 A 46-year-old white male presented complaining of blurred vision in his left eye that had persisted for a month. He also reported a floater in the same eye. Both his ocular and medical histories were unremarkable, and he takes no medications.
A 46-year-old white male presented complaining of blurred vision in his left eye that had persisted for a month. He also reported a floater in the same eye. Both his ocular and medical histories were unremarkable, and he takes no medications.
On examination, the patients best-corrected visual acuity measured 20/20 O.D. and 20/25 O.S. Extraocular motility testing was normal. Confrontation visual fields were full to careful finger counting O.U. His pupils were equally round and reactive, with no afferent pupillary defect. Amsler grid testing was normal O.D., but showed a small, localized area of metamorphopsia inferior nasal to fixation O.S. The anterior segment examination was unremarkable.
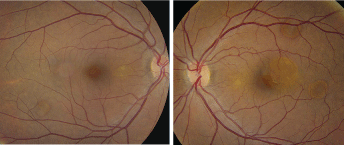
1, 2. Fundus images of our patient show unusual changes scattered throughout the posterior pole and the arcade (O.D. left, O.S. right). What do these changes represent?
On dilated fundus exam, the vitreous was clear O.U. He had small cups with good rim coloration and perfusion O.U. Examination of the macula O.D. was normal; however, some peculiar changes could be seen along the inferior arcade (figure 1).
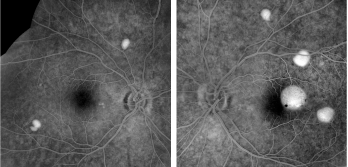 |
| 3, 4. The late-phase frames of our patients fluorescein angiogram (O.D. left, O.S. right) show some interesting changes. What are these changes consistent with? |
The fundus examination of the left eye showed a similar change adjacent to the macula and several other changes throughout the posterior pole and midperiphery (figure 2). Stratus optical coherence tomography (OCT) and fluorescein angiography (FA) were also performed (figures 3 to 6).
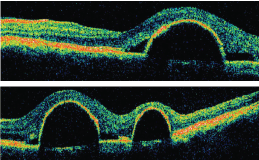
5, 6. A horizontal slice through the left macula (top) and an oblique section of the left macula on Stratus OCT.
Take the Retina Quiz
1. What do the retinal changes seen in both eyes represent?
a. Multiple serous retinal detachments.
b. Multiple pigment epithelial detachments (PEDs).
c. Localized choroidal neovascularization (CNV).
d. Polypoidal choroidal lesions.
2. What does the FA confirm?
a. Multiple serous retinal detachment.
b. PEDs.
c. CNV.
d. Polypoidal choroidal lesions.
3. What does the OCT in figure 5 show?
a. A PED involving the macula.
b. A serous detachment involving the macula.
c. A serous detachment involving the macula and an adjacent PED.
d. A PED secondary to CNV.
4. What is the most likely diagnosis?
a. Idiopathic retinal pigment epithelial detachments.
b. A variant of idiopathic central serous choroidopathy (ICSC).
c. Presumed ocular histoplasmosis.
d. Polypoidal choroidal vasculopathy.
5. How should this patient be managed?
a. Close observation.
b. Avastin (bevacizumab, Genentech) or Lucentis (ranibizumab, Genentech).
c. Photodynamic therapy (PDT).
d. Laser.
For answers, see below.
Discussion
Our patient has multiple serous retinal pigment epithelial detachments O.U., with one large detachment adjacent to his macula O.S. The PED in his left eye is actually outside the fovea. Because of its size, however, there is an overlying neurosensory detachment directly under his fovea that has resulted in some disruption of the photoreceptor segments. The small amount of fluid under his fovea is the likely cause of his reduced visual acuity in the left eye and his other symptoms.
Serous detachments of the retinal pigment epithelium (RPE) are characterized by sharply demarcated, dome-shaped elevations. They can resemble serous retinal detachments (similar to those seen in ICSC), but they tend not to be as sharply demarcated as PEDs.
Fluorescein angiography offers another way to distinguish between the two conditions. On FA, serous PEDs show early and persistent staining, whereas serous retinal detachments show a diffuse glow and never stain as dramatically as a PED. In our patient, there is obvious early and persistent staining on FA that not only highlights the PEDs, but also highlights about seven PEDs that could not be seen on clinical examination.
How do we explain this unusual bilateral presentation in an otherwise healthy individual? I am not sure that we can.
Multiple PEDs have been reported in a variety of patients, including pregnant women, individuals undergoing hemodialysis and individuals who use systemic corticosteroids for diseases, such as lupus or rheumatoid arthritis. Multiple serous PEDs can also be seen in patients with wet age-related macular degeneration (AMD) and polypoidal choroidal vasculopathy. However, our patient has none of these conditions and is seemingly in excellent health.
Based on fundus appearance and given these circumstances, the patient likely has an atypical form of ICSC. ICSC typically affects healthy patients between ages 20 and 45, and men are five to 10 times more likely to develop ICSC than women.1
The condition is usually associated with emotional stress and often presents in patients with Type A, achievement-oriented personalities.1 The disease is usually self-limiting, with an excellent visual prognosis.
Clinically, the hallmark of ICSC is a neurosensory retinal detachment that usually involves the macula.1 The neurosensory detachment typically develops as a result of a tiny PED that can only be seen on FA. In fact, the pinpoint leakage, which is commonly seen on FA, is the result of a microscopic PED.1
Although this is not exactly the clinical presentation of our patient, that still does not rule out ICSC. In 1978, Mary Lou Lewis, M.D., described 21 patients younger than age 55 with similar presentations to our patient.2 All her patients had idiopathic serous detachments of the RPE that were at least one-fifth disc diameter in size. She believed that this presentation was a variant of ICSC. Seventy-eight percent of her patients had visual acuity of 20/25 or better, and 97% demonstrated 20/50 or better in the affected eye.2 She concluded that these patients have an excellent visual prognosis.
The recommended treatment for typical ICSC is observation, as most patients spontaneously improve within six months. Given the good visual acuity of our patient, we elected to observe him with the hope that the fluid will reabsorb and the detachments will spontaneously flatten.
Retina Quiz Answers: 1) b; 2) b; 3) c; 4) b; 5) a
1. Gass JDM. Stereoscopic Atlas of Macular Disease: Diagnosis and Treatment, 4th ed.
2. Lewis ML. Idiopathic serous detachments of the retinal pigment epithelium. Arch Ophthalmol 1978 Apr;96(4):620-4.

