 |
Q:
A six-year-old Caucasian male presented with severe blepharokeratoconjunctivitis (BKC) associated with photophobia, watering, irritation and reduced acuity. He had significant corneal insult with vascularization and scarring. What are my options?
A:
BKC is a chronic inflammatory condition of the lid margin accompanied by conjunctivitis and keratopathy, says Paymaun Asnaashari, OD, who practices in California. The pathogenesis is associated with bacterial species that colonize the lids and ocular surface and release exotoxins.1,2 This leads to a delayed hypersensitivity response, stimulating the production and release of proinflammatory molecules.1,2 These cause the formation of prostaglandins, leukotrienes and other molecules that result in tear film destabilization and neutrophil chemotaxis inflammation.3,4
BKC signs and symptoms include tearing, photophobia, red eye, blepharitis, hordeolum, recurrent chalazium, phlyctenular conjunctivitis, keratitis and corneal complications.1,2,3,5 While presentation is similar between children and adults, visual outcomes are generally worse in kids with corneal involvement.1 The incidence of BKC in younger patients is 15%, with a mean age of disease onset of six years old.1,5
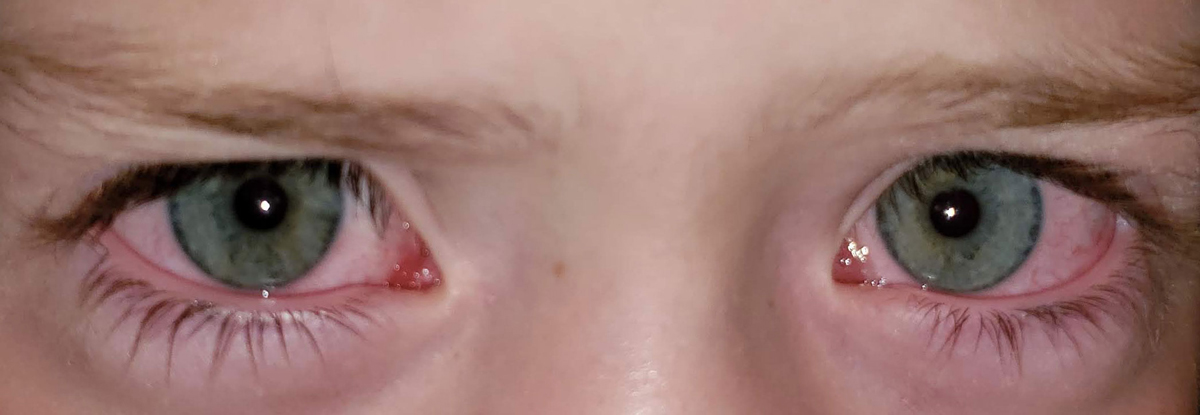 |
| Aggressively treat BKC affecting a child’s eyes. Photo by Christine W. Sindt, OD. Click image to enlarge. |
Vision Preservation
Dr. Asnaashari recommends immediate treatment when a child’s vision is affected. Paracentral and central opacity can lead to deprivation amblyopia and must be addressed early and aggressively to avoid permanent vision loss.
Treatment helps reduce the stimulus for the disease by lowering the population of Staphylococci, improving meibomian gland function and reducing the host’s local immune response.6 Options include lid hygiene, topical and systemic antibiotics and topical steroids.
Daily lid hygiene removes debris along the lid margin, and long-term oral antibiotics help control disease progression.3 The severity of this case warrants the use of macrolides, with erythromycin being the preferred choice in children younger than eight for its safety profile.6,7,8 Systemic macrolides work by penetrating the meibomian glands, affecting meibum composition and inhibiting bacterial protein synthesis and lipase production, notes Dr. Asnaashari.
He suggests short-term topical antibiotics when there is concomitant blepharitis or other infections within the lids and topical, broad-spectrum antibiotic ointments, drops or a combination to reduce bacterial colonization along the eyelid margin. Topical steroids are the most effective option to control ocular surface and corneal inflammation, according to Dr. Asnaashari. In this case, a short course of intensive treatment is needed to control the severe inflammation and minimize scar formation. If long-term treatment is warranted, he advises monitoring patients closely for ocular hypertension and cataract.
Oral omega-3 supplementation is an ancillary therapy in BKC.1,3 Omega-3s inhibit synthesis of proinflammatory mediators by preventing the creation of prostaglandins and promoting a healthier lipid profile of meibomian gland secretions.1,9 In more severe cases of BKC, however, omega-3s alone likely won’t be sufficient to control the inflammation.
“BKC has the potential for severe corneal complications and vision loss,” says Dr. Asnaashari. “Early treatment could prevent or minimize these complications. Many effective options are available, and understanding each is important in promoting successful outcomes.”
1. Rodríguez-García A, González-Godínez S, López Rubio S. Blepharokeratoconjunctivitis in childhood: corneal involvement and visual outcome. Eye (Lond). 2015;30(3):438-46. 2. Tuft SJ. Ento Key. External eye disease and the oculocutaneous disorders. entokey.com/external-eye-disease-and-the-oculocutaneous-disorders/. June 4, 2016. Accessed May 7, 2020. 3. Daniel MC, O’Gallagher M, Hingorani M, et al. Challenges in the management of pediatric blepharokeratoconjunctivis / ocular rosacea. Expert Rev Ophthalmol. 2016;11(4):299-309. 4. Suzuki T. Meibomitis-related keratoconjunctivitis: implications and clinical significance of meibomian gland inflammation. Cornea. 2012;31(Suppl 1):S41-4. 5. Gupta N, Dhawan A, Beri S, et al. Clinical spectrum of pediatric blepharokeratoconjunctivitis. J AAPOS. 2010;14(6):527-9. 6. Viswalingam M, Rauz S, Morlet N, et al. Blepharokeratoconjunctivitis in children: diagnosis and treatment. Br J Ophthalmol. 2005;89(4):400-3. 7. Farpour B, McClellan KA. Diagnosis and management of chronic blepharoconjunctivitis in children. J Pediatr Ophthalmol Strabismus. 2001;38(4):207-12. 8. Meisler DM, Raizman MB, Traboulsi EI. Oral erythromycin treatment for childhood blepharokeratitis. J AAPOS. 2000;4(6):379-80. 9. Macsai MS. The role of omega-3 dietary supplementation in blepharitis and meibomian gland dysfunction (an AOS thesis). Trans Am Ophthalmol Soc. 2008;106:336-56. |

