 A 35-year-old white female presented with pain, redness and blurred vision in her left eye that had persisted for two weeks. She rated the severity of pain as an eight on a scale of one to 10. She said that the pain radiated to the left side of her head. One week earlier, she’d presented to a local emergency room and underwent an MRI. The MRI appeared normal. The attending ER physician prescribed her naproxen and hydrocodone.
A 35-year-old white female presented with pain, redness and blurred vision in her left eye that had persisted for two weeks. She rated the severity of pain as an eight on a scale of one to 10. She said that the pain radiated to the left side of her head. One week earlier, she’d presented to a local emergency room and underwent an MRI. The MRI appeared normal. The attending ER physician prescribed her naproxen and hydrocodone.
On examination, her best-corrected visual acuity was 20/20 O.D. and 20/400 O.S. Confrontation fields were full to careful finger counting O.U. Her pupils were equally round and reactive. There was a 2+ afferent pupillary defect in the left eye. Ishihara color testing was unremarkable in both eyes.
The anterior segment examination of the patient’s right eye was normal. However, her left eye revealed grade 1 to grade 2+ ciliary injection. Additionally, she had keratic precipitates (KP) on her endothelium and grade 1+ cells in her anterior chamber.
On dilated fundus exam, the vitreous was clear in her right eye. The left eye, however, showed grade 2+ vitreous cells.
The right optic nerve showed a moderate-sized cup, with good rim coloration and perfusion. Otherwise, the right eye was completely normal (figure 1).The left eye exhibited the changes seen in figure 2. We also ordered an optical coherence tomography scan of the left eye (figure 3).
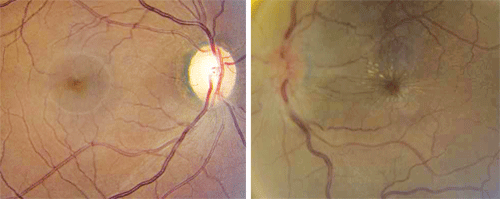
1, 2. Fundus images of our patient’s right and left eye (O.D. left, O.S. right). Note the changes in her left eye.
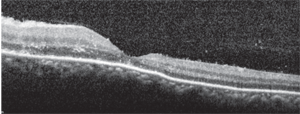
3. An OCT scan through the patient’s left macula. What do you see?
Take the Retina Quiz
1. What do the fundus changes in the patient’s left eye indicate?
a. Disc swelling and a macular star.
b. Clinically significant macular edema (CSME).
c. Dilated venous system and disc congestion from an impending central retinal vein occlusion (CRVO).
d. Neurosensory retinal detachment.
2. What does the OCT show?
a. Cystoid macular edema (CME).
b. Neurosensory detachment.
c. Mild macular thickening and exudate in Henle’s fiber layer.
d. A healthy macula.
3. What additional testing would be most helpful in making a correct diagnosis?
a. Visual fields.
b. Fasting blood glucose.
c. Blood testing that includes an enzyme-linked immunosorbent assay (ELISA) for Bartonella henselae.
d. Fluorescein angiography (FA).
4. What is the correct diagnosis?
a. Papilledema.
b. Moderate non-proliferative diabetic retinopathy with CSME.
c. Optic neuritis.
d. Neuroretinitis.
5. What is the recommended treatment for this patient?
a. Ciprofloxacin.
b. Doxycycline.
c. Observation.
d. Both a and b.
For answers, see below.
Discussion
In this case, our patient had neuroretinitis. This diagnosis was based on the presence of unilateral optic nerve swelling and a macular star in her left eye.
The term neuroretinitis is synonymous with Leber’s stellate neuroretinitis, a condition originally described in 1916 by Theodor Leber, M.D. He defined neuroretinitis as unilateral vision loss in the presence of a macular star.1 Leber believed that the finding was directly related to a retinal condition.
However, in 1977, J. Donald M. Gass, M.D., showed that patients with macular stars also experienced optic disc swelling both before and during the appearance of star formation.1,2 Gass concluded that the condition was not primarily a maculopathy, but an optic neuritis that affected both the optic nerve and retina.
Neuroretinitis affects patients of all ages, but is more commonly seen during the third to fourth decade of life. Generally, it is painless; however, patients have reported varying degrees of discomfort. Nearly 50% of patients with neuroretinitis experience a prior viral-like illness.1 As a result, the condition is sometimes classified as a “post-viral neuroretinitis.” The condition tends to be self-limiting after a period of six to eight weeks.1
The clinical features of neuroretinitis include disc swelling in the presence of an exudative maculopathy in a star-like pattern. The macular exudate may not be present during the initial stages of disc swelling, but will appear within several days to weeks, when the optic disc swelling begins to resolve. The exudate is located between the outer plexiform and inner nuclear layers within Henle’s fiber layer, and results in a macular star formation. Other inflammatory signs, including anterior chamber cell and flare, vitreous cells and venous sheathing, may also develop.
Cat-scratch disease (CSD) is recognized as one primary cause of Leber’s stellate neuroretinitis. Any patient with neuroretinitis should undergo an ELISA to rule out the presence of Bartonella henselae, the organism responsible for CSD.1,3
Other infectious conditions reportedly linked to neuroretinitis include syphilis, Lyme disease, leptospirosis, toxoplamsosis and toxocariasis. In many instances, an underlying cause is not identified.1
Our patient denied any exposure to cats or dogs. She also denied having any specific viral-like illness. Nonetheless, we ordered a medical work-up that included Bartonella henselae IgM and IgG titers; Treponema pallidum antibody testing to rule out syphilis; Lyme titers; HIV testing; and a tuberculosis screening. Additionally, we assessed her for elevated levels of angiotensin-converting enzyme (ACE), rheumatoid factor (RF) and C-reactive protein (CRP). All tests came back negative. As a result, we simply diagnosed her with neuroretinitis.
Treatment for neuroretinitis is controversial because the condition is self-limiting. Even in confirmed cases of neuroretinitis secondary to CSD, a decision to initiate treatment is never straightforward. Many physicians advocate oral antibiotic therapy, even though its efficacy is difficult to establish. Empirical therapy often includes azithromycin, ciprofloxacin, rifampin, trimethoprim and/or doxycycline.1
We placed our patient on 100mg oral doxycycline b.i.d. as well as Pred Forte (prednisolone acetate, Allergan) for her uveitis. The anterior uveitis quickly resolved, and she showed a steady improvement in visual acuity following resolution of disc edema and macular star formation. Three months after her initial office visit, her visual acuity improved to 20/20 O.S.
1. Smith CH. Optic Neuritis. In: Miller NR, Newman NJ (eds). Walsh & Hoyt’s Clinical Neuro-Ophthalmology. Vol. I, 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2005:293-347.
2. Dreyer RF, Hopen G, Gass JD, Smith JL. Leber’s idiopathic stellate neuroretinitis. Arch Ophthalmol. 1984 Aug;102(8):1140-5.
3. Ormerod LD, Skolnick KA, Menosky MM, et al. Retinal and choroidal manifestations of cat-scratch disease. Ophthalmology. 1998 Jun;105(6):1024-31.

