Filamentary keratitis (FK) is a bilateral disease that has a characteristic appearance with strands of cellular material attached to the cornea at one or both ends. A patient usually presents with a foreign body sensation and mild to severe pain. The strands or filaments—composed of mucus, epithelial cells and lipids—are easily observed.1 Epithelial cells around local areas of focal degeneration produce the filaments, which are smaller and thicker than in other conditions.2
The histopathology of this disease is not totally clear, although a postmortem study does indicate inflammatory groups of cells and some fibroblasts below the basal epithelium.3 This study indicates that the inflammatory process somehow disrupts the basement membrane and Bowman’s layer.3 It supports the theory that FK is a result of damage to both the epithelial membrane and the cells.3 The treatment options are varied but should be directed at the corneal receptor sites, the excess mucus or the underlying condition that has caused the corneal abnormality.1
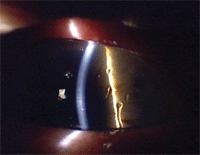
Corneal filaments often lead to foreign body sensation. Courtesy: Paul Karpecki, O.D.
Besides experiencing the foreign body sensation of the filaments, many patients have an increased blink rate that can even result in a blepharospasm.4 The most common condition that can cause this disease is aqueous-deficient dry eye (keratoconjunctivitis sicca [KCS]).5
Patient History
A 38-year-old Hispanic female presented to the clinic on February 4, 2010, with a complaint that she had been experiencing moderate to severe pain in both eyes for a month. She had already been seen by her primary care physician and was treated with antibiotic drops for an eye infection. On presentation, she had pain (6 on a scale of 10), photophobia, redness, itching and decreased visual acuity O.U. Also, she reported that her eyes were swollen shut in the morning. There was no history of ocular trauma or surgery.
Ocular medications included polymyxin b sulfate/trimethoprim ophthalmic drops q.i.d. O.U. Current systemic medications were Allegra-D 24 hour (fexofenadine HCl 180mg/pseudoephedrine HCl 240mg, Sanofi-Aventis), generic methylprednisolone 4mg oral tablets in a dose pack, Zegerid 20mg capsules (omeprazole/sodium bicarbonate, Santarus) and oral contraceptives. She had a surgical history of cesarean section, but no known medical allergies. There was no pertinent family or ocular history.
Diagnostic Data
The patient’s entering uncorrected visual acuity measured 20/70 O.D. and 20/200 O.S. She had no habitual spectacle or contact lens prescription. Pinhole showed improvement to 20/40- O.D. and 20/50- O.S. Pupils were equal, round and reactive to light and accommodation, with no evidence of afferent defect. Extraocular muscles were unrestricted in all fields of gaze, and cover testing showed orthophoria. She was quite photophobic, and the palpebral aperture was minimized due to her discomfort.
Anterior segment examination by slit lamp and fluorescein instillation revealed 2+ conjunctiva injection, 3+ superficial punctate keratitis, 3+ filamentary keratitis, 2+ palpebral papillae and a decreased tear film in both eyes.
Differential diagnoses included:
- Conjunctival/corneal foreign body.
- Chemical conjunctivitis.
- Filamentary keratitis.
- Keratoconjunctivitis sicca.
- Bacterial/viral keratoconjunctivitis.
There was no foreign body stain and no history of being in an environment that could have produced a foreign body. Ocular inspection showed no foreign body on the corneal or conjunctival surfaces, even with lid eversion. The history did not support a diagnosis of bacterial or viral infection, and there was no discharge. There was no history of a chemical contamination, and the ocular signs were definitely conclusive for FK.
Diagnosis
Because there were corneal filaments, photophobia and a foreign body sensation, we diagnosed the patient with FK. There are two common causative factors for FK—dry eye and trauma—so after the origin was determined, treatment could be initiated.
Treatment Approach
FK and the resultant filaments cause foreign body sensation and photophobia. Treatment consists of removing the filaments and increasing tear volume. After instilling 1gtt proparacaine hydrochloride 0.5% O.U., we removed the filaments with a moistened cotton swab.
The patient was in obvious discomfort, so we postponed tonometry until her anterior segment was not inflamed. The angles were Grade 4 O.U. using the Van Herrick method, and she had brown irises. The patient had a clear crystalline lens with no anterior chamber cells or flare O.U.
We scheduled a dilated fundus exam for a later visit, but undilated direct ophthalmoscopy showed no apparent posterior segment pathology. Because of the FK and dryness, we ruled out infection. We discontinued the polymyxin b/trimethoprim sulfate drops, and we recommended Refresh Optive (Allergan) O.U. q.i.d. and Pred Forte (prednisolone acetate, Allergan) O.U. q3h while awake.
We asked the patient to return in four days. We told her to keep the anterior surface lubricated by using the Optive as frequently as necessary, with a minimum dosing frequency of q.i.d.
Follow-Up
• Visit 1. On February 9, the patient returned for her follow-up examination. She said that she felt “only a little bit better,” with pain of 4 on a scale of 10 and some residual itching and light sensitivity that prevented her from working. Her uncorrected distance visual acuity was 20/40- O.D. and 20/70- O.S., with pinhole of 20/40 O.D. and 20/50 O.S. The itching was indicative of an allergic response, but we did not prescribe any allergy drops because she was already using a steroid. She was compliant with the treatment plan.
Slit lamp examination and fluorescein instillation showed 2+ FK still present, and she had superficial punctate keratopathy (SPK) of 2+ O.U. We used a moistened cotton swab to remove the FK filaments. IOP measured 17mm Hg O.D. and 16mm Hg O.S.
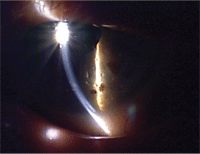
The filaments themselves are composed of cytokeratins that are covered in mucin. Courtesy: Paul Karpecki, O.D.
The patient had finished her methylprednisolone tablets and was still taking oral contraceptives, Zegerid and Allegra-D. She had still been using the polymyxin b/trimethoprim drops. Her understanding of the English language was questionable, but fortunately her daughter came with her. We explained to both of them that she could have had an allergic reaction to the polymixin b/trimethoprim and told her to discontinue that medication.
We added Soothe XP (Bausch + Lomb) q.i.d. O.U., because of its increased viscosity compared to most artificial tears. We instructed her to continue the Pred Forte q.i.d. and substitute the Soothe XP for the Optive. We again stressed ocular lubrication, and educated her about KCS. During this examination, we recommended punctal occlusion, but she decided to wait. We asked the patient to return in another four days.
• Visit 2. The patient returned on February 12. Her uncorrected distance acuity was now 20/40- O.U. and she still had many of the same symptoms, although slightly reduced. Pain was 4 on a scale of 10; she still complained of photophobia and foreign body sensation. IOP measured 18mm Hg O.U. Slit lamp examination with fluorescein instillation showed trace FK (unresolved) and 2+ SPK O.U. We instructed her to continue both the Pred Forte and the Soothe XP O.U.
After discussion, we again recommended silicone plugs (0.6mm) in the lower puncta. We chose silicone plugs because of the long-term nature of the underlying KCS condition. Silicone plugs were inserted at this visit. We told her to continue ocular lubrication more often than she may think necessary to resolve the FK. We postponed the posterior segment exam until her discomfort subsided. We explained that a second set of punctal plugs would help alleviate symptoms and may be needed at the next visit. We scheduled her to return in two weeks.
• Visit 3. The patient returned on February 24, reporting that she felt 30% better with no pain. There was no change in systemic medications, and she was still using Pred Forte and Soothe XP. Her uncorrected visual acuity was 20/50 O.U. Slit lamp examination revealed that the lower punctal plugs were in good position. Additionally, we noted 2+ SPK O.U. without any FK. This was the first time that she had no filaments and her condition seemed to be improving. IOP measured 17mm Hg O.U.
We inserted a second set of silicone plugs (0.6mm) into the upper puncta. We stressed ocular lubrication and added Systane (Alcon) O.U. q.i.d. to her regimen. We instructed her to continue the Pred Forte and Soothe XP, and scheduled her to return for another follow-up appointment in two weeks.
• Visit 4. On March 12, she returned for her fourth follow-up. For the first time, she reported that her eyes did not feel dry. Uncorrected distance visual acuity was 20/30 O.D. and 20/50 O.S. She was compliant with her medications.
Slit lamp exam and fluorescein instillation showed that her FK had resolved, although she still exhibited 1+ SPK. All four punctal plugs were in place without epiphora. Her IOP measured 14mm Hg O.D. and 13mm Hg O.S.
We dilated the patient with 2.5% Neo-Synephrine (phenylephrine hydrochloride 0.5%, Bayer Healthcare) and 1% tropicamide. Then we performed a fundus exam––first with the slit lamp and a Volk Wide Field lens, and then with a binocular indirect ophthalmoscope. The fundus vasculature was normal, the lens was clear and the retina had no apparent pathology. Her cup-to-disc ratio was 0.4 x 0.4 O.U., with normal neuroretinal rim and color.
Ocular lubrication was stressed, and we instructed her to continue with the treatment plan.
• Visit 5. The patient returned on March 26, stating that she felt 100% better. Slit lamp examination with fluorescein instillation showed complete resolution of the FK O.U., and for the first time she had only trace SPK. All four punctal plugs were in place, and she had no epiphora. She was compliant with the drops. IOP measured 15mm Hg O.D. and 14mm Hg O.S.
Her uncorrected visual acuity was 20/25 O.D. and 20/40 O.S. Because her cornea appeared relatively normal for the first time, refraction was performed and her resultant prescription -0.50 +0.25D x 085 O.D. and -0.75D sphere O.S. yielded a corrected visual acuity of 20/20 O.U. She now believed that she could return to work.
We tapered the Pred Forte to t.i.d. for a week, then b.i.d. for a week, and finally q.d. for a week. We asked her to continue her artificial tear regimen of Systane and Soothe XP q.i.d. O.U. We discussed her medications, explaining that both Zegerid and some oral contraceptives could cause KCS and the resultant FK. We suggested that she talk with her medical practitioner(s) about the possibility of changing to more “eye-friendly” medications. We scheduled her to return in one month.
• Visit 6. The patient returned on April 23 with no dry eye complaints. She exhibited complete resolution of the KCS and FK. She believed that her issue was resolved and her eyes felt normal, although she was experiencing some itching. Corrected visual acuity was 20/20 O.U. Slit lamp exam with fluorescein instillation showed no SPK, FK or epiphora. Additionally, all four punctal plugs were in place. IOP measured 15mm Hg O.D. and 16mm Hg O.S.
We explained that, although resolution had occurred, this disease process could reoccur. She had spoken to her general medical practitioner and he was in the process of switching her systemic medications to prevent a recurrence of KCS. Once again, we stressed ocular lubrication, and instructed her to continue the current drop regimen. We added Elestat 0.05% (epinastine HCl, Inspire Pharmaceuticals) O.U. b.i.d. for allergic conjunctivitis during the allergy season, and requested that she return for an annual exam—or sooner if symptoms reappeared.
Discussion
Although the pathogenesis of FK is not truly understood, the inflammatory cells cause the epithelial and mucus strands to appear. KCS seems to be the main cause of FK formation.4 The filaments themselves are composed of cytokeratins (CK-12 positive) that are covered in mucin (MUC5AC), including broken cells and DNA.6 The clinical challenge with this disease is not only to understand what the filaments are composed of, but also to identify the most appropriate treatment to resolve the disease in the shortest amount of time.
Non-resolution or chronic FK can result in vascularization of the cornea.7 Mechanical removal of the filaments results in short-term relief for the patient, but the filaments will re-form within a short time unless the underlying cause of FK is addressed. Conventional treatment can be administered with hyperosmotic sodium chloride solution t.i.d. to q.i.d. This treatment works best for FK associated with acute or traumatic diseases of the cornea, and usually resolves the presentation within one week.8 However, KCS-induced FK responds more slowly, with 89% resolution of symptoms in about a month.8
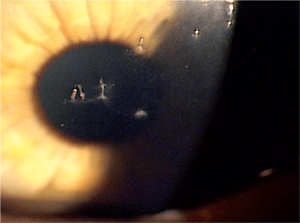
Although the pathogenesis of FK is not truly understood, the inflammatory cells cause the epithelial and mucus strands to appear. Courtesy: Paul Karpecki, O.D.
Punctal occlusion causes 100% resolution of aqueous tear deficiency-induced FK.9 Some optometrists advocate temporary punctal plugs; however, in the management of this patient’s case, permanent or silicone plugs were a better choice because of possible recurrence.10 Temporary plugs would have helped, but the major problem with them is they are hard to see in the puncta—making it difficult to determine if they are working properly. Also, due to the nature of FK, silicone plugs were used because the worst-case scenario would have been to remove them.
Some literature suggests using Voltaren 0.1% (diclofenac sodium, Novartis Pharmaceuticals) q.i.d. as an alternative to 5% sodium chloride. There was a faster resolution seen with Voltaren than sodium chloride solution in patients with FK caused by Sjögren’s syndrome.11 However, the Novartis package insert lists corneal thinning and perforation as potential side effects of long-term medication use. Because of this warning and the possible chronic course of this disease, the medication must be used with caution as a solitary pharmaceutical agent or in combination with topical steroids.
Bandage contact lens use was another option for treatment, and we considered it for this patient. There has been some concern among clinicians that bandage contact lenses may retain the moisture in the lens rather than helping with the KCS and FK disease states, and that the corneal strands could be trapped under them.
For these reasons, we didn’t pursue this option. We ultimately chose punctal occlusion because it was the best option to help our patient retain corneal moisture. We decided that we could try the bandage contact lens at a later date after the FK resolved, if necessary, to treat any remaining KCS.
Our patient had a clear case of KCS-induced FK. Her reluctance for silicone punctal occlusion delayed resolution, but after she consented to plug insertion, her resolution fell within the normal values in approximately one month.9-11 Once resolution of FK was achieved, her vision returned to normal and refraction proved that she could achieve 20/20 vision O.U. She was able to resume normal activities and return to work without the pain, grittiness and foreign body sensation that plagued her.
After the patient had complete resolution, a dilated exam showed a normal posterior segment. We prescribed Elestat 0.05% for allergic conjunctivitis, along with artificial tears q.i.d. to prevent a recurrence of FK. Although there was no epiphora present at the last follow-up, we will monitor the patient for corneal inflammation secondary to waste and allergic products. If inflammation occurs, the solid plugs may have to be replaced with tear flow plugs that allow drainage of those waste products.
Dr. Simon has been practicing optometry for more than 20 years and is currently a staff member at the McCabe Vision Center in Murfreesboro, Tenn.
1. Wright P. Filamentary keratitis. Trans Ophthalmol Soc U K. 1975 Jul;95(2):260-6.
2. Maudgal PC, Missotten L, Van Deuren H. Study of filamentary keratitis by replica technique. Albrecht Von Graefes Arch Klin Exp Ophthalmol. 1979 Jul 2;211(1):11-21.
3. Zaidman GW, Geeraets R, Paylor RR, Ferry AP. The histopathology of filamentary keratitis. Arch Ophthalmol. 1985 Aug;103(8):1178-81.
4. Diller R, Sant S. A case report and review of filamentary keratitis. Optometry. 2005 Jan;76(1):30-6.
5. Albietz J, Sanfilippo P, Troutbeck R, Lenton LM. Management of filamentary keratitis associated with aqueous-deficient dry eye. Optom Vis Sci. 2003 Jun;80(6):420-30.
6. Tanioka H, Yokoi N, Komuro A, et al. Investigation of the corneal filament in filamentary keratitis. Invest Ophthalmol Vis Sci. 2009 Aug;50(8):3696-702.
7. Kowalik BM, Rakes JA, Filamentary keratitis--the clinical challenges. J Am Optom Assoc. 1991 Mar;62(3):200-4.
8. Hamilton W, Wood TO. Filamentary keratitis. Am J Ophthalmol. 1982 Apr;93(4):466-9.
9. Tuberville AW, Frederick WR, Wood TO. Punctal occlusion in tear deficiency syndromes. Ophthalmology. 1982 Oct;89(10):1170-2.
10. Fayet B, Bernard JA, Ammar J, et al. Treatment of dry eye by temporary punctum plug. Comparison with a control group, J Fr Ophtalmol. 1990;13(3):123-33.
11. Avisar R, Robinson A, Appel I, et al. Diclofenac sodium, 0.1% (Voltaren Ophtha), versus sodium chloride, 5%, in the treatment of filamentary keratitis. Cornea. 2000 Mar;19(2):145-7.

