The term “epidemic” has been increasingly used to describe the public health challenge of excess weight and obesity. Obesity is a complex condition with many causal contributors, some modifiable and others that are largely beyond individuals’ control. There is widespread agreement among the general public and the health care community that it is reasonable to call obesity a disease.1

Obesity causes great suffering, because it causally contributes to ill health, functional impairment, reduced quality of life, serious disease and greater mortality.2
Several ophthalmic conditions and diseases are linked to excess weight, some of them sight-threatening. (See “Common Systemic Co-morbidities of Obesity.”)
We as optometrists typically care for several patients each day who are overweight or obese. Pediatric optometrists are seeing children, adolescent and teenage patients gaining weight in startling amounts at rapid rates.
Obese persons—including patients as well as their health care providers—may be subject to enormous societal stigma and discrimination. They deserve better.
How should we as clinicians and as an optometric community respond?
What is Obesity?
Obesity represents a state of excess storage of body fat. (Although similar, the term overweight is defined as an excess body weight for height.) Body mass index (BMI) is commonly used to define obesity. BMI is calculated as a person’s weight/height2, where weight is in kilograms and height is in meters.
The most widely accepted classification is the World Health Organization (WHO) criteria based on BMI.3 Under this convention for adults:
- Grade 1 (simply called overweight) is a BMI of 25 to 29.9 kg/m2.
- Grade 2 (commonly called obesity) is a BMI of 30 to 39.9 kg/m2.
- Grade 3 (commonly called severe obesity) is a BMI greater than or equal to 40 kg/m2.

The definition of obesity in children involves BMIs greater than the 85th (commonly used to define overweight) or the 95th (commonly used to define obesity) percentile, respectively, for age-matched and sex-matched control subjects.1-3
The pathogenesis of obesity is far more complex than the simple paradigm of an imbalance between energy intake and energy output. Obesity is far more than the mere result of too much eating and/or too little exercise. However, the prevalence of inactivity in developed countries is a considerable contributing factor.1
Approximately 100 million adults in the United States are at least overweight or obese—that’s 35% of women and 31% of men older than 19 years. The numbers among children and adolescents are just as staggering. Approximately 20% to 25% of children are either overweight or obese.4
The prevalence is even greater than this in some minority groups, including Pima Indians, Mexican Americans and African Americans.4 Conservative estimates suggest that the management of obesity costs approximately $100 billion annually.5
A Team Approach
In contemporary models of chronic disease management, the patient is no longer a passive follower of instructions, but rather an empowered, central member of her health care team. Effective management of obesity must be based on a partnership between a highly motivated patient and a committed team of health professionals.
In addition to the optometrist, the team should ideally include the primary care physician, psychologist or psychiatrist, physical and exercise therapists, dietitians, and other subspecialists depending on the co-morbidities of the individual patient. A case manager (usually a nursing or social services professional) often acts as a facilitator, coordinator and patient advocate.
Effective obesity medical management programs focus on both treatment and education. Culturally and linguistically appropriate print and multimedia materials can assist in this regard.6 Methods of obesity treatment may include dietary programs, exercise programs, behavioral changes (including sufficient sleep), medications and bariatric surgical care.7
Optometry’s Role
As the primary eye care clinicians, we must be aware of those ocular conditions that are linked with excess weight and obesity. It’s our responsibility to recognize, diagnose and manage floppy eyelid syndrome, age-related macular degeneration, glaucoma (primary open-angle and normal tension), papilledema in pseudotumor cerebri, diabetic and hypertensive retinopathies, thyroid eye disease, and non-arteritic anterior ischemic optic neuropathy (NAION).8
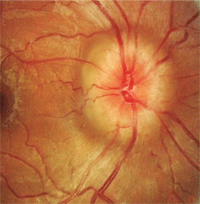
Optic disc edema in an obese female with pseudotumor cerebri.
Though it may be easier to leave all of the “obesity discussions” to other members of the health care team, we eye care providers have a duty to counsel our patients. With repeated experience and a caring attitude, it eventually becomes less awkward to discuss with our patients the importance of addressing excess weight, focusing on the benefits (both ocular and overall) of nutrition and physical activity.
Obesity is epidemic in the United States and many other developed countries. The burden of disease exists at many levels––from quality of life issues to unprecedented health care system expense. It will likely take a concerted, nationwide effort and determined investment across a generation to reverse the alarming trends.
Stigmatizing people will not reduce the consequences of obesity. Geneticists and other scientists, who study obesity as a biological problem, suggest that we fight a “war on obesity, not the obese.”9
Coming in July: Part 2—Obesity and the eye.
1. Jung RT. Obesity as a disease. Br Med Bull. 1997;53(2):307-21.
2. Wijga AH, Scholtens S, Bemelmans WJ, et al. Comorbidities of obesity in school children: a cross-sectional study in the PIAMA birth cohort. BMC Public Health. 2010 Apr 9;10(1):184.
3. World Health Organization. Obesity: preventing and managing the global epidemic. Report of a WHO Consultation. WHO Technical Report Series 894. Geneva: World Health Organization, 2000.
4. Proimos J, Sawyer S. Obesity in childhood and adolescence. Aust Fam Physician. 2000 Apr;29(4):321-7.
5. Thompson D, Wolf AM. The medical-care cost burden of obesity. Obes Rev. 2001 Aug;2(3):189-97.
6. Stolley MR, Fitzgibbon ML, Schiffer L, et al. Obesity reduction black intervention trial (ORBIT): six-month results. Obesity (Silver Spring). 2009 Jan;17(1):100-6.
7. Cigaina V. Gastric pacing as therapy for morbid obesity: preliminary results. Obes Surg. 2002 Apr;12 Suppl 1:12S-16S.
8. Cheung N, Wong TY. Obesity and eye diseases. Surv Ophthalmol. 2007 Mar-Apr;52(2):180-95.
9. Friedman JM. A war on obesity, not the obese. Science. 2003 Feb 7;299(5608):856-8.

