In life––especially in America––we often subscribe to the theory that more is better. Restaurants entice us with “super-sized” portions, while TV manufacturers offer us large screens, with HD, 3D and numerous other extras that appeal to our sense of consumeristic gluttony.

In medicine, the principle of “more is better” may also be seen, although it is usually more subtle and designed to facilitate compliance or improve patient convenience. For example, Zithromax (azithromycin, Pfizer) first entered the U.S. market in 1996 with its now famous Z-Pak––six 250mg tablets designed to be taken over a five-day course. Several years later, Pfizer introduced the TRI-PAK, which consisted of three 500mg tablets that were to be taken just once daily for three days. Similarly, 125mg and 250mg Diamox (acetazolamide, Duramed Pharmaceuticals) tablets have been discontinued in the United States in favor of 500mg extended release capsules (although generic acetazolamide tablets are still available).
Recent Formualtion Alterations
• Alphagan. It came as a genuine surpise in 2001 when Allergan announced that it would be launching a new product called Alphagan-P (0.15% brimonidine tartrate). Alphagan-P, as we now know, ultimately replaced Allergan’s previous product, Alphagan (0.2% brimonidine tartrate). One of the unique differences between the older Alphagan and the newer Alphagan-P was the elimination of its preservative, benzalkonium chloride. Instead, Alphagan-P was preserved with Purite. Purite is a proprietary formulation of sodium perborate, a microbiocide with broad-spectrum antimicrobial activity and low cellular toxicity. Additionally, Purite is one of just a few “disappearing preservatives” that rapidly breaks down into water, sodium and chloride ions, and oxygen following administration and exposure to light.
But, the most intriguing change in the newer formulation was that Alphagan-P actually contained 0.05% less of the active drug (brimonine) than its predecessor. Interestingly, brimonine 0.15% was shown to lower IOP as effectively as brimonine 0.2% when dosed b.i.d. in clinical trials.1 And, while that trial showed that there were no statistically significant differences between the two treatment groups in the incidence of adverse events, a subsequent study from Korea found that ocular allergic reaction was more frequent and severe with Alphagan as compared with Alphagan-P.2
Several years later, Allergan announced yet another modification to Alphagan-P. This most recent formulation also contained Purite, but Allergan had further reduced the concentration of brimonidine from 0.15% to just 0.1%. In clinical comparisons, the 0.1% formulation was judged to be as effective as the 0.15% concentration in lowering intraocular pressure when dosed b.i.d.3 Additionally, both formulations were equally well-tolerated.3 And so, in the course of nine years, research allowed Allergan to reduce the amount of active drug in its Alphagan product by 50%, albeit with no decrease in clinical efficacy.
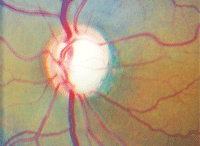
Glaucoma patients, such as this one, may experience fewer adverse side effects from newer IOP-lowering agents that have been reformulated with lower active drug concentrations.
• Lumigan. In August 2010, the U.S. Food and Drug Administration approved a new formulation of Lumigan (Allergan) that contained just 0.01% bimatoprost compared to the 0.03% formulation that had been utilized since 2001. In a large, multi-center clinical trial published earlier this year, bimatoprost 0.01% demonstrated equivalent therapeutic efficacy to bimatoprost 0.03%.4 Additionally, the overall incidence of treatment-related adverse events was significantly lower in the bimatoprost 0.01% group compared with the bimatoprost 0.03% group, including a lower tendency for conjunctival hyperemia.4 However, animal studies have shown that the 0.01% formulation of bimatoprost was actually more irritating and induced greater conjunctival congestion and swelling than bimatoprost 0.03%.5 The authors of this paper suggested that the difference may be attributed to higher levels of benzalkonium chloride, which are actually four times higher (0.02% vs. 0.005%) in the 0.01% bimatoprost formulation.5
• TobraDex ST. The reduction of active drug concentrations in ophthalmic medications is apparently not unique to glaucoma therapy, either. Another recently introduced medication, TobraDex ST (tobramycin and dexamethasone, Alcon) seems to be following a similar trend. While TobraDex ST contains the same concentration of tobramycin (0.3%) as the original TobraDex formulation, ST contains just half the dexamethasone (0.05% compared to 0.1% in TobraDex).6 Yet, despite this substantial difference, TobraDex ST appears to be clinically equivalent to the older formulation.
One reason for this unique capacity is likely related to the vehicle of TobraDex ST, which contains xanthan gum. Xanthan gum is a polysaccharide that is produced by the fermentation of glucose or sucrose via the bacterium Xanthomonas campestris; it is widely utilized as a rheology modifier (i.e., a thickening agent that allows solids to remain suspended in a fluid mixture) in a variety of foods, consumer products and pharmaceutical agents.7 Head-to-head studies of TobraDex and TobraDex ST have shown the newer formulation to have superior settling characteristics, greater in-vitro bactericidal activity and higher relative tissue concentrations for the conjunctiva, cornea and aqueous humor in both animal and human trials.6
Lower Dose, Higher Efficacy
As drug delivery systems are improved and new research continues to indicate that clinical efficacy can be achieved with lower doses of medication, we may see similar modifications to some of our more well-known products. And while it may seem “un-American” to “get less for our dollar,” in the end, it is really about maximizing efficacy, minimizing side-effects, improving compliance and providing the very best treatment options for our patients.
Dr. Kabat is a consultant to Alcon and Inspire Pharmaceuticals. Dr. Sowka is a consultant for Alcon. Neither author has a direct financial interest in any of the products mentioned.
1. Mundorf T, Williams R, Whitcup S, et al. A 3-month comparison of efficacy and safety of brimonidine-purite 0.15% and brimonidine 0.2% in patients with glaucoma or ocular hypertension. J Ocul Pharmacol Ther. 2003 Feb;19(1):37-44.
2. Kim CY, Hong S, Seong GJ. Brimonidine 0.2% versus brimonidine Purite 0.15% in Asian ocular hypertension. J Ocul Pharmacol Ther. 2007 Oct;23(5):481-6.
3. Cantor LB, Safyan E, Liu CC, Batoosingh AL. Brimonidine-purite 0.1% versus brimonidine-purite 0.15% twice daily in glaucoma or ocular hypertension: a 12-month randomized trial. Curr Med Res Opin. 2008 Jul;24(7):2035-43.
4. Katz LJ, Cohen JS, Batoosingh AL, et al. Twelve-month, randomized, controlled trial of bimatoprost 0.01%, 0.0125%, and 0.03% in patients with glaucoma or ocular hypertension. Am J Ophthalmol. 2010 Apr;149(4):661-71.
5. Ogundele AB, Li G, Ellis JJ. Impact of topical bimatoprost 0.01% and bimatoprost 0.03% on conjunctival irritation in rabbits. Clin Ophthalmol. 2010 Feb 18;4:77-80.
6. Scoper SV, Kabat AG, Owen GR, et al. Ocular distribution, bactericidal activity and settling characteristics of TOBRADEX® ST Ophthalmic Suspension compared with TOBRADEX® Ophthalmic Suspension. Adv Ther. 2008 Feb;25(2):77-88.
7. Ceulemans J, Vinckier I, Ludwig A. The use of xanthan gum in an ophthalmic liquid dosage form: rheological characterization of the interaction with mucin. J Pharm Sci. 2002 Apr;91(4):1117-27.

