 |
Q:
A 60-year-old presented with unexplained lid droop after herpes zoster (HZ). I thought it was Ramsay Hunt syndrome until I saw him—no paralysis, very good seventh nerve function and the fifth intact as well. Could it be a facial spasm of some kind?A:
Ramsay Hunt Syndrome, also referred to as herpes zoster oticus, presents as a facial nerve palsy often accompanied by eye pain and hearing loss. This patient presented with a ptosis after a severe bout of herpes zoster on the right side, but cranial nerve (CN) VII function was intact and his hearing was normal. As a result, other conditions were considered.
“Essential blepharospasm and hemifacial spasm represent distinct categories of hyperkinetic eyelid movement disorders,” says Leonard V. Messner, OD, of the Illinois Eye Institute in Chicago. Essential blepharospasm (EB) is an idiopathic, involuntary, bilateral, forceful contraction of the orbicularis oculi muscles. Symptoms typically begin as sporadic episodes of eyelid closure with progression to more frequent and forceful contractions. According to Dr. Messner, typical age of onset is between 40 and 60, with women being affected more than men. The exact mechanism and pathophysiology of EB is unknown. The diagnosis of EB is based on clinical findings alone.
Bright lights frequently exacerbate EB. “An effective provocative test is examining the patient behind the slit lamp looking for increased intensity of the blepharospasm,” Dr. Messner says. “Recent studies show a benefit for light filtering lenses in the management of EB.” Neuroimaging studies are rarely indicated.
Treatment of EB is largely based on disease severity. Botulinum toxin injections minimize the frequency and intensity of EB. While effective, botulinum therapy typically lasts only three to four months and requires repeat injections. Since this patient’s lid closure was unilateral, EB was low on the differential list.
Lastly, perform a dilated fundus examination to rule out commotio retinae, a common finding of whitening of the retinal tissue which typically resolves on its own within two weeks. Other potential posterior segment findings include retinal detachment, vitreous hemorrhage and traumatic optic neuropathy.
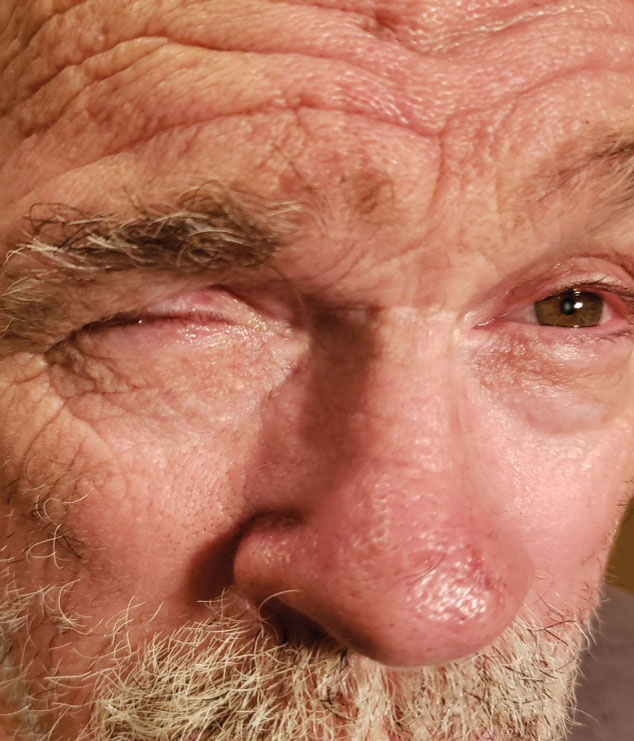 |
EB sets itself from HFS by being able to be diagnosed by clinical presentation alone. |
Mysterious Twitch
Hemifacial spasm (HFS) was also considered. HFS is a rhythmic, unilateral, involuntary twitching or contraction of the facial musculature. If intermittent, with episodes lasting seconds to minutes, it is most likely HFS due to disease of the posterior cranial fossa. If twitching is constant or exacerbated by a voluntary facial movement (e.g. blink or smile), it is probably aberrant regeneration of CN VII. With the latter, one would expect a prior history of a facial palsy with residual weakness.
Involuntary facial twitching often begins around the eyes with spread to the entire side of the face and neck. Women are affected more than men with a peak age of onset between 50 and 60. HFS’s etiology includes aberrant vascular loops, cerebellopontine angle tumors, intrinsic brainstem disease and idiopathic causes. Neurovascular compression of CN VII is most often associated with dolichoectasia of the vertebral artery or posterior inferior cerebellar artery. This is best appreciated with T2-weighted axial MRI sections at the level of the pons.
“Botulinum toxin injections are typically considered first line therapy for HFS as well,” Dr. Messner says. “For more recalcitrant cases, neurosurgical shielding the facial nerve from the offending artery is highly effective.”
Because there was no history of a prior Bell’s palsy or similar condition, HFS was ruled out in this case as well. An oculoplastic specialist was consulted. The working diagnosis was a reactive ptosis related to the zoster. The patient returned four months after the zoster had resolved, and the ptosis was 70% resolved. Another follow-up in three months was scheduled.

