Editor's note: This article is out of date. Readers may be interested in a more recent article on the topic from March 2021.
 Many patients present for routine eye care with nonspecific
complaints of ocular discomfort. By examining the lid margin and tarsal plate,
you may often explain or identify the root cause of a patient’s comfort issues.
Meibomian gland dysfunction (MGD) can lead to inflammation
of the meibomian glands (meibomianitis) and excess oil in the tear film.
Bacteria and other substances often accompany the oil, which causes a myriad of
ocular surface complaints and signs.
Here, we review the common causes of and treatments for
meibomian gland dysfunction to help you to diagnose and treat this common
condition.
Many patients present for routine eye care with nonspecific
complaints of ocular discomfort. By examining the lid margin and tarsal plate,
you may often explain or identify the root cause of a patient’s comfort issues.
Meibomian gland dysfunction (MGD) can lead to inflammation
of the meibomian glands (meibomianitis) and excess oil in the tear film.
Bacteria and other substances often accompany the oil, which causes a myriad of
ocular surface complaints and signs.
Here, we review the common causes of and treatments for
meibomian gland dysfunction to help you to diagnose and treat this common
condition.
 |
| On this patient’s superior eyelid, dilated and inspissated
meibomian glands are visible—note the multiple glands that are affected
(above). Large, isolated inspissated glands and thickened lid margins are
apparent.
|
Meibomian glands are modified sebaceous glands that are arranged vertically within the tarsal plate. The interactive force of an eyelid blink causes meibum to be excreted onto the posterior lid margin. This oil protects the eyelids from maceration and creates a seal when the eyes are closed. As meibum interacts with the tear film, it reduces surface tension and enhances the tears by spreading them evenly, creating a smooth refractive surface and maintaining a consistent quality of vision. In a patient with MGD, vision is affected because there is too much or too little oil in the tear film. This imbalance causes tear film instability, reduced tear film break-up time (TBUT) and evaporative dry eye.
Meibomian Gland Dysfunction
MGD, also termed posterior blepharitis, is the most common form of lid margin disease (LMD); nearly 40% of routine eye care patients and 50% of contact lens wearers are affected.1,2 In the early stages, patients are often asymptomatic, but if left unmanaged, MGD will either cause or exacerbate dry eye-like symptoms. Dryness, burning, itching, stickiness, foreign body sensation, watering, photophobia and intermittent blurred vision are frequently seen in cases of MGD.
Meibomian gland dysfunction can exist alone, or it can be associated with anterior blepharitis or seborrheic dermatitis.
• Primary meibomianitis. Also known as obstructive MGD, primary meibomianitis is a generalized dysfunction of the sebaceous glands. It is commonly associated with acne rosacea, acne vulgaris and seborrheic dermatitis. The anterior lid margin typically appears normal in those with primary meibomianitis, but the meibomian glands are dilated and blocked with inspissated secretions that are sluggish or stagnant upon expression.
• Anterior blepharitis. This can lead to secondary inflammation of adjacent meibomian glands. In addition to the typical signs of anterior blepharitis, focal patches of inflamed or plugged meibomian glands are evident. It is unclear if bacteria cause the glands’ secretions to become thickened (i.e., inspissated), or if they simply exacerbate the condition by causing inflammation. But, it is known that gram-positive bacteria, such as S. epidermidis and S. aureus, release lipases that hydrolyze sebaceous gland lipids. These enzymes produce free fatty acids and other byproducts that irritate the eyes and cause tear film instability.3
• Seborrheic dermatitis. Patients with seborrheic dermatitis (a skin condition that affects the sebaceous glands of the scalp, face and/or trunk) often have greasy flakes in the lashes and inflamed or infected lid margins. These patients may simply have increased meibomian secretions, or meibomian seborrhea. Along with the greasy scales seen in the lashes, excess meibomian oil is usually evident on the lid margins and in the pre-corneal tear film. The meibomian glands are dilated and full of meibum that can be easily expressed. Frequently, soapy-looking bubbles are seen along the inferior lid margin. This saponification occurs when excess lipid secretions react with protein in the tears. It’s not surprising that patients with meibomian seborrhea frequently complain of burning upon awakening—it’s like getting soap in their eyes! Inflammation is usually minimal in cases of meibomian seborrhea, so patient symptoms are often worse than observed signs. The localized inflammatory response that results from meibomian stasis can lead to permanent keratinization and scarification of the gland. Such an advanced condition affects the lid margin contour and gland placement. Due to a lack of oil in the tear film, these patients typically have a reduced TBUT and increased evaporative rates.
Early Signs of MGD
Do not dismiss the subtle signs of early MGD. Look for oily lid margins, excess oil in the tear film, dilated meibomian glands, mild injection and the occasional inspissated gland. Even if patients are asymptomatic, it’s not too early to start educating them about lid hygiene, the chronicity of the condition, and possible sequelae if left untreated. In cases of longstanding disease, signs include thickened (tylotic) eyelid margins, telangiectatic vessels, loss of lashes (madarosis), poliosis, trichiasis and notching of the lid margin. Chronically inspissated glands eventually become keratinized and “drop out,” leaving a divot in the lid margin. This causes a shift in the meibomian glands, and they become unable to secrete oil onto the proper location of the lid, which results in permanent changes in the tear film composition and ocular environment, and significant dry eye symptoms.
| Kits for Ocular Hygiene and Therapy
Kits that combine oral tetracyclines and lid hygiene products are now available by prescription. Packaging these products together should help patients understand that lid hygiene and oral antibiotics together are important for management. • The Cleeravue-M Kit (StoneBridge Pharma) combines a regimen of 50mg of minocycline with SteriLid. • The Alodox Convenience Kit combines a 20mg regimen of Alodox (doxycycline hyclate) with OcuSoft Lid Scrub pads for acute treatment and OcuSoft Lid Scrub Original Foaming Formula for maintenance. It also includes Tranquileyes Moist Heat Therapy Goggles. |
A happy patient who sees well is the goal of any eye care professional. In MGD patients, the reduction of symptoms is important, and the prevention of permanent damage that can affect the eye’s ability to maintain a balanced environment is paramount. Many effective treatments for MGD are available, so therapeutic care can be tailored to each patient. Patients should be made and kept aware of the signs and symptoms of meibomian gland dysfunction. They need to understand that MGD is a chronic condition and that it requires a regular, if not daily, lid hygiene regimen.
Treatment should incorporate lid hygiene techniques with expression, if possible. Reserve medications for acute or recalcitrant cases. Omega fatty acids found in fish oils and flaxseed are also commonly recommended to patients with dry eye and/or MGD.4 Because of the common comorbidity of MGD and dry eye, pa-tients are often on dry eye therapy while on MGD treatment. Prescribing Restasis (cyclosporine 0.05%, Allergan) may be especially beneficial for those who suffer from aqueous deficient or inflammatory dry eye. A recent study found that dry eye patients on Restasis had fewer meibomian gland inclusions and less lid margin injection.5 Restasis is also especially effective in those with acne rosacea and meibomian gland dysfunction.6 As with any chronic disease, continued compliance is a challenge for patients and doctors alike. Luckily, most of the following treatments are not difficult to perform or explain.
• Warm compresses. A study out of Oxford University found that heating the lids about 9ºF significantly increased meibomian oil production.7 Using warm compresses, heat should be applied to the eyes for two to 10 minutes. This warms the meibum, allowing it to flow more freely, and helps soften lash debris. May recommend patients perform compress therapy with a wet washcloth towards the end of a hot shower. This should encourage compliance by helping incorporate lid hygiene into the daily routine—may also enhance the therapeutic effect since meibomian glands and skin pores open in a hot shower. Other warm compresses are a microwaved sock filled with dry rice, hot hard-boiled eggs in a damp sock, and gel-filled masks. After the application of warm compresses, patients with all forms of posterior blepharitis should massage their lids to help express meibum from deep within the glands.
• Lid scrubs. These help to remove oil, bacteria and debris, as well as to stimulate the meibomian glands. Baby shampoo or mild soap have historically been recommended to patients with seborrheic forms of lid disease. Note that some patient’s eyes are sensitive and become chemotic and injected due to the detergent. OcuSoft (OcuSoft) and SteriLid (Advanced Vision Research) are bactericidal products available commercially. These products may be less irritating to the conjunctiva than shampoo or soap. Lid scrubs may be prescribed at different steps within the lid hygiene regimen. In patients with anterior blepharitis, lid scrubs should be performed before massage so the lashes are cleared of bacteria and debris prior. In patients with posterior blepharitis, one may opt to first express meibum from deep within the lids, then perform lid scrubs to remove excess oil.
• Massage. Lid massage can dramatically improve symptoms by helping re-establish tear film stability. Research has demonstrated that, after gland expression, TBUTs return to normal, and in some cases, super-normal levels.8 The technique: Extend finger and apply light pressure. Roll the finger upward on the lower lid two times while in upgaze, then roll the finger downward on the upper lid two times while in downgaze. Excessive manipulation of the lids can cause additional irritation, so lid massage and scrubs should be performed twice a day during the acute stage, and once daily during maintenance. Follow-up care is important in these cases, so that treatments can be assessed and modified. After regular lid hygiene, have patients instill an artificial tear. This helps to rinse away the extra oil from gland expression and/or any residue from the lid scrub. MGD patients also typically have dry eye, so tears are often recommended between two and four times per day.
• Tetracycline. For ongoing management of MGD, tetracyclines are effective and useful. Oral tetracyclines—e.g., doxycycline and minocycline—appear to inhibit bacterial lipase production. This reduces free fatty acids, which helps to lessen inflammation and symptoms of irritation. Tetracyclines also help inhibit keratinization of the meibomian glands, and have been shown to reduce the number of Staphylococcus organisms.9,10 Ocular hygiene kits that package tetracyclines and hygiene tools together for patients are now available for prescription. The current modality is to decrease doxycycline dosage from the typical dose (100mg b.i.d.) to 20mg to 50mg b.i.d. for a two-month course. In a study comparing low- vs. high-dose doxycycline, patient symptoms were equally improved in both dosage groups.11 Side effects can be kept at a minimum with a decreased dose of doxycycline. Minocycline can be considered as well, because it already carries a lower dosage (50mg), once-a-day treatment, and few side effects (particularly with regards to sun exposure). Patients may be kept on a maintenance dose as long as necessary.
| In-Office Expression of Meibomian Glands
In-office expression of the meibomian glands can provide significant relief because the backed-up glands can be painful. To express the meibomian glands, instill topical anesthetic and apply pressure between two cotton-tipped applicators in an upwards-rolling motion (one applicator on either side of the eyelid). Alternatively, use a Mastrota paddle (OCuSOFT), developed by Katherine Mastrota, O.D., which is used specifically for expressing the meibomian glands. Upon expression, the secretions may be thickened, and they may appear cheesy or toothpaste-like. A topical antibiotic/steroid may be prescribed to reduce inflammation after manual expression. As prophylaxis post-expression, one may choose to prescribe any of a variety of generic antibiotic ointments, like bacitracin or erthythromycin. |
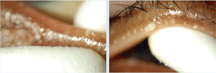 |
| The pressure of two cotton-tipped applicators will express
the meibomian glands. Upon expression, not only are nearly all glands stagnant,
but dry and scaly material (i.e., scurfs) is also found in the lashes.
|
The latest trend in the treatment of MGD is the use of the topical antibiotic AzaSite (azithromycin 1%, Inspire Pharmaceuticals). AzaSite is gel-forming and lipophilic. It remains on the ocular surface longer than conventional drops do, which allows for an increased drug concentration in the eyelid and conjunctival tissue. Like other macrolides, azithromycin has an anti-inflammatory effect. AzaSite is prescribed off-label to help control posterior blepharitis—it is thought to expedite resolution of gland inflammation.12 Patients may instill one drop after lid hygiene at bedtime and rub the solution into their lashes. They follow this routine for two to four weeks and are closely monitored. Another potential treatment option for MGD is to begin a regimen of nutraceuticals. A growing body of evidence links the dietary intake of omega fatty acids with benefits for patients with dry eye conditions and MGD.13,14 This family of essential fatty acids provides the building blocks for the prostaglandins that modulate tissue inflammation. Because of the benefit to vascular, cardiac and other physiologic functions, most clinicians suggest 2g to 3g per day of high-quality OTC fish oil capsules or flaxseed. Lovaza (GlaxoSmithKline) is a 4g dose of super-purified omega-3 fatty acid ethyl esters that is currently available by prescription.
If patients are educated about eyelid hygiene early in the course of the disease, it is possible to prevent advanced signs. For milder cases, lid hygiene alone may be enough to prevent symptoms. For patients who are symptomatic, a variety of therapeutic options may be used in combination with hygiene techniques. It is especially important to incorporate eyelid massage into the hygiene regimen; this helps keep the oil flowing from the meibomian glands and can improve symptoms quickly. Manual manipulation of the lid is critical for a successful outcome. Ultimately, we want to keep patients comfortable. The challenge for any clinician managing a case of MGD is to offer patients a practical solution that is not overly cumbersome and affords a reasonable chance at continued compliance. Dr. Pitts is a Southern College of Optometry graduate and Clinical Instructor. She works in the Ocular Disease and Primary Care clinics at The Eye Center, and she is a regular attending staff doctor with the Student Volunteer Optometric Services to Humanity. Dr. Lievens is an Associate Professor and the Chief of Primary Care at the Southern College of Optometry. He is also the Interim Chief of Staff of The Eye Center. Dr. Lievens is the co-creator of the funduscopic grading card.
1. Hom MM, Martinson JR, Knapp LL, Paugh JR. Prevalence of meibomian gland dysfunction. Optom Vis Sci. 1990 Sep;67(9):710-2.
2. Henriquez AS, Korb DR. Meibomian glands and contact lens wear. Br J Ophthalmol. 1981 Feb;65(2):108-11.
3. McCulley JP, Shine WE. Changing concepts in the diagnosis and management of blepharitis. Cornea. 2000 Sep;19(5):650-8.
4. Paranjpe DR, Foulks GN. Therapy for meibomian gland disease. Ophthalmol Clin North Am. 2003 Mar;16(1):37-42.
5. Perry HD, Donnenfeld ED. Topical 0.05% cyclosporine in the treatment of dry eye. Expert Opin Pharmacother. 2004 Oct;5(10):2099-107.
6. Schechter BA, Katz RS, Friedman LS. Efficacy of topical cyclosporine for the treatment of ocular rosacea. Adv Ther. 2009 Jun;26(6):651-9.
7. Nagymihalyi A, Dikstein S, Tiffany JM. The influence of eyelid temperature on the delivery of meibomian oil. Exp Eye Res. 2004 Mar;78 (3):367-70.
8. McCulley JP, Sciallis GF. Meibomian keratoconjunctivitis. Am J Ophthalmol. 1977 Dec;84(6):788-93.
9. Marks R, Davies MJ. The distribution in the skin of systemically administered tetracycline. Br J Dermatol. 1969 Jun;81(6):448-51.
10. McCulley J. A combination therapy for blepharitis and meibomianitis. Ophthalmol Manage. 2006 Sept. Available at: www.ophmanagement.com/article.aspx?article=86674 (Accessed May 2009).
11. Yoo SE, Lee DC, Chang MH. The effect of low-dose doxycycline therapy in chronic meibomian gland dysfunction. Korean J Ophthalmol. 2005 Dec;19(4):258-63.
12. Ianaro A, Ialenti A, Maffia P, et al. Anti-inflammatory activity of macrolide antibiotics. J Pharmacol Exp Ther. 2000 Jan;292(1):156-63.
13. Sullivan BD, Cermak JM, Sullivan RM, et al. Correlations between nutrient intake and the polar lipid profiles of meibomian gland secretions in women with Sjögren’s syndrome. Adv Exp Med Biol. 2002;506(Pt A):441-7.
14. Boerner CF. Dry eye successfully treated with oral flaxseed oil. Ocular Surgery News. 2000;10:147-8.

