 |
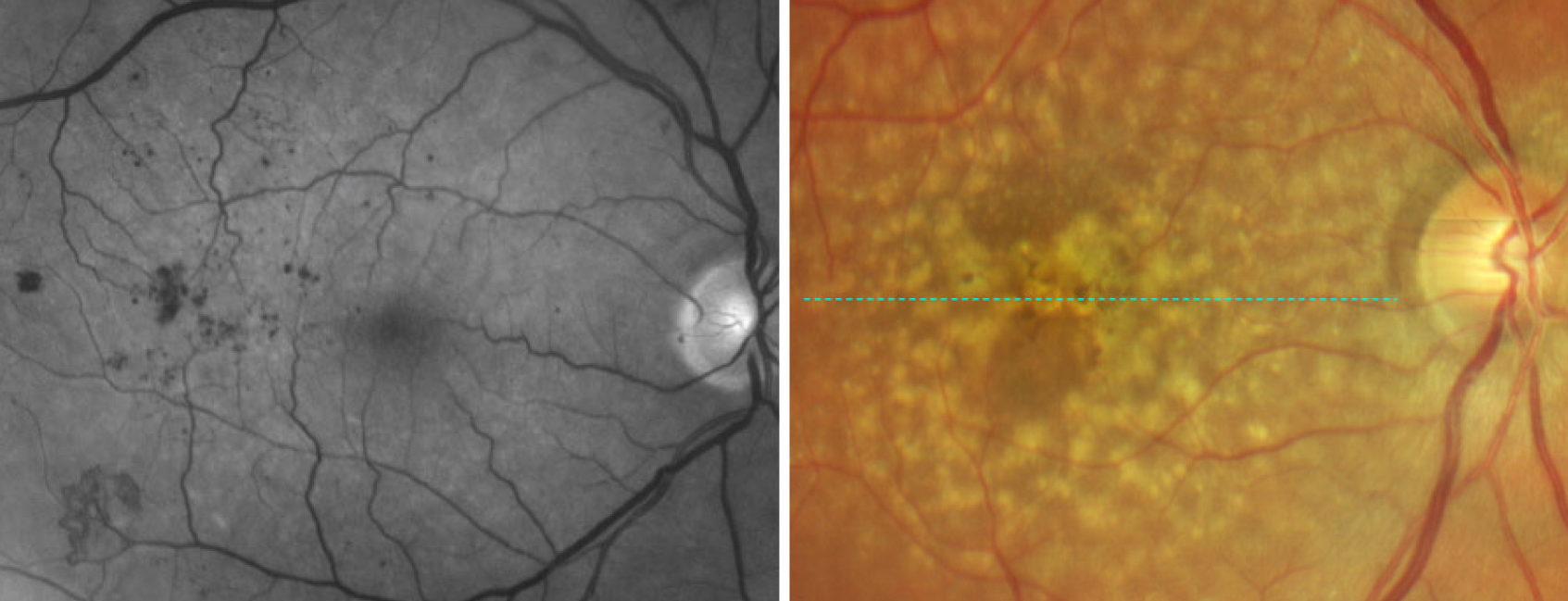
Milder DR at baseline was associated with increased risk of AMD. Photo: Steve Ferrucci, OD; Carolyn Majcher, OD. Click image to enlarge. |
You’ll sometimes hear lecturers at medical conferences remind the doctors in attendance that patients can have as many diseases as they like. This cheeky comment underscores the principle that not all signs and symptoms can or should be chalked up to a single condition; comorbidities are quite common and need to be teased apart. But for the two most common retinal conditions—AMD and DR—the presence of one argues against the likelihood of the other, at least in its most severe forms.
Researchers based in Boston have noted differing metabolic pathways underlying the development of both diseases. The team also demonstrated an inverse correlation of the clinical and biochemical changes between AMD and DR. Their results were presented on the first day of ARVO 2023 in New Orleans.
The study graded digital fundus images for ETDRS DR severity and for AMD using the AREDS system in people with types 1 and 2 diabetes at the Beetham Eye Institute, as well as those who have had insulin-dependent diabetes for 50 years or longer (Joslin 50-Year Medalist Study). Individual retinal layer thicknesses in the foveal area were assessed in eyes of this second group, which the study noted as the Medalist (n=545). Retinol binding protein 3 (RBP3) and VEGF concentrations were measured vitreous samples (n=187) obtained during vitreoretinal surgery of those in the eye institute group and from postmortem eyes of the Medalists.
The presence of AMD was associated with less severe DR in both Medalist (n=1163) and Beetham Eye Institute cohorts (n=580). In the Medalists, 16.2% had any AMD, 13.2% had AREDS levels 1 to 2 and 3.0% had AREDS levels 3 to 4. There were no eyes with neovascular AMD in the study.
All eyes with AMD in the eye institute cohort had AREDS levels 1 to 2 (10.4%). In the Medalist cohort, the presence and severity of AMD was positively associated with the presence of drusen outside the macula. The presence of drusen outside the macula was associated with less severe DR in the Medalists. In a subset of Medalists (22.9%) with longitudinal follow-up, DR progression was less frequent in eyes with AMD AREDS level ≥2 (n=2) compared with eyes with AMD AREDS level <2 (n=31, 13.0% vs 7.1%). Also, milder DR at baseline was associated with increased risk of AMD. Increased photoreceptor thickness was associated with AMD and milder DR. The presence of AMD and milder DR were associated with higher RBP3 to VEGF ratios in the vitreous from individuals of the Joslin Beetham Eye Institute and the Medalists.
“Detailed retinal studies from eyes with DR and AMD may provide additional pathways to target against these common sight-threatening diseases,” the researchers concluded in their abstract.
Original abstract content © Association for Research in Vision and Ophthalmology 2023.
Fickweiler W, Jacoba CMP, Jangolla S, et al. Inverse risk for progression of diabetic retinopathy and age-related macular degeneration. ARVO 2023 annual meeting. |

