Note: Given the time-sensitive nature of the topic, this article from the June 15, 2020 issue of Review of Optometry is being published online ahead of print, June 3, 2020.
As practices across the country are reopening for routine care amid COVID-19, the process isn’t business as usual. For instance, when patients enter optometrist Bradley Richlin’s practice in Beverly Hills, they are now greeted with a sign that reads, “Welcome to Our Sterile Office,” followed by a masked staff member who reinforces the message: “Welcome to our office. Things have changed for your safety and ours.”
With the addition of personal protective equipment (PPE), slit lamp breath shields and routine disinfection, ODs are going to great lengths to protect their patients, staff and themselves. Communicating these efforts can be paramount in allaying patient fears. “The number one question we get from patients is, ‘What are you doing to keep me safe?’” Dr. Richlin says.
In the 10th wave of Jobson’s weekly Coronavirus ECP Survey, a majority of respondents (52%) said patients were willing to reschedule appointments if they were comfortable with the safety precautions.
Still, patient education in the time of COVID-19 encompasses far more than simply touting new office cleaning protocols. Doctors also find themselves fielding questions on how to safely wear contact lenses and whether they can contract the virus through their eyes.
 |
| Dr. Whipple’s office has a screening area set up before patients even enter the office. Photo: Ian Whipple, OD. Click image to enlarge. |
It Starts With a Call
The initial scheduling call is the first opportunity to educate patients on the office changes. When patients call optometrist Glenn Corbin’s practice in Wyomissing, Pa., staff let them know everyone is required to wear a mask—something most patients appreciate, Dr. Corbin says.
Not only that, if patients take their mask off during the visit, staff ask them to either put their mask back on or leave.
During that initial phone call, staff also advise patients that they will take their temperature when they arrive, and the individual should plan to come alone. “We don’t want additional family members or others in the practice unless it’s medically appropriate or the additional person is a parent of a child,” Dr. Corbin says.
For Ian Whipple, OD, of Farr West, Utah, his staff reassure patients that they will be given a mask and gloves when they arrive. They also outline the new check-in protocols and extended appointment time to allow for cleaning.
In-office Precautions
Often, the best defense is a good offense, and many ODs are getting ahead of any concerns with extended patient intake forms. All of Dr. Whipple’s patients complete a risk assessment to determine if anyone in their household is ill; the form not only gathers information but also conveys to patients a strong message: the office isn’t taking any risks if patients feel ill. If they are, the individual is rescheduled.
Recently, two patients had to reschedule due to red flags, the latter being a teething infant. The child returned to the practice 10 days later with her father, and the mother joined the appointment via Skype since the practice only allows one individual to accompany a patient, when necessary. Dr. Whipple says both parents were appreciative that his practice took precautionary methods to keep their family safe.
If a patient enters Dr. Richlin’s practice already wearing gloves, staff ask the individual to remove them. “Some patients think the gloves are protecting them, but we let them know their gloves are dirty, and gloves are just like your hands, but you don’t wash your gloves.”
Patients are instructed to clean their hands with the touchless hand sanitizer and don a clean surgical mask (even if they are already wearing a cloth mask). Staff then take their temperature with a no-touch thermometer and place a bright neon sticker on their shoulder, indicating they’ve passed the checkpoint.
During the visit, staff educate patients on the rigorous precautions the office is taking to ensure everyone’s safety. When staff arrive at work, everyone is required to log in and record their temperatures and any symptoms. Anything suspicions prompts a pop-up alert instructing them to go home and contact their primary care physician.
Sanitation Products AboundMost optometric practices have set strict cleaning protocols upon reopening for routine care. In addition to wiping down surfaces between patients, some ODs are adding extra steps in an effort to sanitize and better reassure patients: • COVID-19 disinfectants: While many household cleaning products claim to kill COVID-19, the EPA offers a list of approved disinfectants: www.epa.gov/pesticide-registration/list-n-disinfectants-use-against-sars-cov-2. On this list is hypochlorous acid, which is often used to manage a number of ocular conditions. Dr. Whipple now uses hypochlorous acid to disinfect surfaces in his practice and explains its benefits to patients when they enter the exam room. He chose this cleaning product in particular because it is gentle enough that he doesn’t need to glove up as is often the case with harsher products, he adds. • Electrostatic disinfection: Dr. Corbin recently committed to an electrostatic system for disinfecting his practice. The new misting sprayer, eMist from Eye Designs, is said by its manufacturer to adhere to surfaces more readily because electrostatic attraction allows it to coat a larger surface area than spray-and-wipe techniques that may leave large areas untouched. For some, this could mean a faster, more efficient sterilization process for frames, equipment, chairs and doors. The active ingredient here is also hypochlorous acid. • Air purifiers with HEPA filters: Dr. Richlin purchased three medical-grade HEPA air filters for his practice. Each has a charcoal filter for smell and uses UV light to kill viruses, mold, fungi and bacteria. On top of each air filter he added signs reading, “Hi. Don’t mind me. I’m an air filter, I’m here to clean your air, kill viruses and bacteria and keep you safe.” • UV boxes to sanitize frames: Ultraviolet LED sterilizer boxes are designed to clean objects during a quick two-to-three minute light cycle. Most are easy to use with just a push of a button. Reseach shows UV sanitizing makes viruses non-viable, and as such, hospitals routinely use this technology, Dr. Richlin says. In Dr. Richlin’s dispensary, used frames get a double cleaning, first with soap and water followed by a turn in a UV box. • Touch-free hand sanitizers: Upon reopening, Dr. Richlin added 15 touchless hand sanitizers throughout the office, which he says are meant to eliminate a common contact point where germs can be transferred—a traditional sanitizer bottle’s pump. |
Exam Lane Changes
The eye exam requires the doctor to work in close proximity to the patient, less than the six-foot guidance—perhaps not as close as a dental hygienist or dentist, but close nonetheless, and especially with contact lens services, says Brian Chou, OD, who practices in San Diego. “I believe that the close nature of examinations is implicit for patients that have previously had an eye exam,” he says.
Still patients should expect increased disinfection, more hand washing and the use of masks and gloves. When entering the exam room, patients’ worries may be eased just by seeing disinfection taking place before they sit in the chair.
Dr. Richlin’s staff cleans every surface before and after each patient. Because patients want to see the room cleaned in front of them, staff will clean the arm rests, microscope, eye drop bottles and other surfaces in their presence, he adds.
“Aside from conspicuous and regular hand washing, I’m not doing much different compared to before COVID-19 with instilling eye drops, contact lens application and expressing meibomian glands,” says Dr. Chou. “With instilling topical anesthetic and dilating drops, as before, I take care not to contact the bottle tip with the patient’s ocular tissue.”
But some ODs have implemented changes for each of these instances:
Eye drops. Dr. Whipple’s practice is trying to eliminate eye drops as much as possible and is encouraging ultra-widefield imaging as an alternative to dilation whenever possible.
Contact lenses. While Dr. Whipple now wears gloves during contact lens insertion and removal, ODs at Dr. Richlin’s practice are still doing contact lens appointments with clean hands that are washed again immediately after the process is complete.
With contact lens application, and particularly with new wearers, Dr. Chou generally takes charge of the lens handling in the exam room, since he says he is usually faster, more hygienic and less prone to time-consuming complications.
Gland expression. For meibomian gland expression, Dr. Richlin now relies heavily on the LipiFlow (Johnson & Johnson Vision) and wears gloves during the procedure.
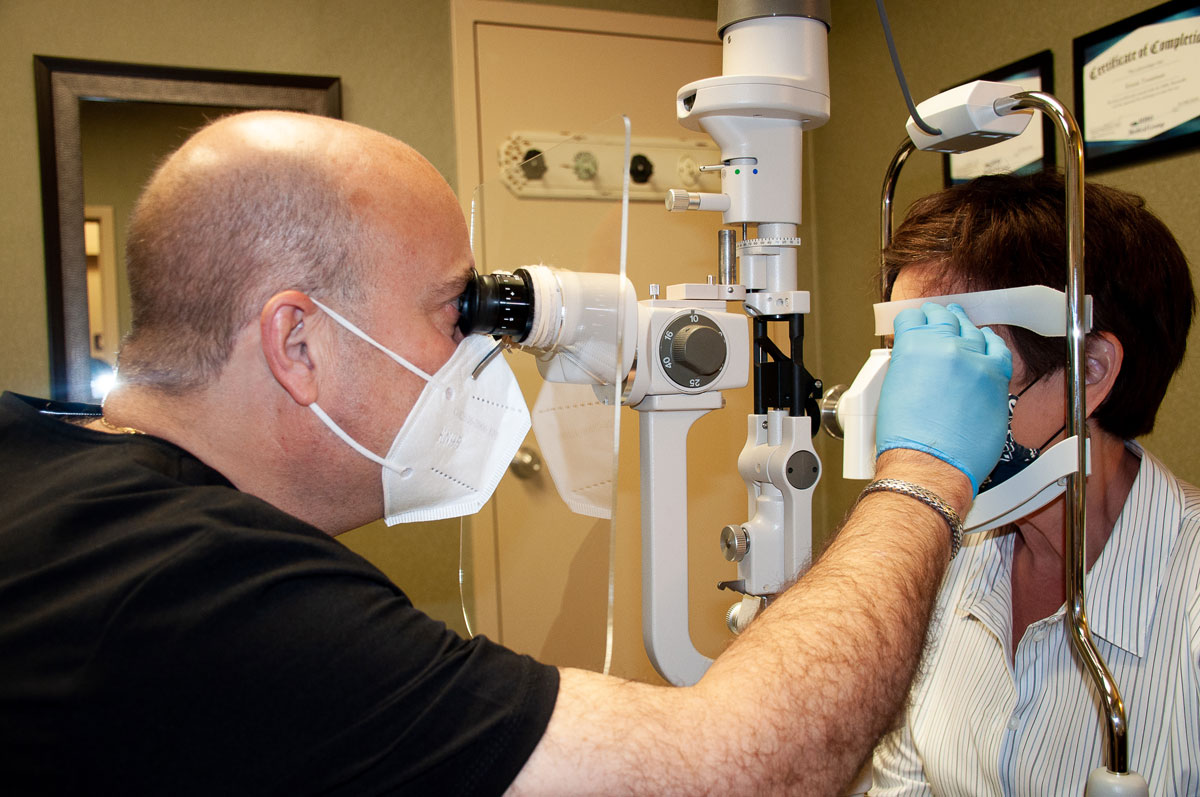 |
| Dr. Corbin and his patients wear masks and gloves throughout the exam. Photo: Glenn Corbin, OD. Click image to enlarge. |
Allay CL Fears
While many people are hungry for information regarding how to stay safe during the pandemic, misinformation is rampant about contact lens wear, according to the Centre for Ocular Research and Education (CORE).1 Despite the myths and misinformation, contact lens wear remains safe—something clinicians need to stress to their patients who may be uncertain.1
Optometrists can reassure patients that no scientific evidence suggests lens wear increases their risk of contracting COVID-19 compared with spectacle wear.2,3
In addition, good hygiene, and specifically hand washing, is widely accepted as a critical preventative measure against COVID-19. For contact lens wearers, hand washing has always been important, but more so now than ever. Clinicians must re-educate contact lens wearers on the need for thorough hand washing and drying before inserting and removing lenses and proper lens wear and care, including replacing contact lens cases regularly.2,3 Spectacle wearers should regularly clean their glasses with soap and water.2,3 CORE also offer these additional pearls:2,3
- Regular eyeglasses don’t provide protection from COVID-19.
- Keep unwashed hands away from your face.
- If you become sick, temporarily stop wearing your lenses and switch to glasses.2,3
Still, conflicting reports that suggest patients shouldn’t wear contact lenses during the pandemic may be influencing patients’ lens wearing habits.4 An early April poll of 89 patients on lockdown found 72% were wearing their lenses less than normal. The most common reason was “less need” for contact lenses while at home. Another reason for reduced contact lens wear during the lockdown included concern about infection due to lens use (8%).4
Dr. Richlin reminds his patients that if they keep their fingertips clean—as they should rgardless of COVID-19—they shouldn’t have any issues, as contact lenses are rarely the source of infection; rather, unclean cases, dirty fingers and dirty eyelids are often the culprits.
ODs Do Double-Duty as Mask EnforcersMasks have become a flashpoint in some areas of the country during the pandemic. Upon reopening, many doctors have enforced strict mask policies. According to Jobson’s 10th wave Coronavirus ECP Survey, 64% of clinicians are offering free masks and 14% are providing one for a fee. Another 13% are barring unmasked patients from entering the practice, while only 3% are willing to see them without a mask. If a patient is uncomfortable wearing a mask in Dr. Corbin’s practice, the individual is rescheduled in one to two months when the requirement may be lifted. “My attitude is, if you don’t want to wear a mask, you won’t have access to my practice. I’m not going to put my patients, my staff and myself at elevated risk because someone doesn’t want to wear a mask,” Dr. Corbin says. In the first week of his practice’s reopening, Dr. Whipple had to turn away a patient for refusing to wear a mask and gloves. “It wasn’t worth the risk to our employees,” he says. “I was really proud of my staff members for sticking to their guns.” Some patients may come armed with a letter outlining their rights to not wear a mask based on the Americans with Disabilities Act (ADA)—a sticky situation for ODs trying to keep everyone safe. Recently, the Department of Justice released a warning that it has not issued any formal letter, so any patient claiming to have one may not realize it’s not official.1 In addition, the ADA does allow medical offices to refuse care if the patient “poses a direct threat to the health or safety of others.”2
|
No-touch Dispensing
The dispensary, perhaps more so than the waiting area or exam room, is likely to be a patient’s biggest source of anxiety in a newly reopened practice. It’s also a concern for practitioners, as 46% of Jobson’s Coronavirus ECP Survey respondents are looking for information on how to handle patients and frame selection in the optical/dispensary.
Long gone are the days when patients can browse freely and take various frames from the board for a test drive. This is sure to cause both relief and frustration. Everyone wants to feel insulated from exposure, but the “customer first” environment of the dispensary may compel patients to still do as they please. Plan to invest time reorienting patients to a new experience.
Dr. Whipple’s practice launched a mandatory guided frame selection process following reopening. His opticians were already well-trained to offer patients frame recommendations; now, staff stay by the patient’s side in the dispensary, make suggestions, take the frames from the board and immediately place the unwanted frames in a separate bin for disinfection—a process Dr. Richlin’s practice is following as well.
Dr. Richlin added an extra ultraviolet (UV) light sanitation step for already cleaned frames.
Limited Bathroom Access
These days, you can never be too careful about safety, and now that means stricter bathroom protocols as well. Dr. Whipple only opens the office bathroom upon request. “It might be a bit overboard, but we weren’t sure if people were using it, so we decided to lock the door and if someone does need it, we give them the key and know to wipe it down afterward.”
 |
 |
| In many offices, the COVID-19 optical experience looks a lot different now, with masks, face shields, a personalized frame selection process and sanitizing between patients. Photo: Glenn Corbin, OD. Click images to enlarge. |
COVID-19 and the Eye
Researchers are working overtime to better understand this novel coronavirus, yet much remains uncertain. Patients are bound to ask if COVID-19 can manifest in the eye, and even well-read doctors will likely say the answer isn’t clear.
However, some preliminary investigations can help clinicians educate patients on the current understanding. Some studies suggest the virus is capable of causing ocular complications such as viral conjunctivitis in the middle phase of illness.5
One case study highlights a patient diagnosed with viral conjunctivitis two days before classic symptoms of COVID-19 presented.6
A recent non–peer reviewed investigation from Johns Hopkins University suggests the ocular surface is susceptible to infection and could serve as a portal of entry through exposure to aerosolized droplets or hand-eye contact.7
Still, a comprehensive review as of April 15 noted that coronaviruses are unlikely to bind to ocular surface cells to initiate infection. The review also found only occasional cases of conjunctivitis reported in patients with COVID-19.9
Dr. Whipple admits everything he’s doing at his practice might not be a one-size-fits all for other doctors. “I feel every small thing we do hopefully shows patients we really do care about keeping them safe and we’re taking this seriously. Hopefully, it’s giving patients a little more trust in what we do.”
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
1. Centre for Ocular Research and Education (CORE). COVID-19 and contact lens wear: what do eye care practitioners and patients need to know? Contact Lens Update. March 16, 2020. 2. Jones L, Walsh K, Wilcox M, et al. The COVID-19 pandemic: Important considerations for contact lens practitioners. Cont Lens Ant Eye. 2020;43(3):196-203. 3. CORE. COVID-19 and contact lenses: the facts you need to know, new research reassures & advises contact lens wearers during coronavirus/COVID-19 pandemic, offers clear facts and hygiene advice. core.uwaterloo.ca/covid-19. Accessed May 25, 2020. 4. Morgan PB. Contact lens wear during the COVID-19 pandemic. Cont Lens Ant Eye. 2020;43(3):213. 5. Chen L, Meizhou L, Zhang Z, et al. Ocular manifestations of a hospitalized patient with confirmed 2019 novel coronavirus disease. Br J Ophthalmol. 2020;43(3):213. 6. Khavandi S, Tabibzadeh E, Naderan M, et al. Corona virus disease-19 (COVID-19) presenting as conjunctivitis: atypically high-risk during a pandemic. Cont Lens Ant Eye. 2020;43(3):213. 7. Zhou L, Xu Z, Castiglione GM, et al. ACE2 and TMPRSS2 are expressed on the human ocular surface, suggesting susceptibility to SARS-CoV-2 infection. bioRxiv. May 9, 2020. [Epub ahead of print]. 8. Wu P, Duan F, Luo C, et al. Characteristics of ocular findings of patients with coronavirus disease 2019 (COVID-19) in Hubei Province, China. JAMA Ophthalmol. 2020;138(5):575-78. 9. Willcox MDP, Walsh K, Nichols JJ, et al. The ocular surface, coronaviruses and COVID-19. Clin Exp Optom. May 13, 2020. [Epub ahead of print]. |

