 Q: I recently had a patient with all the signs and symptoms of thyroid eye disease, yet her medical doctor told her that her blood work for thyroid was normal. How can this be?
Q: I recently had a patient with all the signs and symptoms of thyroid eye disease, yet her medical doctor told her that her blood work for thyroid was normal. How can this be?
A: “Thyroid eye disease” is something of a misnomer because the orbitopathy is only associated with, but not necessarily caused by, abnormal thyroid hormone levels, says optometrist Dennis Mathews, associate professor at Southern College of Optometry, as well as a neuro-optometrist and partner at Eye Specialty Group, in Memphis, Tenn.
“The ocular orbital disease that we see is not from the hyperthyroidism itself, it’s from the autoimmune condition that caused the hyperthyroidism,” he says. This explains how a patient can have symptoms of thyroid eye disease, yet have normal thyroid levels.
“I had a patient like that very recently,” Dr. Mathews says. “She started out hyperthyroid for a year. Now she’s euthyroid (normal thyroid) without treatment, and yet she has grade III thyroid-related orbitopathy, also called Graves’ ophthalmopathy. It is a common misconception that the orbital disease should resolve once the patient shows normal thyroid levels.”
What’s going on? Two possible scenarios may explain the patient’s thyroid-related orbitopathy with normal thyroid levels, Dr. Mathews says:
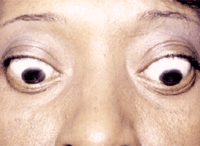
A thyroid patient with lid lag and lid retraction.
• The thyroid gland has not been affected by the autoimmune condition, but the orbit has.
• The patient’s thyroid levels fluctuate such that she had hyperthyroidism at one time but was euthyroid when the blood work was done.
“The reason for the hyperthyroidism in the first place is that abnormal lymphocytes release thyroid-stimulating antibodies that the thyroid gland mistakes for normal thyroid-stimulating hormone,” Dr. Mathews says. “These same antibodies also affect the orbit.”
Q: How should I treat these patients, and which specialists should I comanage with?
A: First, “when working these patients up, it’s important to image the orbit, because thyroid-related orbitopathy shows a very characteristic swelling of just the belly of the extraocular muscle, and not its insertion or origin,” Dr. Mathews says. “You can see this using CAT scan, MRI, or even ultrasound of the orbit.”
Document all your findings carefully in these patients, including a careful motility assessment and observation of lid lag or lid fatigue, measurement of lid fissures, and proptosis.
Coordinate treatment with the patient’s endocrinologist. “The systemic treatment for hyperthyroidism is usually radioactive iodine therapy.” Dr. Mathews says.
The optometrist should treat the orbitopathy as appropriate. “The first level of care is to lubricate the ocular surface and protect the cornea from exposure issues. Treat any inflammation of the ocular surface with a short-term topical steroid,” he says. “In cases where the motility deficit is significant, a short course of a high-dose oral steroids (60mg to 80mg a day of prednisone) should be considered. If the orbital disease is bad enough that the cornea is compromised, or the optic nerve is being compressed with disc edema and vision loss, surgery may be necessary. Orbital treatment could involve decompression surgery—where a fistula is created below the orbit to allow contents to drain down into the maxillary sinus—or radiation therapy to the orbit.”
Another important note: “In addition to the thyroid problem, the patient may also have myasthenia gravis—15% of the time they’re seen together,” he says. “If the patient has obvious thyroid orbital disease, but something doesn’t quite make sense—like maybe a droopy lid rather than lid retraction—then consider the possibility of myasthenia gravis.”

