suture material, we prescribed a topical steroidal-antibiotic combination agent q.i.d. for one week.1,2
One week later, the patient returned for a progress evaluation and an intraocular pressure measurement (to monitor the steroidal medication’s impact). Fortunately, the patient experienced no complications following suture extraction.
Thanks to Marc D. Myers, OD, of Coatesville, Pa. for contributing this case.
1. Usgaocar RP. Lessening the pain of suture removal. Plastic Reconstr Surg. 1998 Jul; 102(1):268.
2. Abenavoli FM. Painless stitch removal. Plastic Reconstr Surg. 2001 Sept;108(4):1084-5.

