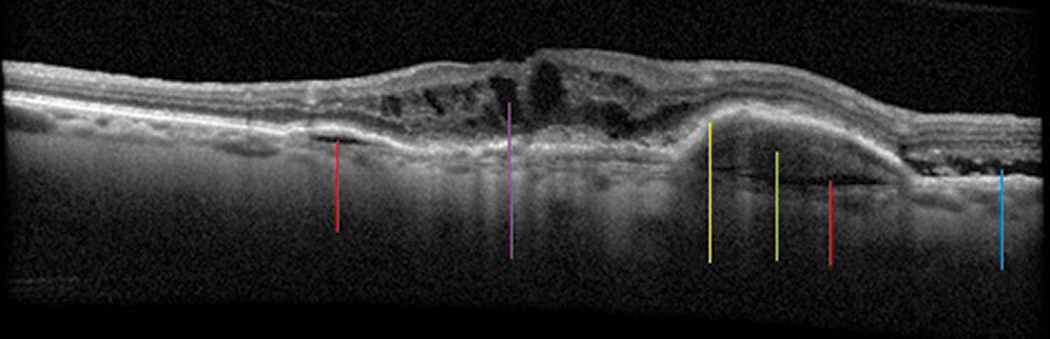
 |
PED and SRF developed in a substantial proportion of patients with type 3 |
Pigment epithelial detachment (PED) progression in type 3 neovascularization (MNV) indicates the progression of the lesion into the sub-retinal pigment epithelium (RPE) space, and MNV patients with PED may require treatment to preserve vision. To understand more about this progression, researchers evaluated the incidence and timing of PED and subretinal fluid (SRF) development in type 3 MNV.
Included were a total of 84 patients who were diagnosed with treatment-naïve type 3 MNV who did not show SRF at diagnosis. All patients were initially treated with three loading injections of ranibizumab or aflibercept. Following the initial loading injections, the regimen was evaluated for retreatment as needed. The development of either PED or SRF was assessed. The incidence and timing of PED development in patients without PED at diagnosis and that of SRF development in patients with PED at diagnosis were also evaluated.
The incidence of PED development was high at 62.5% among patients without the condition at diagnosis and was noted at the first or second lesion reactivation.
“This suggests that type 3 MNV progresses in the majority of patients after initial anti-VEGF therapy, emphasizing the progressive nature of the disorder,” the authors noted.
Most of these findings first developed at the first and second lesion reactivation, suggesting the need for active treatment such as TAE during the early treatment period to improve treatment outcomes, the authors suggest.
“TAE should be started during the early treatment period to impede stage progression or at least to avoid serious adverse events such as subretinal hemorrhage or RPE tear,” the authors suggested. “We recommend starting TAE immediately either after the diagnosis or at least after the first lesion reactivation. In the latter case, frequent follow-ups are required until the first reactivation to promptly detect lesion reactivation and stage progression. In particular, since greater central retinal thickness was associated with a high risk of PED development, applying TAE immediately after three initial loading injections would be appropriate for patients exhibiting severe intraretinal edema at diagnosis.”
SRF developed during the follow-up period in 28.8% of the patients with PED at initial diagnosis. In addition, among the 32 patients without PED at diagnosis, SRF eventually developed in 18.8%, and the incidence of SRF development was 25% in the entire study population.
The authors note that the presence of SRF in type 3 MNV may indicate high hydrostatic pressure from the neovascular lesion, severe hypoxic environment or diminished RPE function, suggesting a chronic and advanced form of the disease.
“If the presence of SRF indicates advanced disease, it would be a plausible approach to prevent the development of SRF or at least to perform aggressive treatment for patients with SRF,” they wrote in their paper. “Similar to PED development, the majority of SRF developed during the early treatment period, suggesting the need for early aggressive treatment in patients with PED. In particular, because PED and SRF can codevelop during follow-up, care should be taken even in patients without PED at diagnosis.”
Kim JH, Kim JW, Kim CG. Incidence and timing of pigment epithelial detachment and subretinal fluid development in type 3 macular neovascularization associated with age-related macular degeneration. Retina. March 27, 2023. [Epub ahead of print]. |

