 History
History
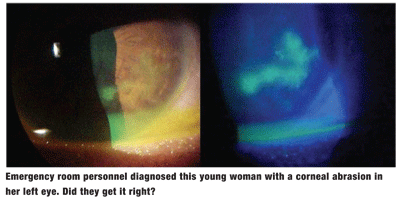
A 23-year-old white female presented with a painful red left eye. Four days earlier, she had gone to the emergency room, where she was diagnosed with a corneal abrasion. The ER staff medicated her with a topical antibiotic and instructed her to follow up with her own eye doctor. Her systemic history was noncontributory.
Diagnostic Data
The patients best-corrected acuity at this exam was 20/20 O.D. and 20/40 O.S. at distance and near. External examination was normal, and there was no evidence of afferent pupillary defect. The pertinent anterior segment findings are demonstrated in the photograph. Intraocular pressure measured 19mm Hg in both eyes. The dilated fundus findings were normal, O.U.
Your Diagnosis
How would you approach this case? Does this patient require additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Discussion
The diagnosis in this case is herpes simplex virus (HSV). Additional history for cold, upper respiratory infection, previous eye infection or fever blister might have been helpful. Additional testing might have included corneal sensitivity testing or corneal staining with fluorescein, lissamine green or rose bengal.
The herpes simplex virus, a member of the Herpesviridae family, is an obligate intracellular parasite.1-6 Humans are the only natural host of the virus. Although HSV contains the genetic material necessary to replicate, it does not have the metabolic machinery, so HSV enters the host cell and uses its metabolic pathways.1-6
There are two types of herpes simplex virus: herpes simplex virus 1 (HSV-1), which characteristically produces oral, facial and ocular lesions; and herpes simplex virus 2 (HSV-2), which is associated with the sexually-transmitted form of the disease.1-6
Transmission of HSV-1 occurs either from direct contact or via contaminated secretions.6 A positive titer of serum-neutralizing antibodies is often noted seven days following the primary infection. The titer then diminishes but remains positive throughout life. An infected person becomes the carrier of the disease, presumably by transneuronal spread of the virus into the neural ganglia. The virus then persists in a quiescent state called latency. Virus particles can be shed intermittently in tears, saliva, and respiratory and genital secretions.1,6 Occasionally, primary HSV-1 is ocular (as in this patients case), causing lid vesicles, ulcerative blepharitis, keratitis and conjunctivitis.
Management of purely epithelial herpes simplex keratitis involves debridement or use of the topical antiviral agent Viroptic (trifluridine, Monarch), or a combination of the two. Some manage the condition with oral antiviral medication such as acyclovir, famcyclovir or valacyclovir, but the topical treatment is regarded as the standard.
The management of stromal and disciform keratitis is more complex and usually involves both antiviral and anti-inflammatory measures.3-7 Oral antiviral agents can be used to prevent recurrence.3-7 Also, cyloplegia can be added to relieve discomfort.
The Herpes Stromal Keratitis, Not on Steroid Trial (HEDSSKN), found that patients who received prednisolone phosphate drops along with topical trifluridine had faster resolution of the stromal keratitis and fewer treatment failures than patients in the placebo group. The study also determined that delaying the initiation of corticosteroid treatment caused no deleterious effects.2-7
HEDS-SKN is one of three study arms of the Herpetic Eye Disease Study (HEDS) I. Another study arm, the Herpes Stromal Keratitis, on Steroid Treatment (HEDSSKS) demonstrated that adding oral acyclovir to the treatment regimen of a topical corticosteroid and a topical antiviral showed no apparent benefit when treating herpetic stromal keratitis.3-7 That said, other arms of HEDS indicate there are indications for oral therapy in combination with the topical or low-dose oral treatment following resolution of the episode.1-6
1. Kaye S, Choudhary A. Herpes simplex keratitis. Prog Retin Eye Res 2006 Jul;25(4):355-80.
2. Santos C. Herpes simplex uveitis. Bol Asoc Med P R 2004;96(2):71-4, 77-83.
3. Wilhelmus KR, Gee L, Hauck WW. Herpetic Eye Disease Study: A controlled trial of topical corticosteroids for herpes simplex stromal keratitis. Ophthalmology 1994 Dec;101(12):1883-96.
4.
5.
6. Gurwood AS. The National Eye Institute of The National Institutes of Health: Its history and impact on clinical eye care. Optometry 2003;74(10):627-57.
7. Wilhelmus KR. Interventions for herpes simplex virus epithelial keratitis. Cochrane Database Syst Rev 2003;(3):CD002898.

