Q: A 16-year-old white female was referred for a corneal evaluation due to extensive corneal neovascularization in the inferior portion of the epithelium O.U. What is the differential diagnosis in a case such as this, and how would you treat the patient?

A: The patient initially presented to her optometrist complaining of blurred vision in her left eye with no history of ocular inflammation. She had a history of recurrent styes, but her ocular and systemic histories were otherwise unremarkable. She reported no allergies and took no medications. Her last visit was three years earlier.
She was referred to Heartland Eye Consultants in Omaha, Neb., where Robert J. Vandervort, O.D., consulted on the case. External examination was normal, and her face was totally clear of any visible acne or telangiectasia. Visual acuity with her current prescription was 20/20 O.D. and 20/40 O.S. Acuity in the left eye improved to 20/25 with pinhole. There was no hyperemia in either eye, but she had extensive neovascularization in the inferior corneas of both eyes (O.S. worse than O.D.), which caused the reduced VA in the left eye. Mild corneal thinning and scarring was noted at the leading edge of neovascularization.
Examination of the lids and lashes indicated mild meibomian gland dysfunction (MGD). The patient was fair skinned, and her complexion was relatively clear.
Possible diagnoses include:
- Atopic keratoconjunctivitis (AKC).
- Chronic hypersensitivity keratitis secondary to MGD.
- Atypical pediatric rosacea.
- Interstitial keratitis associated with syphilis.
“Due to the bilateral nature, lack of any significant history of symptomatic inflammation, and involvement in the inferior third to half of each cornea, we believe the condition to be most consistent with a variant of juvenile rosacea with associated MGD, or chronic hypersensitivity secondary to MGD without rosacea,” Dr. Vandervort says. “Interstitial keratitis in syphilis is usually unilateral and deeper in the stroma than the neovascularization in this patient. So, we consider that option very unlikely.”
The meibomian gland disease and neovascularization are the two main clues. Consider: In one study of rosacea patients, 95% of patients had meibomian gland disease or blepharitis, and 90% had keratitis, corneal scarring, or neovascularization.1
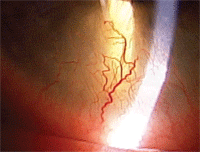
This patient had bilateral, symmetrical corneal neovascularization.
Early recognition and prompt aggressive treatment are necessary to avoid extensive scarring and corneal opacification.1 Rosacea is rare in children, and subtle changes can be overlooked.2,3 In one study of 20 patients with rosacea, ocular involvement preceded skin eruption in 11 patients (55%).3 Also three out of 20 patients (15%) had ocular involvement alone.3
“Due to the potential threat to vision, we obtained an additional opinion from a corneal specialist,” Dr. Vandervort says. “He agreed with our diagnosis but leans more toward hypersensitivity keratitis secondary to MGD.”
The patient was started on AzaSite (azithromycin 1%, Inspire) to treat the meibomian gland dysfunction. After consulting with the patient’s pediatrician, she was also prescribed doxycycline 50mg b.i.d. for two weeks then q.d. thereafter. Because there was no active inflammation and significant corneal thinning was present centrally in the left eye, she was not prescribed a steroid.
“Because her visual acuity is at risk, we’re going to follow her carefully for any further progression,” he says. “If progression does occur even with the aggressive topical and oral antibiotic therapy, then we’ll consider initiating a topical steroid.”
1. Donaldson KE, Karp CL, Dunbar MT. Evaluation and treatment of children with ocular rosacea. Cornea 2007 Jan;26(1):42-6.
2. Oltz M, Check J. Rosacea and its ocular manifestations. Optometry 2011 Feb;82(2):92-103.
3. Chamaillard M, Mortemousque B, Boralevi F, et al. Cutaneous and ocular signs of childhood rosacea. Arch Dermatol 2008 Feb;144(2):167-71.

