Breast cancer is the leading cause of cancer death among women worldwide. It occurs in both men and women, although male breast cancer is rare. The American Cancer Society estimated nearly 1.4 million new cases of invasive breast cancer worldwide in 2008. In the United States, an estimated 207,090 women will be diagnosed with breast cancer and 39,840 women will die of it in 2010.1

Breast cancer is defined as a neoplasia that forms in tissues of the breast, usually the ducts and lobules (milk-producing glands). Malignant cancers of the breast arise through a series of molecular alterations at the cellular level, resulting in the uncontrolled outgrowth and spread of epithelial cells. (For more on tumorigenesis, see “
Neoplastic Disease: Part 1,” September 2010.)
Breast cancer research has led to marked progress in the understanding of the disease, resulting in more effective and less toxic treatments. Also, increased public awareness and improved screening have led to earlier diagnosis at stages more amenable to complete surgical resection and curative therapies.
Breast Cancer Risk Factors
Epidemiological studies have identified several factors that increase the chance of a woman developing breast cancer. Risk factors are identified based on their effect on the level and duration of exposure to endogenous estrogen.
• Age. The median age of diagnosis for breast cancer is about 61.2 The chance of getting breast cancer increases with advancing age.
Metastatic Carcinoma in the Eye
A 63-year-old white female presented with diplopia and proptosis O.S. Forced ductions revealed restrictive eye disease.
Below, the proptotic O.S. underacts in right gaze.
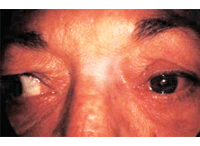
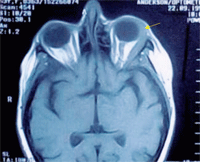
MRI revealed a soft tissue mass in the region of the left lacrimal gland. Orbital biopsy revealed malignant neoplasm consistent with metastatic carcinoma from the breast to the lacrimal gland.
• Personal health history. Having cancer in one breast increases the risk of cancer in the other breast. Certain types of abnormal cells (atypical hyperplasia, lobular carcinoma in situ [LCIS], or ductal carcinoma in situ [DCIS]) increase the risk of invasive breast cancer.2
• Family health history. Risk is increased if a first-degree relative has breast cancer. The risk is even higher if the family member had breast cancer before age 50.2
• Genetic factors. Mutations in certain genes, such as BRCA1 or BRCA2, substantially increase the risk. Women who inherit a mutation in the BRCA1 or BRCA2 gene have an estimated 50% to 80% lifetime risk of developing breast cancer.2
BRCA1 mutations are seen in 7% of families with multiple breast cancers and 40% of families with breast and ovarian cancer. People with a BRCA1 mutation have a lifetime risk of 40% for developing ovarian cancer and are also at a higher risk of colon cancer and prostate cancer.
• Radiation therapy to the chest. Women who have had radiation therapy to the chest (including the breasts) before age 30 are at an increased risk. This includes radiation for Hodgkin’s lymphoma. Studies show that the younger a woman is when she receives radiation treatment, the higher her risk of breast cancer later in life.2
• Reproductive and menstrual history. Women who never had children are at an increased risk. The older a woman is when she has her first child, the greater the chance of breast cancer. Women who had their first menstrual period before age 12 are at an increased risk. Those who went through menopause after age 55 are at an increased risk of breast cancer.
• Race. In the United States, breast cancer is diagnosed more often in white women than in African-American/black, Hispanic/Latina, Asian/Pacific Islander, or American Indian/Alaska Native women.2
• Breast density. Mammography studies show the breast as having areas of dense tissue and areas of fatty tissue. Women whose mammogram shows a larger than normal area of dense tissue (compared to others in their age group) are at increased risk of breast cancer.2
• Hormone replacement therapy (HRT). Consistent epidemiologic data support an increased risk of breast cancer incidence and mortality with the use of postmenopausal HRT. Risk is directly associated with length of exposure.2
• Excess weight. The chance of getting breast cancer after menopause is higher in women who are overweight or obese. In addition, women who are physically inactive throughout life may have an increased risk of breast cancer.2
• Alcohol. Studies suggest that the more alcohol a woman drinks, the greater her risk of breast cancer.2
Breast Cancer and the Eye
Intraocular/orbital metastasis is the most common malignancy of the eye, but often goes undiagnosed.4 The frequency of intraocular metastasis in patients dying of cancer is approximately 12%. Breast carcinoma in women and lung carcinoma in men are the most common primary foci.4
The uveal tract, with its rich vascular network, is the site in the globe most often involved in metastatic disease. Less commonly, other ophthalmic structures—including the optic nerve, conjunctiva and lacrimal gland—are the sites of metastatic cancer. The overall survival time (eight to 12 months on average) for these patients is poor.4-6
Treatment and Management

Management of intraocular/orbital metastasis may include observation, chemotherapy, photocoagulation, cryosurgery, surgical resection, localized plaque therapy, and external beam radiation.4,6 The specific therapy chosen is an individualized process that must take into account the clinical condition of the patient.
The choice of cancer therapy for the primary site depends upon the location and grade of the tumor(s), the stage of the disease, and the general status of the patient. Surgery is considered primary treatment for breast cancer, as many early stage patients are cured with surgery alone.
Medical treatment may include chemotherapeutic drugs. These agents are divided into the following groups: natural products, angiogenesis inhibitors, and biologic therapy (immunotherapy).7,8 Tamoxifen is a selective estrogen receptor modulator (SERM) that binds to and inhibits estrogen receptor signaling in the breast. Remember that tamoxifen treatment might bring about ocular side effects, including maculopathy.
Radiation therapy may be indicated as either a therapeutic or palliative measure. Monoclonal antibody therapy and bone marrow transplant may also be effective.1,3,7
Treatment of choroidal metastasis is not without potential complications and side-effects, such as cataract, radiation retinopathy, optic neuropathy, exposure keratopathy, retinal detachment and epiretinal membrane.
While metastatic tumors of the choroid are the most common forms of intraocular malignancies in adults, advancements in cancer treatments have lengthened the life span of patients with ocular metastasis.
Optometrists must recognize the symptoms, clinical features, differential diagnoses, and current treatments/prognosis for this life-threatening condition. Proper management can often maintain patients’ vision and thus maximize their quality of life.
1. American Cancer Society. Breast Cancer Facts & Figures 2009-2010. Available at:
www.cancer.org/downloads/STT/F861009_final%209-08-09.pdf.
2. American Cancer Society. Risk Factors for Breast Cancer. Available at:
www.cancer.org/Cancer/BreastCancer/DetailedGuide/breast-cancer-risk-factors.
3. American Cancer Society. Cancer Facts & Figures 2009. Atlanta: American Cancer Society; 2009.
4. Quillen DA, Blodi BA. Intraocular Tumors. In: Clinical Retina. Chicago: American Medical Association Press; 2002: 208-9.
5. Wiegel T, Kreusel KM, Bornfeld N, et al. Frequency of asymptomatic choroidal metastasis in patients with disseminated breast cancer: results of a prospective screening programme. Br J Ophthalmol. 1998 Oct;82(10):1159-61.
6. Shields CL, Shields JA, Gross NE, et al. Survey of 520 eyes with uveal metastases. Ophthalmology. 1997 Aug;104(8):1265-76.
7. Weinberg RA. The Biology of Cancer. New York: Garland Science; 2006: ch.1-5.
8. Visvanathan K, Chlebowski RT, Hurley P, et al. American society of clinical oncology clinical practice guideline update on the use of pharmacologic interventions including tamoxifen, raloxifene, and aromatase inhibition for breast cancer risk reduction. J Clin Oncol. 2009 Jul 1;27(19):3235-58.

