As COVID-19 continues to make a rapid march across the country, optometrists are improvising to ensure continuity of patient care. While many ODs are faced with the difficult decision whether to put their practices on temporary hiatus, some eye care practitioners are turning to emergency-only visits or moving to telehealth to serve their patients without sight-threatening issues.
Still others are finding a way to make a difference by offering guidance to their colleagues on how their practices can not only withstand the current crisis, but what they can do to jumpstart their offices once their doors reopen after the fog of the pandemic clears.
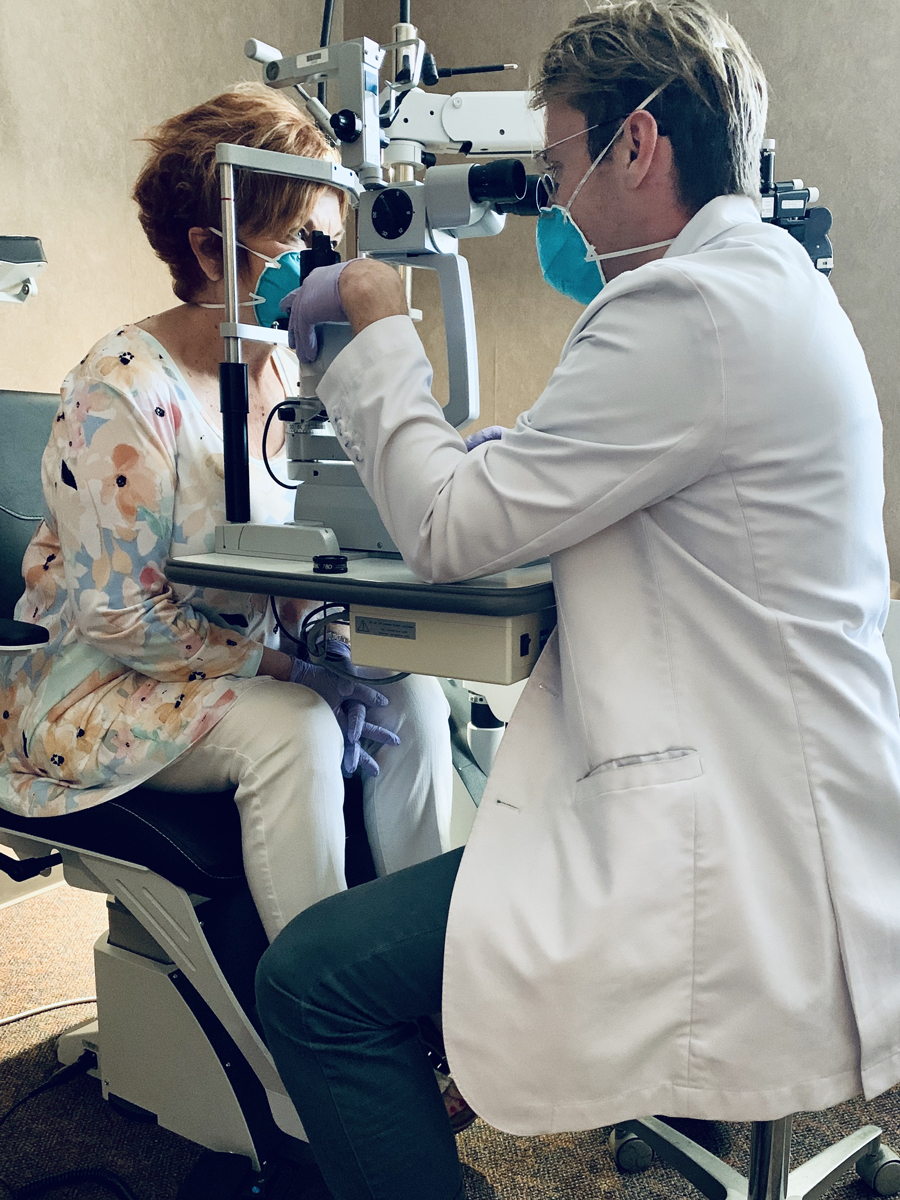 |
| Dr. Vollmer uses an N-95 mask and gloves when seeing patients, and he offers similar protective measures to his patients when they enter the office. Photo: Patrick Vollmer, OD. Click image to enlarge. |
Rising to the Occasion
The coronavirus outbreak has forced nearly every practice in the country to adapt, and what that means for most, including Patrick Vollmer, OD, of the Vita Eye Clinic in Shelby, NC, was to eliminate routine care.
“We felt this was the best recourse despite being considered ‘essential,’” he says.
Dr. Vollmer is keeping his clinic open for emergency visits and for two cohorts of research patients who are part of his practice’s dry eye clinical trials.
To ensure proper social distancing, he teleconferences with individual patients in one study group. The other study cohort comes into the office on a “one-in, one-out” basis.
Continuing to see patients who called in for urgent issues fills a critical patient care need and keeps Dr. Vollmer’s practice busy, despite cancelling routine visits.
“One of the important aspects that I learned—and really already knew—is how important it is to diversify your practice. If it wasn’t for emergency patients and ‘urgent’ needs, life would be pretty slow,” he says.
Still, urgent care was nothing new to Dr. Vollmer, who says he pursued an emergency model the first day he walked in the door of his practice and long before COVID-19 struck.
“I worked tirelessly in my community to establish medical and emergency eye care. This has proven to be a virtuous decision. To my knowledge, pretty much all of the hospitals, urgent cares and primary care offices are a bit overwhelmed with the COVID-19 response. They don’t want to deal with eye issues right now. A lot of these patients are getting funneled into my clinic day and night.”
At one point, Dr. Vollmer considered moving to a large city an hour away and commuting to his practice, but he’s thankful he decided against it, especially now with the high call volume due to the pandemic.
Since he only lives a few blocks away from his clinic, Dr. Vollmer can get to his office in a matter of minutes. On a typical week, he sees between five and 12 research patients and 20 to 25 emergency patients.
He sees one patient at a time, so there is never more than one patient in the clinic. To further ensure safety, Dr. Vollmer wears a N-95 mask and gloves, and all patients also receive masks and gloves at the door. When the patient leaves, everything is sterilized.
“It’s a pretty rogue procedure but it works,” he says.
Many of Dr. Vollmer’s current emergency patients tell him they would’ve normally gone to the emergency room (ER) or urgent care, but they were worried about being in a hospital setting.
“I take this opportunity to educate these new patients that they shouldn’t go the ER anyway. A lot of patients simply don’t know this despite going to their eye doctors for years. Optometry cannot assume patients know to come to their clinics for ocular emergencies,” he says.
Patients are appreciative of emergency care regardless, but they are especially grateful during this outbreak, Dr. Vollmer says. “I don’t charge an after-hours fee right now, and the most I charge for any procedure is around $150 if they have no insurance or a high deductible. It’s nice to be appreciated, but I get more fulfillment in knowing I helped someone in need.”
Turning to Telehealth
A series of federal, state and local COVID-19 mandates caused Kambiz Silani, OD, to cease all routine eye care at his Beverly Hills Optometry: Advanced Dry Eye Center practice in Southern California until further notice. Although his practice significantly reduced in-office services, Dr. Silani and his staff worked to reassure patients they would still be there for them through in-office emergency and telehealth visits.
Virtual Care Across the NationYou can hear more about how your optometric colleagues are handling telehealth in their practices in our recent news coverage, "New Week, New COVID Challenges Met." For more COVID-19 news, check out our comprehensive coverage here. |
“Our practice always considered telehealth in our pipeline,” Dr. Silani says. “After COVID-19 hit hard, telehealth quickly became a top priority so we could be available for our patients remotely.”
For his telemedicine platform, Dr. Silani chose Doxy.me, which is HIPPA compliant. Although he says FaceTime and Skype are adequate during the COVID-19 pandemic with temporary HIPAA leniency, he still found it beneficial to choose a platform that fit into his practice post-pandemic.
He describes the move to telehealth as a relatively smooth transition that provided patients calling in for routine issues and others already on the books the option to be seen sooner rather than waiting to reschedule until the practice fully reopened.
Telehealth visits do pose some limitations based on the reason for the patient visit, Dr. Silani says. “We don’t have the ability to perform contact lens evaluations or routine eye care via telehealth visits.” Dr. Silani also encourages patients to come into the office if they have sudden vision loss, onset of floaters/flashes or any eye pain.
What does fall under the practice’s telehealth umbrella are dry eye consults and mild to moderate issues such as styes, red eyes, watery eyes and ocular irritation.
To get the word out about the new telehealth platform, Dr. Silani’s staff shared the news on the practice’s social media platforms and also as an e-mail campaign to reach current patients.
Dr. Silani was quick to hammer out a template for a typical telehealth consult:
- When a patient contacts the practice for an appointment, staff offers the option and benefits of booking a telehealth visit.
- Staff then books an appointment for the doctor/patient video visit.
- Staff sends the patient a consent form highlighting the features, benefits and potential risks of telehealth and collects payment via credit card.
- The doctor and patient engage in the video visit. At the completion, the doctor determines whether the patient needs to be seen for a follow-up (either virtual visit or in-office), if the patient needs a prescription sent to the pharmacy, or if a referral to a specialist, such as a neuro-ophthalmology, retina, cornea or glaucoma, is warranted.
- Finally, the doctor shares the notes of the visit with the staff to upload into the patient’s chart.
“If eligible for a virtual appointment, patients enjoy the convenience, comfort and safety of this option,” Dr. Silani says. “After the COVID-19 outbreak has ended, we will certainly continue offering this service as an option for our new consults and pre-existing patients.”
Because the platform and service are new to both Dr. Silani’s practice and patients, he estimates his office is currently conducting three to five telehealth visits a week, with the hope the number will continue to rise, especially for some out-of-town patients and ones who commute long distances.
Looking to the future, he adds: “Although COVID-19 presents many challenges to eye care practitioners, it is key to adapt and pivot. Use this added, precious time to dabble with new ideas, services, products, update marketing material, create a blog or attend virtual CEs and webinars.”
As New York City became the epicenter of the COVID-19 outbreak in the United States, Justin Bazan, OD, of Park Slope Eye in Brooklyn, NY, physically closed his office due to the increased health risk he saw for himself and his staff. He headed to the mountains temporarily where he’s also taking care of his patients through telehealth visits. He coordinated with a local practice to handle emergency referrals and directed his employees to work entirely from home, since he felt the risk for them to return to the office was too great.
Dr. Bazan says he feels very fortunate and thankful he had the opportunity to leave the city, yet “his heart bleeds” for those residents who couldn’t.
“We wanted to provide help to people in need, and telemed and digital communication is the best we can do that right now. We have always answered a lot of questions and provided advice via email, so it was an easy and natural progression into using a formal telemed platform.” Still, “the amount we are doing is minuscule compared to our normal in-office flow,” he admits.
Dr. Bazan says the learning curve for telehealth is very low. He suggests ODs test drive a few of the popular platforms and they can watch an AOA telemedicine webinar as a helpful resource if they are considering this option.
 |
| The Memphis VA Medical Center now provides a convenient drive-through lab to help patients get the labwork they need without risking exposure in the hospital. Photos: Memphis VA Medical Center. Click image to enlarge. |
Drive-through Clinics Help Social Distancing
Working at the front lines at the Memphis VA Medical Center, Katherine Sanford, OD, easily answered the “all hands on deck” call when her hospital decided to roll out its drive-through clinic to promote social distancing while still providing continuity of care for veterans.
“I live in Memphis, so there’s a lot of diabetes, high blood pressure and other chronic conditions that need to be monitored,” she says.
And while the hospital previously launched an intensive telemedicine program for primary care visits, the drive-through lab for blood work—which was officially launched this week—was the VA Center’s latest push to take care of patients and ensure their safety during the pandemic.
Although the new lab is phlebotomy based, Dr. Sanford was eager to lend a hand in helping organize and facilitate the effort when she wasn’t in the clinic, especially since she had some extra time on her hands without routine care visits on her schedule.
“The majority of patients have appointments for labs,” Dr. Sanford explains. “They can still go inside the hospital to the main lab, but we are funneling every visitor and every employee into one entrance.” In addition to social distancing, the drive-through lab provides convenience for those with ambulatory issues who would otherwise have to navigate through the building until they reach the main lab located on the far end of the hospital, Dr. Sanford says.
Here’s how it works:
A patient pulls up in their car to a station for screening questions. Based on their answers, hospital workers will put a colored strip of paper on their windshield. A red slip of paper indicates a patient may have been exposed or is exhibiting symptoms of COVID-19 and hospital staff shouldn’t approach the vehicle. In this case, the individual will be redirected to the ER and personnel will be notified before the patient’s arrival so they can take necessary precautions.
Patients who are asymptomatic or who indicate they were not exposed to anyone with symptoms get a green slip of paper, alerting staff that it’s safe to approach them.
The drive-through lab can handle two cars at a time. When the patient reaches one of two bays, they get out of their vehicle and enter a side room inside a large tent where a phlebotomist takes their blood for the specific tests their doctor ordered.
The patient then will generally return home where they will have a telemedicine visit with their primary care physician to discuss the results and any other issues.
The first day of the drive-through lab had 35 patients, but the hospital is anticipating up to 150 per day.
“It’s good to feel like we are providing an extra service for the veterans,” Dr. Sanford says.
 |
| This drive-through lab can handle two cars at a time, as blood tests are taken in the tent. Photo: Memphis VA Medical Center. Click image to enlarge. |
Finding Purpose in the Chaos
When Samantha Hornberger, OD, of Bright Family Eyecare in Lawrenceburg, IN, suddenly had to temporarily close her office to routine care in mid-March, she picked up a notebook and pen and started jotting down a plan.
What came next was a comprehensive, step-by-step manual called “Office Closure Action Plan: A Plan for COVID-19 Closure.” The document details what doctors can do to best position themselves in this unprecedented time and how to reboot after reopening.
Dr. Hornberger said her brainstorming gave her less anxiety about what was happening around her. “I thought, if this makes me feel better to have an organized plan, it’s going to make others feel better too.”
Hornberger’s COVID-19 practice roadmap offers immediate and post-pandemic advice for ODs, including how to continue to generate revenue, reaching out to suppliers and vendors about the potential to defer, delay or alter payment arrangements, how to get the word out to the community that you’re still open for emergency visits and tips on sanitizing the office and scheduling and launching a telehealth platform.
Her guide has already become a valuable resource for hundreds in the profession, as more than 700 eye care practitioners have either downloaded it or connected with her on social media, she says.
Dr. Hornberger is currently working on the next update to the manual. The new section will offer suggestions on how doctors can start envisioning changes they’d like to make to their practice that would reduce burnout and stress.
“Honestly, there has never been a better time to think about this, because we won’t go back to normal right away. Who knows what normal is even going to look like. There will be a transition period where you can make the changes you want to make even if they aren’t COVID-related.”
In the meantime, Dr. Hornberger encourages her colleagues to persevere and persist, two traits in which she feels the profession already excels. And during this unprecedented time, Dr. Hornberger still suggests trying to find small joys throughout the day.
“I fully believe we are going to find good that’s going to come out of this if we look for it.”
Dr. Hornberger’s guide can be found on her website at themoderneyesite.com.

