Although the elective refractive surgery market, such as LASIK, has been down due to the economy, many patients are electing for the implementation of premium intraocular lenses to address their visual needs. The reason for this difference is that refractive surgery usually can be put on hold, whereas cataract surgery usually cannot.
Furthermore, patients have just one opportunity to choose what type of vision they wish to receive from their cataract procedure. Due to their decreased functional vision, many cataract patients do not choose to put off this important decision based on economics.
Additionally, the majority of cataract patients are baby boomers who have the discretionary income to spend money and want to appeal to their younger side).1 This means these patients are willing and able to purchase these technologies.
As optometrists, we have an opportunity and responsibility to offer our patients advanced refractive technologies to improve quality of life by addressing both the quality and quantity of their vision. Baby boomers (those born between 1946 and 1964) start turning 65 in 2011, and the number of older people will increase dramatically between 2010 and 2030.2
Currently, more than three million cataract surgeries are performed each year, and the number of surgeons offering premium IOLs continues to grow.3 As a result, optometrists can demonstrate they provide state-of-the-art care by becoming proactively involved in the perioperative care for these cutting-edge technologies. According to a 2008 survey of cataract and refractive surgeons cited by Market Scope, 71% of U.S. ophthalmic surgeons were offering premium IOLs in their practice, up from around 59% in 2007.4 This growth, along with aging patients and their visual demands, suggests that patients are interested and can benefit from these premium IOL technologies.
Who is better positioned than optometrists to educate these patients about this new technology? No one. Optometrists are more likely to make informed recommendations to long-term patients than the surgeon, who has to make his recommendation in a five-minute encounter.
This article encourages optometrists to become actively involved in the clinical and coding/billing aspects of cataract and refractive surgery.
Balance Billing Background

With advancements in premium IOLs, cataract patients have become the new refractive surgery patients.
Let’s revisit a little history. In May 2005, Medicare set forth a policy concerning the requirements for determining payment for insertion of presbyopia-correcting intraocular lenses (PCIOLs) following cataract surgery (
www.cms.hhs.gov/Rulings/downloads/CMSR0501.pdf). This ruling from the Centers for Medicare & Medicaid Services (CMS), which allows surgeons to bill the patient for the extra costs involved in implanting these lenses, was certainly unprecedented in the ophthalmic area.
This CMS policy created a new market within optometry and ophthalmology, specifically for patients aged 50 years and older. This particular market demographic continues to experience tremendous growth. The 50+ market is expected to grow seven times faster than any other segment during the next 15 years, while the volume of refractive surgical candidates have decreased or are flat because baby boomers have reached their 50s. Although 50-somethings may not make good refractive surgery candidates, they certainly are candidates for a presbyopia-correcting IOL.
Then, in January 2007, Medicare set forth policy concerning the requirements for determining payment for insertion of astigmatism-correcting intraocular lenses (ACIOLs) following cataract surgery (
www.cms.hhs.gov/Rulings/downloads/CMS1536R.pdf).
These recent Medicare rulings concerning presbyopic and astigmatic correcting IOLs is a huge win for cataract surgery patients and physicians alike. Before this ruling, Medicare patients who needed cataract surgery were denied access to approved multifocal IOLs or toric lenses for astigmatism. Furthermore, any extra tests and work specifically related to the correction of either presbyopia or astigmatism are not covered and need to be charged directly to the patient as an out-of-pocket fee.
This also represented a change in policy and procedure. Rather than send a claim directly to Medicare for payment, both optometrists and ophthalmologists must bill patients directly for these services and the non-covered component of the IOL itself, which in and of itself requires even greater communication and coordination between these two groups to achieve the best outcomes that this technology can deliver.
These CMS rulings essentially removed the balance-billing obstacle by establishing that all charges, either by physician or facility, for additional items and services intended to correct presbyopia or astigmatism are non-covered services. Consequently, collecting for non-covered services from the patient doesn’t constitute balance billing and effectively removes the intrinsic obstacles contained within the process.
As a result, Medicare beneficiaries may upgrade from a conventional monofocal IOL to either a PCIOL or ACIOL, as long as they request the additional products/services and are willing to pay all charges beyond those associated with standard cataract surgery. To the extent that Medicare patients are willing to pay the extra costs for a PCIOL or ACIOL, facilities and physicians may receive an additional payment from the patient than that amount allowed by Medicare for insertion of a conventional IOL following cataract removal.
Prior to the May 2005 ruling, Medicare officials understood that the new IOL technology was something that patients were interested in receiving and that rules in place at that time were an obstacle to good patient care. As long as providers and patients have an honest discussion about the pros and cons of the lenses and the cost and coverage differences between conventional and premium IOLs, it creates a win-win-win situation for all concerned. This decision represented an important new beginning for Medicare policy, moving us in the direction of technological advance, individual choice, and patient supremacy over bureaucracy.
With the advancements in premium IOL technology, our cataract patients have become the new refractive surgery patients, and patients are benefiting from an improved quality of life due to an increase in spectacle independence. By utilizing these implants, we are able to offer our patients cutting-edge technologies that are able to meet and exceed their expectations. As their eye care providers, we understand that patients have greater expectations for surgery with a goal of 20/20 in the distance, and they are reluctant to wear reading glasses unless they have no other choice. As long as our premium IOL patients understand that there is a compromise with any IOL, whether standard or premium, this will lead to more “20/Happy” patients.
LASIK Down, Not Out
The refractive surgery market has taken a hit in the last decade or so due to several factors, mainly the economic downturn of recent years. With the uncertainty of our economy, consumers find it easier to cut back on elective procedures such as LASIK surgery.
Yet, there are many patients who are still interested in increased spectacle independence, in particular Generation Y (about 18 to 30 years of age). A combination of four factors will continue to influence adoption of LASIK by Generation Y:5
• Familiarity. They know of someone who had LASIK.
• Affordability. Many Generation Y patients still have family who can support them financially.
• Luxury. They’re willing to spend on luxury goods.
• Longevity. The procedure will last them for many years.
Advancements in refractive technologies—such as the femtosecond laser, wavefront-optimized and guided ablations, implantable collamer lenses, and future presbyopic ablations—have expanded our treatment options while allowing eye care providers to choose the best options for different patients.
Additionally, eye care providers have been much more attuned to proper patient selection, patient education and proactively addressing issues preoperatively, such as ocular surface disease. These factors have led to greater results, higher patient satisfaction and a renewed interest in refractive procedures.
With such positive buzz, an economy slowly returning to life and consumers’ rising confidence, LASIK volumes are expected to recover from being down 25.9% across the country in 2009 compared with 2008.6,7
As their primary eye doctor, we must be ready to discuss and offer these refractive technologies to our patients. If we don’t, patients who are interested in refractive surgery will bypass their optometrist and may not choose to be comanaged despite the comanagement center’s best efforts.
The Preoperative Evaluation
When cataracts become visually significant, the preoperative cataract evaluation is more involved than the standard work-up and additional testing is required. (See “Premium IOL/LASIK Non-covered O.D. Services,” below.)

One of the most important conditions to address preoperatively with both cataract and refractive surgery is ocular surface disease (OSD). By addressing OSD preoperatively, the accuracy of measurements is improved, the final outcome is maximized and the postoperative dry eye symptoms have less impact on our patients.
Because these are our patients and we understand their needs, our role is to offer premium IOL technologies to those patients who we know would be good candidates—as long as they have realistic expectations. A thorough discussion is critical to ensure that patient’s understand what a cataract is, who to go to for surgery, which IOL to select, and your role in the postoperative care.
Have a staff member schedule the appointment for the patient with the surgeon’s office, in addition to sending over a referral request form with the recommended IOL, patient notes, and the consent for comanagement form. The consent for comanagement form is important for two reasons: It is required for documentation; and reviewing the form with your patients helps them understand your role in the postoperative care. Patients are more than willing to be comanaged with their optometrist if they understand the O.D.’s role in the postoperative care.
The Business Model
The discussion of comanagement fees for premium IOL technology and refractive surgery are very straightforward, with appropriate fees going to the ambulatory surgery center, the surgeon, and the comanaging optometrist. The typical cost for premium IOL technology ranges from $1,000 to $3,000, depending on whether the surgeon bundles the refractive package. It is important to discuss with your surgeon whether the premium IOL fee is bundled (including refractive enhancements), and about your own fee schedule for providing pre-/postoperative care.
During surgery scheduling, patients review the informed consent for the procedure, choose to have their postoperative care comanaged, discuss the elective portion of the procedure (including the Notice of Exclusion from Medicare Benefit or the Advance Beneficiary Notice forms), and review the fees involved.
Both the surgeon and the optometrist bill the patients’ insurance for the surgery and postoperative care and charge the patient individually for their respective services that represent the work involved for the premium portion of the IOL. It is not uncommon for patients to make out three separate checks/payments to each entity, which clearly defines where appropriate premium IOL fees are going.
While 20% is the maximum amount the comanaging physician makes for a traditional, non-premium IOL, this 20% model does not apply to premium IOLs. Be sure that the additional fee you charge is commensurate with the amount of work you perform in respect to the premium portion of the IOL; it may be greater than 20% or it may be less than 20% of the additional amount. This can include addressing any ocular surface diseases; educating patients on the technologies, risks, benefits and alternatives to surgery; and providing the postoperative care and education.
After each visit, the surgeon and the comanaging optometrist are required to fax over postoperative reports to each other to document visits in the patient records. There are several reasons to do this: it is proof to insurance carriers that the postoperative care was performed; it is required by insurance carriers; and it provides good patient care through a check-and-balance system.
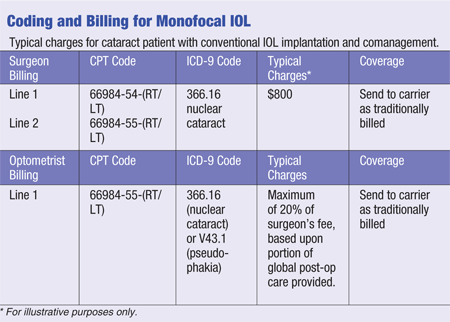
Let’s review traditional monofocal implantation, followed by a discussion of premium IOL implantation.
MONOFOCAL IMPLANTATION
Pre-op Visual Testing
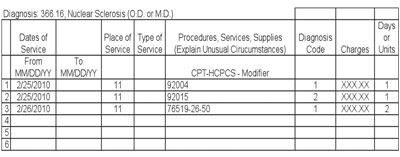
In most cases involving a simple cataract, a diagnostic ultrasound A-scan is used.
Prior to cataract surgery with a traditional monofocal implant, a comprehensive eye examination (ocular history and ocular examination) and a single scan to determine the appropriate pseudophakic power of the intraocular lens are usually all that are required. In most cases involving a simple cataract, a diagnostic ultrasound A-scan is used (76519; see example below). For patients with a dense cataract, an ultrasound B-scan may be used.
Accordingly, when the only diagnosis is cataract(s), Medicare does not routinely cover testing other than one comprehensive eye examination (or a combination of a brief/intermediate examination not to exceed the charge of a comprehensive examination) and an A-scan or, if medically justified, a B-scan. Claims for additional tests are denied as not reasonable and necessary unless there is an additional diagnosis and the medical necessity for the additional tests is fully documented.
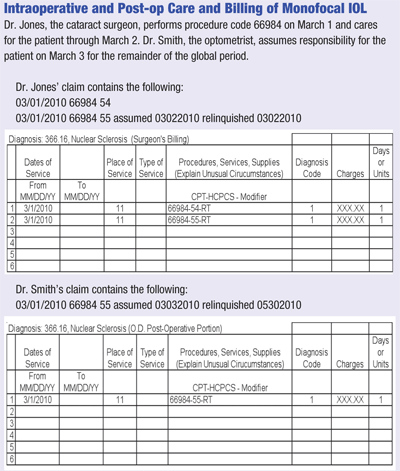
Transfer of Care
Ordinarily, the global surgery fee schedule allowance includes preoperative evaluation and management services rendered the day of or the day before surgery, the surgical procedure, and the postoperative care services within the defined postoperative period. Postoperative care may be rendered by an ophthalmologist, optometrist, or a provider who is licensed to render such services.
When a physician transfers the care of a patient to another provider outside their group practice within the global period, it is considered “a transfer of care.” A transfer of care occurs when the referring physician transfers the responsibility for the patient’s complete care to the receiving physician at the time of referral, and the receiving physician documents approval of care in advance. Each provider must agree and document the transfer of care in the medical record. The agreement must be in the form of a letter or written as a notation in the discharge summary/hospital records or ambulatory surgical center records. The appropriate CPT-4 modifiers must be added to the surgical procedure code:
• –54 Surgical care only.
• –55 Postoperative management only.
• –79 Unrelated procedure or service by the same physician during the postoperative period.
The claim for the “surgical care only” and the claim for the “postoperative care only” must identify the same surgical date of service and the same surgical procedure code. Modifier -54 must be reported with the surgical care only. For claims in which physicians share postoperative care, the assumed and/or relinquished dates of care must be indicated in Item 19 of the CMS-1500 claim form, or electronic media claim equivalent.
When a transfer of postoperative care occurs, the receiving physician cannot bill for any part of the global services until he/she has provided at least one service. Once the physician has seen the patient, that physician may bill for the service. When more than one physician bills for the postoperative care, the postoperative percentage is apportioned based on the number of days each physician was responsible for the patient’s care. The maximum percentage for postoperative care for 66984 is 20%, and the length of the associated global period is 90 days.
Generally, the diagnosis for cataract is the most appropriate (366.XX) to use, but many carriers will also accept pseudophakia (V43.1) code for the postoperative portion of care.
PREMIUM IOL IMPLANTATION
Pre-op Visual Testing
Just as in conventional or traditional monofocal implantation surgery, a comprehensive eye examination (ocular history and ocular examination) and a single scan to determine the appropriate pseudophakic power of the intraocular lens is covered by Medicare when the only diagnosis is cataract(s).
However, when the patient requests an upgrade to a PCIOL, there are additional tests, both pre- and postoperative, that if medically necessary may be billed directly to the patient because they are deemed non-covered services. The typical set of additional tests performed, in addition to the comprehensive examination and A-scan, could include:
• Initial consult (separate from comprehensive exam)
• Dry eye evaluation and treatment
• Corneal topography
• Wavefront aberration testing
• Pachymetry
• Additional A-scan and IOLmaster
• Contact lens trial fitting
• Additional refractions, postoperative evaluations and progress evaluations to deal with residual refractive error
• Refractive surgical procedures for the purpose of reducing dependence on eyeglasses or contact lenses (e.g., limbal relaxing incisions, corneal relaxing incisions, LASIK, etc.).
These additional tests and care protocols may be itemized to the patient or globally grouped into a PCIOL package of services that is directly billed to the patient. Keep in mind, however, that the surgeon, the O.D., and most importantly, the patient, must have a clear understanding of the additional services performed, who’s performing them, and what the associated cost will be prior to them being provided.
Using an ABN or NEMB
Because the carrier does not cover these additional tests, and the patient will most likely be bearing 100% of the additional non-covered cost, there are strict rules of notification that must be followed before performing and billing the tests. Have the patient sign a waiver and keep it with the chart. It is critical that all the specifics of the elective part of the procedure need to be detailed in this waiver to be given to and signed by the patient. The waiver should clearly define what Medicare pays for and for what the patient is financially responsible.
The most appropriate document for this purpose is NOT the Advance Beneficiary Notice (ABN) as is commonly used in day-to-day practice, but is the CMS document called the Notice of Exclusions from Medicare Benefits (NEMB) form (
www.cms.hhs.gov/BNI/Downloads/CMS20007English.pdf). While this form is not required, its use is “strongly encouraged” by CMS. This form is not to be sent to Medicare; its purpose is for documentation only and should remain in the patient’s file.
Pick the Right Surgical Code
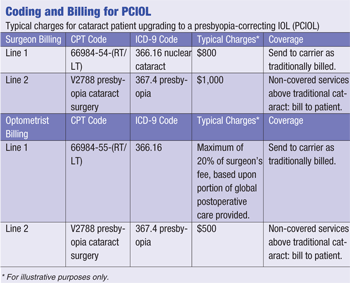
The CPT code for standard cataract surgery fees is 66984, and it is recommended that physicians’ offices use this code when billing Medicare or commercial insurance when a patient elects a PCIOL.
CPT code 66984 is for the covered portion of the surgery and IOL. That part of the process should be billed in standard fashion. For the non-covered upgrade, code V2788 should be used to describe the upgrade to a PCIOL. Surgeons should not use CPT 66982 (complex cataract) when implanting presbyopia-correcting IOLs, unless the requirements of code 66982, as defined in the CPT, are also met or physicians receive specific instructions from CMS that state that this is acceptable.
Be aware that the Office of Inspector General is watching for patterns of abuse with the advent of this new policy, so surgeons and O.D.s alike should be careful not to change patterns of recommending cataract surgery to their patients. Moreover, surgeons cannot require patients to elect a PCIOL as a condition of implanting an IOL; the patient must always have the option of selecting a conventional monofocal IOL.
Charging the Patient
The beneficiary is responsible for paying for the portion of the physician’s charge for the PCIOL that exceeds the physician’s charge for a conventional IOL. There are many non-covered technical work expenses associated with the preoperative process of presbyopic cataract surgery and many additional non-covered work expenditures associated with the postoperative care, which is necessary in order for patients to achieve satisfactory near, intermediate and distance vision.
While most surgeons anticipate that residual refractive error will be corrected with additional surgery, keep in mind that the existing covered Medicare benefit of one pair of spectacle lenses, an ophthalmic frame, or one pair of contact lenses per surgery remains intact even for the patient who requested the upgrade to a PCIOL procedure/product.
Transfer of Care
Just as with traditional monofocal implantation surgery, the global surgery fee schedule allowance includes preoperative evaluation and management services rendered the day of or the day before surgery, the surgical procedure, and the postoperative care services within the defined postoperative period. Postoperative care may be rendered by an ophthalmologist, optometrist or other provider who is licensed to render such services, and all of the same guidelines remain as explained earlier.
Implications for Optometry
These rulings from CMS certainly sounded a clarion call in policy shift for both patients and physicians. Patients now have the option of having the best technology available to satisfy their visual needs for their lifestyles, and O.D.s and M.D.s can provide it without the fear of losing significant revenue. These rulings create a climate for a true win-win-win for the O.D., the M.D., and most importantly for the patient who is able to now have options in their own health care decisions. Ophthalmology and optometry can and must work together to bring this exciting new technology to the mainstream.
Because O.D.s provide the majority of primary eye care visits in the country, it is vitally important that we are knowledgeable about these technologies and the opportunity that exists by educating our patients about them. We are in a key position to understand the intricacies of patient expectations in combination with patient refractive states and visual needs. As we continue to improve our understanding of the differences in premium IOL technology, it is important that we take the time to educate our patients about their surgical decisions including what a cataract is, who the best surgeon is to perform the procedure, and which IOL or refractive surgery option is best for them. As their doctor, we need to inform our patients that we will help them make this important decision, and that we will continue to provide their care after the procedure.
Before patients leave the office, they should be given educational materials on cataracts or refractive surgery, the surgical procedure, and materials that explain IOL/refractive surgical options. Additionally, a staff member should help schedule the patient for a surgical evaluation. It is important for optometrists to give their patients a direct referral to a specific surgeon with whom they have established a trusting relationship, such as someone who they would have perform surgery on themselves or their family.
Although this technology may not be for everyone, optometrists must take an active role in educating their patients. By offering premium IOL technology to our patients, optometrists can showcase these cutting-edge technologies that have been clinically proven to be successful in improving patients’ quantity and quality of vision after cataract or refractive surgery.
With the “boomer generation” having less than a year before hitting the Medicare system, we have the tools at our disposal to satisfy their visual demands, and preserve their active lifestyles.
The government has done its part to create policy that provides us flexibility and options in being able to fulfill our patient demands without financial compromise. Don’t be left out of being a part of these exciting times in eye care. Take advantage of the opportunity before you and make the most of it—for your patient, your practice and yourself.
Dr. Rumpakis is the founder of Practice Resource Management, a management and consulting firm. He lectures nationally and internationally on medical coding & compliance topics, as well as on managed care, contact lenses and refractive surgical procedures. He is Clinical Coding Editor for Review’s “Coding Abstract” column.
Dr. Whitley is the director of optometric services at Virginia Eye Consultants, in Norfolk, Va., a tertiary referral care center. He is also an adjunct assistant clinical professor at Pacific University College of Optometry, Pennsylvania College of Optometry and Southern California College of Optometry.
1. Burns D. Baby boomers are still the largest consumer group in America—even in a recession. BabyBoomer Magazine.com. 2010 July 25. Available at:
www.babyboomer-magazine.com/news/165/ARTICLE/1217/2009-12-22.html (accessed October 11, 2010).
2. Federal Interagency Forum on Aging-Related Statistics. Number of older Americans [Data file]. Administration on Aging website. 2008. Available at:
www.aoa.gov/agingstatsdotnet/Main_Site/Data/2008_Documents/Population.aspx (accessed October 11, 2010).
3. Lee J, Bailey G. Cataracts. All About Vision website. 2010 Oct 11. Available at:
www.allaboutvision.com/conditions/cataracts.htm (accessed October 11, 2010).
4. Freeman W. Global demand for presbyopia-correcting IOLs grows. Market Scope. 2008;13(8):1,4-6.
5. Mahdavi S. Future growth of LASIK: understanding and reaching generation Y. SM2 Strategic website. 2008. Available at:
http://sm2strategic.com/files/AMO%20Paper08_5.pdf (accessed October 11, 2010).
6. Majmudar PA. Lasik and the economy: where have we been, and where are we going? Cat Ref Surg Today. 2010 March. Available at:
http://bmctoday.net/crstoday/2010/03/article.asp?f=lasik-and-the-economy-where-have-we-been-and-where-are-we-going (accessed October 11, 2010).
7. Market Scope. Quarterly Updates on the US Refractive Market. Q4-2009 US Refractive Update. Market Scope website. Available at:
www.marketscope.com/market_reports/refractive_reports.html (accessed October 11, 2010).

