 A 68-year-old Hispanic male presented for an annual eye exam. He reported occasional ocular itching, but otherwise was not experiencing any problems. His medical history was significant for hypertension, which he claimed was medically controlled.
A 68-year-old Hispanic male presented for an annual eye exam. He reported occasional ocular itching, but otherwise was not experiencing any problems. His medical history was significant for hypertension, which he claimed was medically controlled.
On examination, his best-corrected visual acuity was 20/20 OU. Confrontation visual fields were full to careful finger counting OU. His pupils were equally round and reactive, with no evidence of afferent defect. Extraocular motility testing was normal. The anterior segment examination of both eyes was unremarkable. Intraocular pressure measured 15mm Hg OU.
Dilated fundus exam revealed a clear vitreous OU. Both optic nerves appeared healthy, with small cups and good rim coloration and perfusion. The fundus evaluation of the left eye appeared normal, with an unremarkable peripheral retina.
The right macula was normal with a good foveal light reflex; however, we noted a subtle elevation located inferotemporal to the macula along the arcade (figure 1). In the same location, the retina exhibited a reddish hue over an area that measured approximately 2DD. We ordered a spectral-domain optical coherence tomography (SD-OCT) scan (figure 2) and an ultrasound (figure 3) of the right eye.
Take the Retina Quiz

1. Fundus photograph of
the right eye shows an imperceptible change in the retina along the
inferotemporal arcade. (Note: The round, white lesion is an artifact.)
1. The lesion primarily involves which retinal layer?
a. Sensory retina.
b. Bruch’s membrane.
c. Retinal pigment epithelium (RPE).
d. Choroid.
2. What is unique about the information provided by the SD-OCT scan?
a. The presence of choroidal fluid.
b. An extremely deep view into the choroid.
c. Significant retinal elevation.
d. Nothing.
3. What is the extent of the lesion’s reflectivity?
a. Too small to determine.
b. Low internal reflectivity.
c. Medium internal reflectivity.
d. High internal reflectivity.
4. What is the correct diagnosis?
a. Amelanotic nevus.
b. Choroidal melanoma.
c. Metastatic lesion.
d. Choroidal hemangioma.
5. How should this patient be managed?
a. Observation.
b. Intravitreal anti-VEGF injection.
c. Plaque radiotherapy.
d. Photodynamic therapy (PDT).
For answers, see below.
Discussion
On clinical examination of the right posterior pole, we detected a subtle reddish hue located inferotemporal to the macula along the inferior arcade. This really was noticeable only when looking at the area with indirect illumination. In other words, with the light source directed off to the lesion’s side, the affected retina and choroid exhibited a reddish glow.
We determined that this difference in coloration required closer inspection. Upon further evaluation, we detected an extremely subtle elevation of the retina and RPE. It was so subtle that we even questioned the accuracy of our observation. Fortunately, ancillary testing supported our clinical impression. Our primary suspicion was that this defect represented a small choroidal hemangioma.
An “enhanced depth” SD-OCT scan (which images deeper into the choroid) showed an obvious lesion pushing upward on the RPE. The consequent elevation was depicted on the scan as an optically empty space located below the RPE.

2. The SD-OCT scan of the lesion located in our patient's right eye. What is unique about this image?
In comparison to the lesion’s clinical appearance, its size and extent were exaggerated on SD-OCT. The scan also revealed no evidence of retinal or subretinal fluid.
Standardized ultrasound is perhaps the most useful diagnostic test for evaluating such a presentation. Unfortunately, our patient’s lesion was too small to identify its reflectivity on the A-scan.
However, the B-scan nicely complemented the SD-OCT findings––clearly revealing a dome-shaped lesion that measured slightly less than 1mm thick. Even though the A-scan did not provide definitive confirmation of what the lesion represented, we remained fairly certain that our patient exhibited a small choroidal hemangioma.
A choroidal hemangioma is a benign, vascular tumor of the choroid that is composed predominately of large, dilated, thin-walled vessels with minimal stroma. These tumors blend almost imperceptibly with the surrounding choroidal tissue. Usually, they are round or oval, and appear slightly elevated with a subtle, orange-red coloration.1 They often have indistinct borders, and are more apparent upon binocular indirect ophthalmoscopy. Choroidal hemangiomas typically are located in the posterior pole, within the paramacular area. Some, however, may be found adjacent to the optic nerve or on the nasal side of the disc.
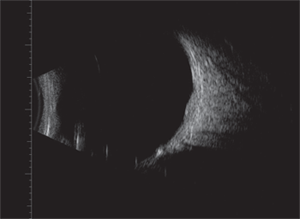
3. The B-scan component of our patient's ultrasound. What do you notice?
Most patients are asymptomatic and, as a result, the lesion may be discovered as an incidental finding. Interestingly, our patient had been seen several times over the last 10 years for annual eye examinations; however, we never noted this presentation. This likely was due to the extremely subtle elevation and the lack of associated symptoms.
These tumors generally do not grow much in adulthood. Some minor enlargement may occur later in life, but this is thought to result from varicosity and congestion of the large vascular channels.
Symptoms can develop if the lesion is located directly under the macula, or if the individual develops a neurosensory detachment involving the macula. If this occurs, photocoagulation is the traditional intervention of choice. Additionally, good success has been attained with newer, less invasive treatments, such as PDT and intravitreal anti-VEGF therapy. Nevertheless, most patients do not require treatment.
We explained the findings to our patient and asked him to return in four to six months to ensure that the lesion had not progressed.
1. Agarwal A. Neoplastic Diseases of the Choroid. In: Gass’ Atlas of Macular Diseases, 5th ed. Philadelphia: Elsevier Saunders; 2012:1206-53.
Answers
1. d
2.
b
3.
a
4. d
5. a

