 |
A 63-year-old Caucasian female presented to the office as a new patient in June seeking a second opinion. She had presented to an eye clinic earlier in the year with complaints of gradually decreasing vision. The patient attributed this to normal decline in her vision, and felt that her eyeglasses needed to be updated. She was told that she did have a change in her prescription and that new glasses were warranted, but also that she needed to see a glaucoma specialist for a “laser procedure.”
She ordered new eyeglasses, and shortly thereafter she made her way to an ophthalmic surgeon who performed a laser procedure on both eyes that same day. Approximately two weeks after the procedure, she developed moderate pain, with photophobia and a headache lasting a couple of days as well as difficulty seeing out of the left eye. She subsequently reported back to the surgeon who performed the laser procedure, and was put on drops (the patient did not know which ones specifically, but she remembered she was to shake the drops vigorously before instillation) for what was about five days, during which time the pain seemed to resolve, but her vision remained blurry. She reported back to the surgeon who then referred her to retina.
Apparently when seen at retina, blood work was ordered and the patient was told that she may have had a “stroke” in the eye. In a subsequent follow-up with retina, the patient was told the blood work was normal and the residual effects on vision to her left eye are permanent. She was then sent to my office.
Examination
When seen by me for the first time, she was only taking lisinopril, and had been so for several years, and she was taking no topical medications. Her best-corrected visual acuities were 20/20-1 OD and 20/50 OS. Her pupils were round and reactive to light, and there was a 2+ afferent pupillary defect in her left eye. Confrontation fields demonstrated an altitudinal defect in the left eye and were normal in the right.
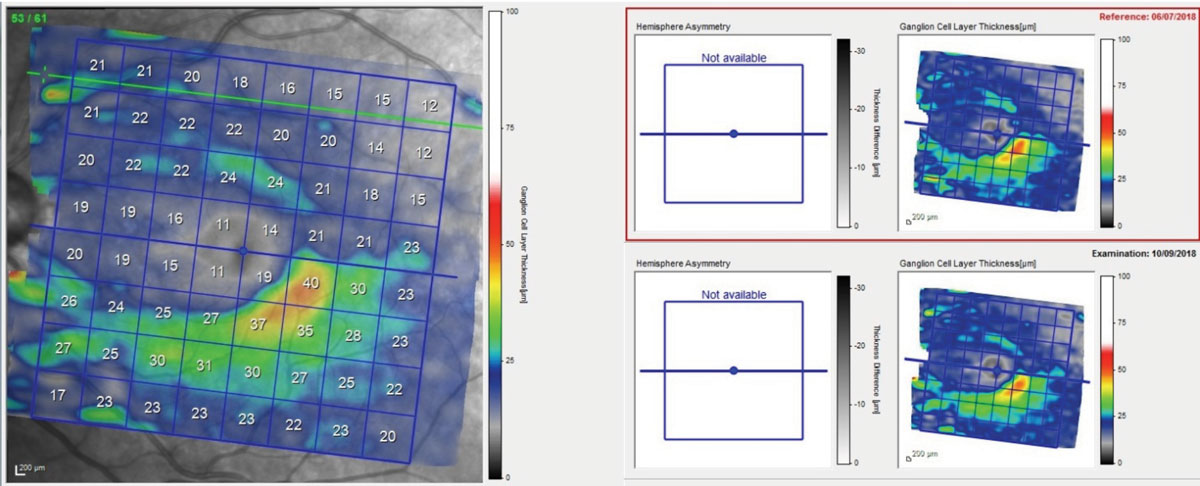 |
| This OCT shows our patient’s left macula, highlighting the ganglion cells. Note the significant loss of ganglion cells superiorly as compared with inferiorly, and the lack of change seen as compared with the baseline. This is consistent with chronic phase ganglion cell loss, as opposed to acute loss. |
A slit lamp examination of her corneas was unremarkable. Both anterior chamber angles appeared somewhat narrow at the slit lamp using the Van Herick technique. Her right eye had a laser peripheral iridotomy (LPI) at 12 o’clock, and in the left there were two LPIs, one at 3 o’clock and the other at 9 o’clock. Her anterior chambers were quiet with no cells or flare. Applanation tensions at 3:45pm were 23mm Hg OD and 24mm Hg OS. Pachymetry readings were 598µm OD and 594µm OS.
Threshold visual fields were entirely normal in the right eye. The left was characterized by a field defect extending from the blind spot to fixation, greater below the horizontal than above. The findings were consistent with an optic nerve infarct and with the confrontation field findings.
The patient was dilated in the usual fashion. Through dilated pupils, her crystalline lenses were characterized by mild nuclear sclerosis in both eyes.
The cup-to-disc ratio in her right eye was 0.3x0.3 and that of the left was 0.4x0.4. The neuroretinal rim in the right was plush and well perfused, whereas that of the left was pale and atrophic from 12 o’clock to 4 o’clock. Both maculae were healthy. Her retinal vascular details were also unremarkable. The peripheral retina was characterized by scattered areas of cystoids degeneration in both eyes. Post dilation pressures were 22mm Hg OD and OS, with open angles.
OCT imaging of the optic nerves was consistent with a chronic appearance of non-arteritic ischemic optic neuropathy (NAION) in the left eye; the OCT imaging of the right optic nerve was unremarkable. Neuro OCT imaging of the left optic nerve demonstrated a reduced papillomacular bundle, consistent with the findings of NAION.
History
Much of the history on the initial visit was from the patient’s perspective, and I’ve learned over the years that, sometimes what actually happens is different than what is portrayed in the history. Subsequent to our first visit together, I was able to obtain relevant medical records, and the patient’s interpretation of the series of events was fairly accurate.
One of my initial questions at the first visit centered around what transpired during the laser procedure. It was my interpretation from the history, and later confirmed by review of the medical records, that the patient was only given two drops in each eye of Iopidine (apraclonidine, Novartis) in the office, and was discharged on a regimen of Pred Forte (prednisolone acetate, Allergan) to use for three days. No follow-up was scheduled.
On the follow-up visit after the patient experienced pain and blurred vision, she was again prescribed Pred Forte QID and was scheduled to see a retina specialist. There was no mention of the status of the anterior chamber at that visit, and IOPs were 20mm Hg OD and OS.
Diagnosis
The retinologist diagnosed an ischemic optic neuropathy and the patient was ultimately sent to me. As best as I can tell, sometime following the LPI, most likely within the first few days, the left optic nerve infarcted. Did the LPI contribute to that? Possibly, though we’ll never know for certain. But the timeframe fits. Could she have experienced an exaggerated inflammatory response in the left eye that underwent two LPI procedures? Could she have had a concurrent IOP spike post LPI in the left eye? What did that eye look like in the immediate post LPI period? The answers to these questions are unknown, as no follow-up was performed until after the patient developed symptoms.
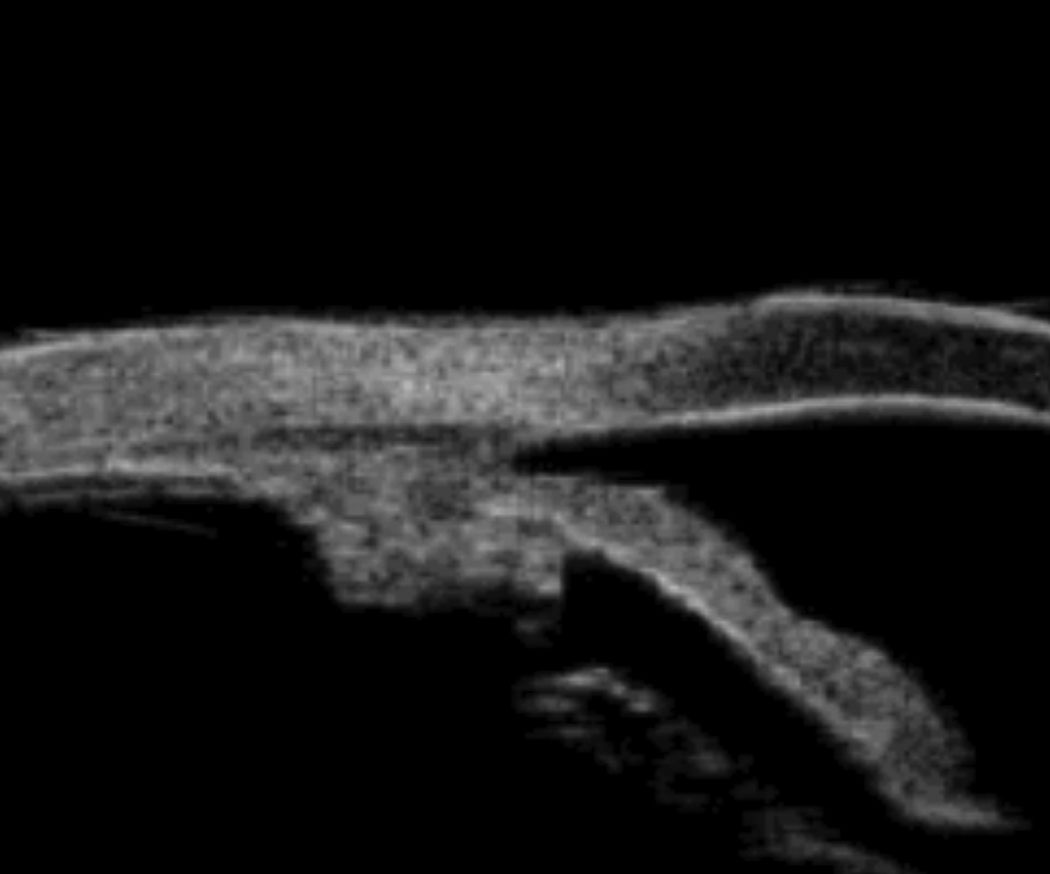 |
| Note the relative anterior positioning of the ciliary body posterior to the iris root, and the subsequent anterior displacement of the iris root. This can be seen on slit lamp as a narrow angle, but without the ciliary body being visible on slit lamp exam, the diagnosis of plateau iris configuration cannot be made. |
This is an important reminder that, following LPI, the patient must be examined several days later for some of the common side effects from the procedure, such as inflammation and IOP elevation, not to mention what effect it has on opening the angles and reducing the risk of angle closure. And therein lies the rub in this unfortunate situation.
Imaging
Standard protocol in my office when I am examining patients with narrow or slightly narrow angles is to obtain an ultrasound biomicroscopy (UBM) image of the anterior segment. While the angle itself can be visualized in a variety of ways, namely, at the slit lamp, during gonioscopy, and with anterior segment OCT imaging, there are times when UBM gives us important details. And one of the situations where UBM gives us more data than the aforementioned procedures is in the case of plateau iris configuration.
In plateau iris configuration, the ciliary body and ciliary processes are positioned more anteriorly, and therefore result in the iris being positioned more anteriorly, especially toward the iris root. The iris may appear non-bowed on clinical examination. The mechanism of angle closure in plateau iris syndrome is different than in normal anatomically narrow angles, where typically pupillary block results in elevation of IOP in the posterior chamber, which in turn forces the iris root more anteriorly.
The benefit of LPI in cases of narrow angles and pupillary block glaucoma is well documented. However, LPIs have little effect in reducing the potential closure of the angle in cases of plateau iris configuration.
Plateau iris syndrome is essentially a form of angle closure glaucoma, but with a mechanism different than outlined above, and with the appearance of narrow angle glaucoma.1 UBM plays an important role in differentiating anatomically narrow angles from plateau iris configuration.2,3
Treatment
Because a plateau iris configuration lends itself to a different mechanism of subsequent angle closure, the treatment options are different. The treatment of choice in plateau iris situations is a laser iridoplasty.1 In argon laser peripheral iridoplasty, laser energy is applied to the peripheral iris in a circumferential pattern. The thermal energy applied to the iris causes contracture of the iris, and a somewhat posterior planar movement of the peripheral iris away from the cornea and trabecular meshwork.
Researchers suggest that, when an LPI is performed and there is no opening of the anterior chamber angle, plateau iris configuration be considered.1 And that is exactly what happened in this case; post LPI, the angle configuration had not changed. Of course hindsight is always 20/20, but pre-surgical evaluation with UBM can facilitate the diagnosis before intervention is performed.
What is doubly unfortunate in this case is that the ophthalmic surgeon who performed the LPI does not have a UBM unit. We do, and the surgeon knows that we do. How many times has that surgeon sent a patient to this OD for that procedure? Precisely zero. One of the other things I’ve learned throughout the years is that some ophthalmic surgeons give lip service to working with optometry, when in fact their actions sometimes speak louder than words. Someone is still fighting the old battles between the professions. And unfortunately, it is the patient who invariably loses.
|
1. Stefan C, Iliescu D, Batras M, et al. Plateau iris – diagnosis and treatment. Rom J Ophthalmol. 2015;59(1):14-8. 2. Kumar G, Bali S, Panda A, et al. Prevalence of plateau iris configuration in primary angle closure glaucoma using ultrasound biomicroscopy in the Indian population. Indian J Ophthalmol. 2012;60(3):175-8. 3. Parc C, Laloum J, Berges O. Comparison of optical coherence tomography and ultrasound biomicroscopy for detection of plateau iris. J Fr Ophthalmol. 2010;33(4):266;e1-3. |

