 A 64-year-old female was referred for consultation regarding the unusual vasculature on her left optic disc. The patient had both hypertension and type 2 diabetes, so the referring clinician was concerned that she may have neovascularization of the disc––although there were no other signs of retinopathy.
A 64-year-old female was referred for consultation regarding the unusual vasculature on her left optic disc. The patient had both hypertension and type 2 diabetes, so the referring clinician was concerned that she may have neovascularization of the disc––although there were no other signs of retinopathy.
In addition to hypertension and diabetes, her medical history was significant for hypercholesterolemia. She reported many years of good control with her medications.
Upon examination, the patient reported no complaints with her eyes or vision. Her visual acuity was 20/20 OU. Intraocular pressure measured 14mm Hg OD and 12mm Hg OS. She had significant cupping in each eye, but exhibited symmetrical, healthy rim tissue.
Of note were two areas of vascular abnormality on her left optic disc. Upon further evaluation, we determined that these anomalies were not areas of neovascularization, but rather collateral vessels.
This month, we review the pathophysiology of collateral vessels and discuss their significance.
 |
|
|
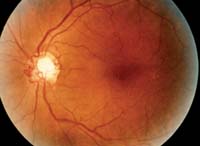
Collateral vessels of the inferior nasal and superior temporal disc.
|
Many years ago, we were taught that collateral vessels resulted from three causes: vascular occlusion, glaucoma and/or optic nerve sheath meningioma. We have seen these vessels in patients’ eyes over our respective careers too many times to count. These vessels have been referred to by many names, such as collateral vessels, anastomotic vessels, optic disc shunts, shunt vessels and, most commonly, optociliary shunt vessels. Unfortunately, “optociliary shunt vessels” is the most inappropriate name because they are neither optociliary nor shunts. Technically, a shunt is a direct communication between an artery and a vein, which is not what is happening in this instance.
So what are these vessels? Where do they come from, what causes them and what do we do about them?
Strong Ties to Vein Occlusion
Technically, collateral vessels are retinochoroidal. In the context of vaso-occlusive disease, these anastomotic vessels act to reroute blood from one obstructed vein to an unobstructed vein. The pressure differential between an obstructed vein and an unobstructed vein initiates a redirection of blood flow though pre-existing collateral channels, exploiting capillaries deep within the retina.1
In cases of branch retinal vein occlusion (BRVO), this process typically involves redirecting blood from the occluded retinal vein to an unoccluded retinal vein. This is often seen with connections between retinal veins, with the collateral vessels typically crossing the horizontal raphe.
However, in cases of central retinal vein occlusion (CRVO), the redirection usually is from an occluded central retinal vein to a choroidal vein. In these instances, the collateral vessel can be seen on the surface of the optic disc, but then seems to disappear as it connects to the choroidal circulation.2-4
The prognostic significance of collateral vessel development after venous occlusion is unknown. While neovascularization is an ocularly and visually damaging attempt to reperfuse an ischemic eye due to the lack of tight junctions and a predilection to leakage, collateral vessels typically do not leak. They are often considered a beneficial reparative process designed to bypass an occluded tributary.
One study group examined the genesis of these anastomotic vessels following CRVO and found a decreased incidence of anterior segment neovascularization in eyes that developed collateral vessels.5 Thus, they believed that collateral vascularization following CRVO was indeed protective against the development of neovascularization. However, other researchers contend that the development of collateral vascularization after CRVO results in a poor visual outcome.6
More recently, the SCORE study examined the prognostic significance of collateral vessel development in response to non-ischemic BRVO and CRVO in patients who were being treated with intravitreal steroid injections.4
In eyes with BRVO, the researchers found that the factors most associated with collateral vascularization were longer duration of macular edema, smaller area of retinal hemorrhage and younger age. By contrast, eyes with non-ischemic CRVO developing collateral circulation were associated with shorter duration of macular edema.
Overall, however, the feature most frequently associated with the development of collateral circulation in each type of occlusion was the overall area of capillary non-perfusion. Further, the SCORE researchers discovered that the different types of occlusions resulted in characteristic collateral development. In other words, eyes with CRVO tended to develop disc collaterals while eyes with BRVO developed collateral vascularization across the retina (although this pattern was not universal).4
 |
|
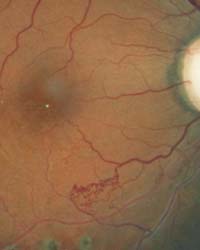
This patient's retina exhibits collateral vessels bypassing an occluded vessel.
|
A Potential Sign of Tumor
Collateral vessel development is also known to be caused by optic nerve sheath meningioma, as well as some other compressive optic neuropathies.7-9 Meningiomas are benign, neoplastic lesions arising from meningothelial cells of the dural meninges, including the optic nerve sheath. Optic nerve sheath meningiomas exhibit characteristic indolent growth over years, presenting with the classic triad of collateral vascularization of the optic disc, optic atrophy and progressive vision loss.
It is unlikely that optic nerve compression alone results in collateral vascularization; these eyes typically exhibit optic disc pallor and slow, progressive vision loss. In contrast, patients who develop collateral vessels from complete vascular occlusion usually have a history of abrupt vision loss.
What About Glaucoma?
In addition to vascular occlusion and optic nerve sheath meningioma, other identified causes of collateral vessel development include optic disc drusen, high myopia and diabetes, as well as congenital development.10-12 But, what about glaucoma? While collateral vessels have been reported to occur in glaucomatous eyes, it’s difficult to consider it a primary cause.
Glaucoma and retinal vascular occlusions are often comorbidities in patients, and asymptomatic retinal vein occlusions do occur. Asymptomatic mini-occlusions have been reported in glaucomatous eyes that did not exhibit the widespread retinal hemorrhaging typically associated with classic retinal vein occlusions.13,14 As such, we don’t consider glaucoma itself to be an etiology of collateral vessel development. So, when encountering these vessels in glaucomatous eyes, we often attribute their presence to a past vascular event rather than glaucoma.
When evaluating collateral vessels of the retina or disc, realize that they are neither optociliary nor shunts; they are most likely associated with vascular disease, not glaucoma; some other rare causes do exist; and that patients with disc pallor in association with disc collaterals likely harbor a compressive lesion. Otherwise––simply note their existence in the patient’s record, reassure the individual, and do nothing more.
1. Kohner EM, Dollery CT, Shakib M, et al. Experimental retinal branch vein occlusion. Am J Ophthalmol. 1970 May;69(5):778-825.
2. Takahashi K, Muraoka K, Kishi S, Shimizu K. Formation of retinochoroidal collaterals in central retinal vein occlusion. Am J Ophthalmol. 1998 Jul;126(1):91-9.
3. Schatz H, Green WR, Talamo JH, et al. Clinicopathologic correlation of retinal to choroidal venous collaterals of the optic nerve head. Ophthalmology. 1991 Aug;98(8):1287-93.
4. Weinberg DV, Wahle AE, Ip MS, et al. Score Study Report 12: Development of venous collaterals in the Score Study. Retina. 2013 Feb;33(2):287-95.
5. Fuller JJ, Mason JO 3rd, White MF Jr, et al. Retinochoroidal collateral veins protect against anterior segment neovascularization after central retinal vein occlusion. Arch Ophthalmol. 2003 Mar;121(3):332-6.
6. Cunningham MA, Edelman JL, Kaushal S. Intravitreal steroids for macular edema: the past, the present, and the future. Surv Ophthalmol. 2008 Mar-Apr;53(2):139-49.
7. Rebolleda G, Corcóstegui J, Arruabarrena C, et al. Optociliary shunt vessels in compressive optic neuropathy by the intracranial internal carotid artery. Eur J Ophthalmol. 2008 Mar-Apr;18(2):316-9.
8. Tsukahara S, Kobayashi S, Nakagawa F, Sugita K. Optociliary veins associated with meningioma of the optic nerve sheath. Ophthalmologica. 1980;181(3-4):188-94.
9. Zakka KA, Summerer RW, Yee RD, et al. Opticociliary veins in a primary optic nerve sheath meningioma. Am J Ophthalmol. 1979 Jan;87(1):91-5.
10. Masuyama Y, Kodama Y, Matsuura Y, et al. Clinical studies on the occurrence and the pathogenesis of optociliary veins. J Clin Neuroophthalmol. 1990 Mar;10(1):1-8.
11. Anderson SF, Townsend JC, Selvin GJ, Jew RL. Congenital optociliary shunt vessels. J Am Optom Assoc. 1991 Feb;62(2):109-15.
12. Lee JJ, Yap EY. Optociliary shunt vessels in diabetes mellitus. Singapore Med J. 2004 Apr;45(4):166-9.
13. Piltz-Seymour JR, Piccone MR, Pathay F, Brucker AJ. Venous collateral remodeling in a patient with posttraumatic glaucoma. Am J Ophthalmol. 1999 Jul;128(1):101-3.
14. Tuulonen A. Asymptomatic miniocclusions of the optic disc veins in glaucoma. Arch Ophthalmol. 1989 Oct;107(10):1475-80.

