Q: I have a patient who I sent for cataract surgery and implantation of a toric intraocular lens. When the patient came back, his best-corrected visual acuity was 20/40 due to a misaligned lens. How can this be prevented in the future?
 |
A: Fortunately, the future is here. There are several newly available cataract surgery systems that will help the surgeon align the toric lens more accurately. Not many centers have these systems just yet—but they’re coming, so you should know what to expect.
Before discussing what these new surgery systems can do, let’s review the heart of the matter: the toric intraocular lens (IOL).
Toric IOLs have been a big hit since their introduction several years ago. First introduced in the 1990s, newer toric IOL designs include the AcrySof Toric (Alcon), approved by the FDA in 2005, as well as the Tecnis Toric (Abbott Medical Optics) and Trulign Crystalens Toric (Bausch + Lomb), both approved in 2013.
These implants allow for better management of corneal astigmatism, leading to less reliance on distance correction and a simpler reading prescription as well. Any patient with more than 1.00D of regular astigmatism is a candidate for a toric lens.
| |
|
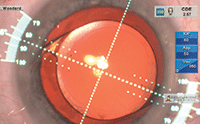
The reticule, as seen through a surgical microscope, helps to align the marks on the toric lens.
|
As the comanaging OD, you can play a huge role in counseling patients and obtaining measurements ahead of time. Be sure to obtain corneal topography on every patient before you send him or her for surgery. Also, insurance doesn’t cover the extra costs associated with this lens, so you’ll need to discuss the price as well as the advantage of correcting the refractive error more naturally inside the eye.
Once a patient chooses this lens, the measurements become critical. Even a minor error in alignment can result in a significant reduction in vision. This is where the new surgical systems shine. Surgical “suites”—such as the Cataract Refractive Suite using the new Verion Image Guided System (Alcon) and the Zeiss Cataract Suite—link the imaging/measurement device with the phaco machine and the operating microscope.
Specifically, the system’s imaging device measures the eye using biometric landmarks such as scleral vessels and iris crypts. Then, that information is transferred to the surgical microscope for precise axis alignment and positioning of the toric lens.
The Alcon system goes one step further by communicating this information to its LenSx femtosecond laser, allowing for more accurate placement of arcuate incisions (for astigmatism correction under 1.00D).
Q: So, how would such a system have avoided the misaligned toric IOL in my patient?
A: Without this technology, eyes are marked “by hand” based on the surgeon’s best estimate of where the axis of the astigmatism should be. “This technique has been less reliable and is very difficult to reproduce,” says Lawrence Woodard, MD, Medical Director of Omni Eye Services of Atlanta, one of the first practices in the nation to use one of these new surgical suites. “These integrated systems eliminate the need for manual marking, resulting in improved accuracy, reproducibility and visual outcomes,” Dr. Woodard says.
With the help of comanaging ODs who can track and share post-surgical refractive data, surgeons will further optimize post-op results with these systems by adjusting future A-scan calculations.
In addition to improved alignment of toric lenses, these instruments also allow for better centration of multifocal IOLs, giving patients their best chance of seeing clearly at all distances after surgery.

