 |
Q:
I’m worried about the risk of Acanthamoeba keratitis (AK) in my patients who wear contact lenses. Why are contact lens wearers at an increased risk? How significant is the reduction in safety and efficacy if they switch to daily disposable lenses?
Since Acanthamoeba is ubiquitous, i.e., present everywhere, and 50% to 100% of us have antibodies to this organism, why is Acanthamoeba keratitis not more common and why are contact lens wearers most at risk?1 “The rate of AK is 20 times more common in contact lens wear than the general population,” says Associate Professor Nicole Carnt, BOptom, PhD, of the School of Optometry and Vision Science, UNSW, Sydney in Australia.2 In reusable lens wear, refraining from water activities such as swimming and showering can reduce risk by over 50%.3
Acanthamoeba is everywhere but predominately lives in water and soil.4 It’s been found in the United Kingdom and Australia that roughly a third of domestic bathroom sinks harbor the organism.5,6 Acanthamoeba has even been isolated from a shower curtain.7 Dr. Carnt notes that studies indicate that the same genotype of Acanthamoeba in a patient’s home water can also be found in the eye, indicating a direct link between the two.6,8
Contact lenses act as a vector to transmit organisms to the eye. While 6% of contact lens cases harbor Acanthamoeba, there is not a direct correlation.9 However, daily disposables are four times less likely to cause AK than reusables, likely related to contamination of the lens case and the reusable lenses, according to Dr. Carnt.10 When compared with reusable lens bacterial keratitis, cases involving daily disposables display a smaller proportion of corneal isolates that are gram-negative (or environmental) and more gram-positive (endogenous) organisms, generally resulting in better outcomes.11
 |
|
A contact lens with Acanthamoeba on the surface after 90 minutes of incubation (seen at 4x magnification). Photo: Hari Peguda, BOptom, UNSW Scientia PhD Scholar. Click image to enlarge. |
Contact lenses not only transmit organisms to the eye—they also retain them for a longer period of time. “We have different ways of protecting our corneas from infection, including our eyelids, blinking mechanism, tear film antimicrobials and sloughing of the ocular surface epithelial cells,” Dr. Carnt explains.
A contact lens affects the homeostasis of all these defense mechanisms. “If you are in the shower without contact lenses and water gets in your eyes, blinking is enough to wash away or dilute the organisms because it will cause your eyes to water,” says Dr. Carnt. With a contact lens in place, there is an opportunity for the organisms to stick on the front or back of the lens and get trapped underneath the lens, subsequently remaining on the eye longer.
Furthermore, Acanthamoeba contains a mannose-binding protein that can facilitate attachment to the cornea. This can happen when epithelial cells are irritated—for example, by microtrauma from the contact lens—causing the infective process to ensue.12
 |
|
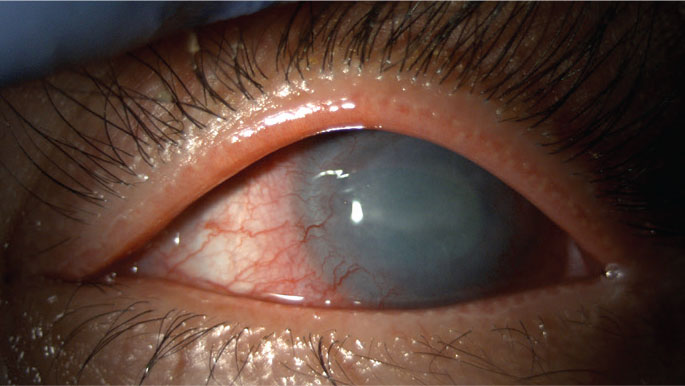
Clinical presentation of Acanthamoeba keratitis. Photo: Suzanne Sherman, OD. Click image to enlarge. |
 |
|
In vivo confocal microscopy of organism cysts in the cornea. Photo: Suzanne Sherman, OD. Click image to enlarge. |
Acanthamoeba has a defense mechanism of its own. When it is threatened by lack of nutrients, temperature extremes or pH changes, it encysts into a double-walled inactive, sessile form that can exist for months to years.4 This is one of the main reasons AK has such poor outcomes, with 50% of patients needing treatment for more than 12 months and subsequent reduced quality of life, impacting reading, mobility and emotional well-being.13
The best defense against AK is prevention. By switching all wearers from reusable soft to daily disposable lenses, cases of AK would halve.10 However, daily disposables are not without risk themselves. The chance of AK in daily disposables can be further reduced by not reusing, sleeping or showering in the lenses.10 The biggest reduction in risk is regularly seeing an eyecare practitioner.10 “We are in a powerful position to educate wearers how to use contact lenses safely and enjoy the benefits of healthy contact wear,” sums up Dr. Carnt.
Dr. Shovlin, a senior optometrist at Northeastern Eye Institute in Scranton, PA, is a fellow and past president of the American Academy of Optometry and a clinical editor of Review of Optometry and Review of Cornea & Contact Lenses. He consults for Kala, Aerie, AbbVie, Novartis, Hubble and Bausch + Lomb and is on the medical advisory panel for Lentechs.1. Clarke DW, Niederkorn JY. The immunobiology of Acanthamoeba keratitis. Microbes and infection / Institut Pasteur. 2006;8(5):1400-5. 2. Radford CF, Minassian D, Dart JKG. Acanthamoeba keratitis in England and Wales: incidence, outcome and risk factors. Br J Ophthalmol. 2002;86:536-42. 3. Carnt N, Hoffman JM, Verma S, et al. Acanthamoeba keratitis: confirmation of the UK outbreak and a prospective case-control study identifying contributing risk factors. Br J Ophthalmol. 2018;102(12):1621-8. 4. Kilvington S, White DG. Acanthamoeba biology, ecology and human disease. Rev Med Microbiol. 1994;5:12-20. 5. Carnt NA, Subedi D, Lim AW, et al. Prevalence and seasonal variation of Acanthamoeba in domestic tap water in greater Sydney, Australia. Clinical & Exp Optom : J of the Austral Optometrical Assoc. 2020;103(6):782-6. 6. Carnt NA, Subedi D, Connor S, Kilvington S. The relationship between environmental sources and the susceptibility of Acanthamoeba keratitis in the United Kingdom. PloS One. 2020;15(3):e0229681. 7. Rayamajhee B, Subedi D, Won S, et al. Investigating domestic shower settings as a risk factor for Acanthamoeba keratitis. Water-Sui. 2020;12(12). 8. Kilvington S, Gray T, Dart J, et al. Acanthamoeba keratitis: the role of domestic tap water contamination in the United Kingdom. Invest Ophthalmol Vis Sci. 2004;45(1):165-9. 9. Larkin DFP, Kilvington S, Easty DL. Contamination of contact lens storage cases by Acanthamoeba and bacteria. Br J Ophthalmol. 1990;74:331-3. 10. Carnt NM, Dart J. Acanthamoeba keratitis risk factors for daily wear contact lens users: a case control study. Ophthalmology. 2022. 11. Stapleton F, Naduvilath T, Keay L, et al. Risk factors and causative organisms in microbial keratitis in daily disposable contact lens wear. PloS One. 2017;12(8):e0181343. 12. Clarke DW, Niederkorn JY. The pathophysiology of Acanthamoeba keratitis. Trends Parasitol. 2006;22(4):175-80. 13. Carnt NA, Man REK, Fenwick EK, Lamoureux EL, Keay LJ. Impact of Acanthamoeba keratitis on the vision-related quality of life of contact lens wearers. Cornea. 2022;41(2):206-10. |

