 |
Q:
A patient presents to me for the first time with a classic case of retinitis pigmentosa (RP). I know there is no treatment, but in what other ways can I help counsel this patient?
A:
RP is one of the most common inherited retinal diseases (IRD). “No treatment is currently available, so the key to patient care lies in management,” says Himakshi Bhatt, OD, an ocular disease resident at Omni Eye Services of Atlanta. “This is where genetic testing comes into play.”
Genetic information can provide insight to inheritance patterns, severity and ultimately disease prognosis. All this information together can help the doctor provide optimal patient care.
 |
|
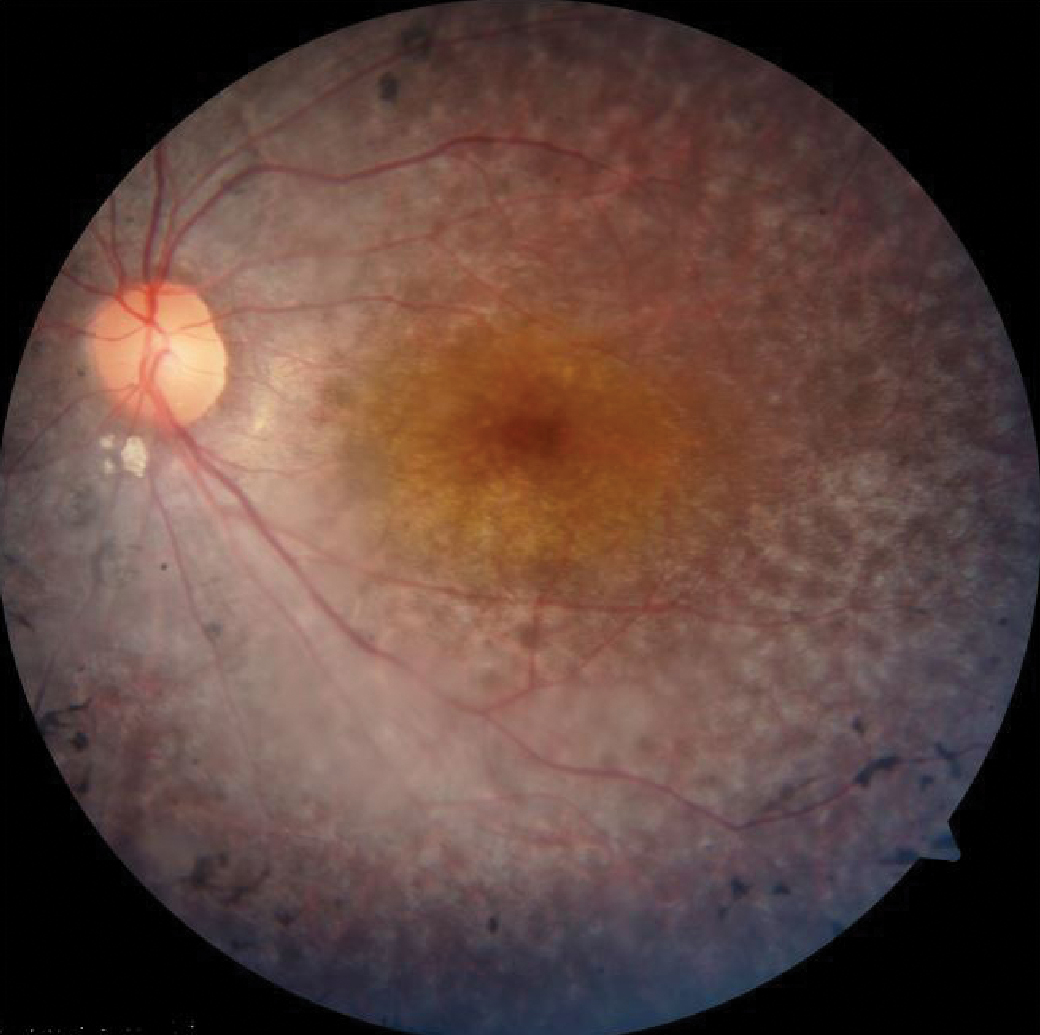
RP with arteriolar attenuation and bone spicules. Note the peripheral retinal loss with central island of sparing. Click image to enlarge. |
Inheritance Outcomes
RP is a group of inherited disorders that results in the degradation of the rod (and eventually cone) photoreceptors. The classic presentation includes the triad of bone spicules, arteriolar narrowing and waxy optic disc pallor.1 Additionally, posterior subcapsular cataracts, epiretinal membranes and cystoid macular edema can also be present in some cases.1 Common symptoms include nyctalopia, reduced visual acuity (VA), peripheral visual field loss and, in later stages, photopsia.
Over 50 genes are affected in the disease process, with the most common mutations affecting phototransduction in rods, the retinoid cycle and photoreceptor structure. Commonly affected genes include PRFP31 and RHO for autosomal-dominant inheritance, ABCA4 and USH2A for autosomal recessive inheritance and RPGR for X-linked inheritance.2
The severity and outcome of RP greatly depends on inheritance. Autosomal dominant accounts for about 15% of all RP and is the least severe in presentation. Onset is gradual; the average best-corrected VA is 20/30 for someone under 30 years old. Autosomal recessive RP, the most common variant, has a poorer visual prognosis. Patients usually experience severely diminished vision early in life. X-linked is the rarest form and the most severe. Usually only males are affected, and VA is typically worse than 20/200.
Plan and Manage
Though it may seem daunting, genetic testing is readily available and accessible for patients with RP. For example, Invitae (through Spark Therapeutics) offers free genetic testing for IRDs (www.invitae.com/en/idyourird). Additional testing resources are available with the Foundation Fighting Blindness’s My Retina Tracker Program through Blueprint Genetics. Saliva, blood or buccal samples are taken in-office using a pre-ordered collection kit. The specimen is then shipped to a company-specific lab and results come back in a few weeks.
Once mutation and inheritance patterns are discerned, treatment and management of your patient can begin. The only known genetic treatment currently available for RP is for mutations in the RPE65 gene; all other types require mindful management.2
“Being diagnosed with an incurable disease is a harsh reality for many to cope with,” Dr. Bhatt says. “This information can empower the patient and allow them to come to terms with their diagnosis.”
Genetic testing is critical to family planning, especially disease severity and inheritance. Knowing the specific mutation can also be valuable when it comes to future treatment options.
“New clinical trials and experimental gene therapies are always on the horizon, and knowing a patient’s specific mutation can open the door to these opportunities,” Dr. Bhatt says.
Knowing how severe the final disease state will be or how quickly it will progress provides both the patient and doctor crucial information.“Patients have a way to take their disease in their own hands and no longer fear the unknown,” Dr. Bhatt notes. “Testing can also help the provider find the best resources and provide their patient better counsel.”
It is key to emphasize that the disease is not the patient’s fault and that, as a team, you and the patient will take on the challenge together.
Dr. Ajamian is the center director of Omni Eye Services of Atlanta. He currently serves as general chairman of the education committee for SECO International and is vice president of the Georgia State Board of Optometry. He has no financial interests to disclose.
1. O’Neal TB, Luther EE. Retinitis pigmentosa. StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2021. 2. Fahim AT, Daiger SP, Weleber RG. Nonsyndromic retinitis pigmentosa overview. GeneReviews. www.ncbi.nlm.nih.gov/books/nbk1417. January 19, 2017. Accessed March 29, 2022. |

