 |
|
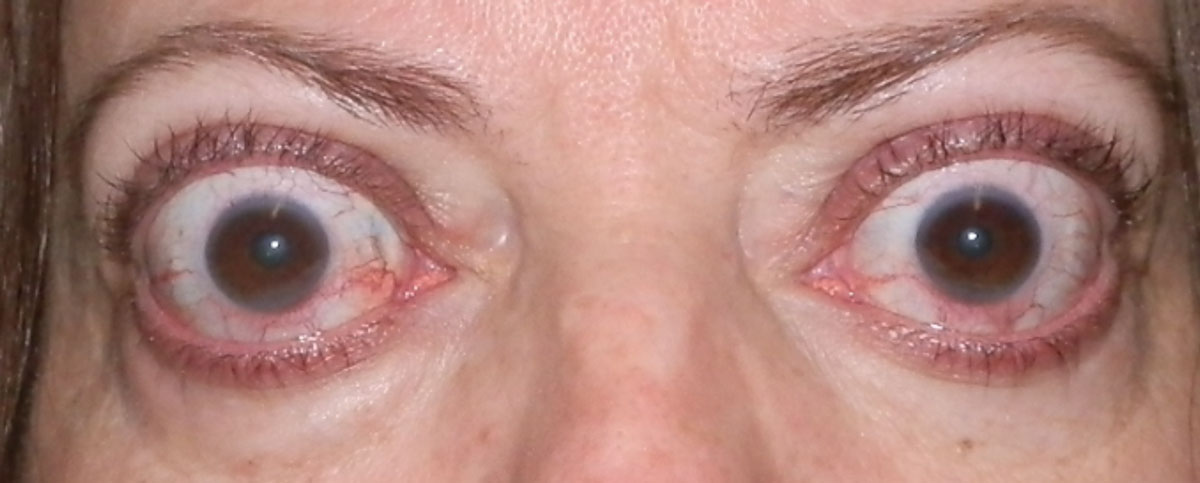
Patients with TED had even lower QoL scores than patients with blindness or uveitis in this study. Photo: Bobby Saenz, OD, MS. Click image to enlarge. |
New research presented in JAMA Ophthalmology sought to help doctors better understand the impact of thyroid eye disease (TED) on quality of life (QoL). Characterized by varying degrees of proptosis and diplopia, TED results in visual changes and potential disfigurement and disability.
The study authors wanted to validate the health states of patients with this disease in moderate to severe cases. To do so, they used six health states of varying severity along with a QoL questionnaire and distributed it to a general population to value health states in TED. A general population was used because, unlike patients with thyroid eye disease, they are not invested in the disease and prevent bias from patients adapting to their health state over time.
Out of the 111 participants with the condition who completed the time trade-off interviews, the mean utility value was 0.44, which is relatively low on a scale from zero to one indicating quality of life. The lowest, or worst score, was seen in the severest disease state (constant diplopia and large proptosis) at 0.30. This was followed by constant diplopia and small proptosis with a score of 0.34, and other disease states increased in score as they were classified as less severe. The highest scoring state was no diplopia and small proptosis with a score of 0.60. In general, values worsened as diplopia became more severe.
All this suggests patients with active, moderate to severe thyroid eye disease may have disutility brought on with increased severity of proptosis and diplopia. The researchers highlight that this shockingly low score is comparable or worse than other debilitating conditions like blindness without light perception, noninfectious uveitis and AMD. The authors of the study specifically note that “this congruence highlights the severe burden moderate-severe active TED places on patients as perceived by an unbiased unaffected population.”1
Despite the concerning results, the authors of the study are hopeful that “these data might now serve as baseline for prospectively assessing improvements (utility gains) with therapies”1
In an invited commentary on the article, also published by JAMA Ophthalmology, one author additionally places importance on the way in which utility values are derived from general vs. patient populations.
As these values can be quite different, the author of the commentary explains that this could be due to respondents with poor health having difficulty imagining full health, a response shift where individuals adapt their standards for assessing their health as it changes or adaption by patients over time to the disease.
The commentary also discusses that the time trade-off method used can pose additional problems, like requiring guidance from interviewers, leading to interference effects. The biggest potential issue is that time trade-off theoretically only produces values, not utilities, because uncertainty and risk are not involved when determining the measurements.
The author does not dismiss the study, though only tries to put it into the greater context of still needing to develop better methods when conducting this kind of research. The commentator believes, in line with the authors of the study, that “the low values reported by the authors of this important study demonstrate that quality of life for patients with TED, especially those with more severe forms of the disease, is probably a lot poorer than we might have thought.”2
1. Smith TJ, Cockerham K, Lelli G, et al. Utility assessment of moderate to severe thyroid eye disease health states. JAMA Ophthalmol. December 29, 2022. [Epub ahead of print]. |

