 |
|
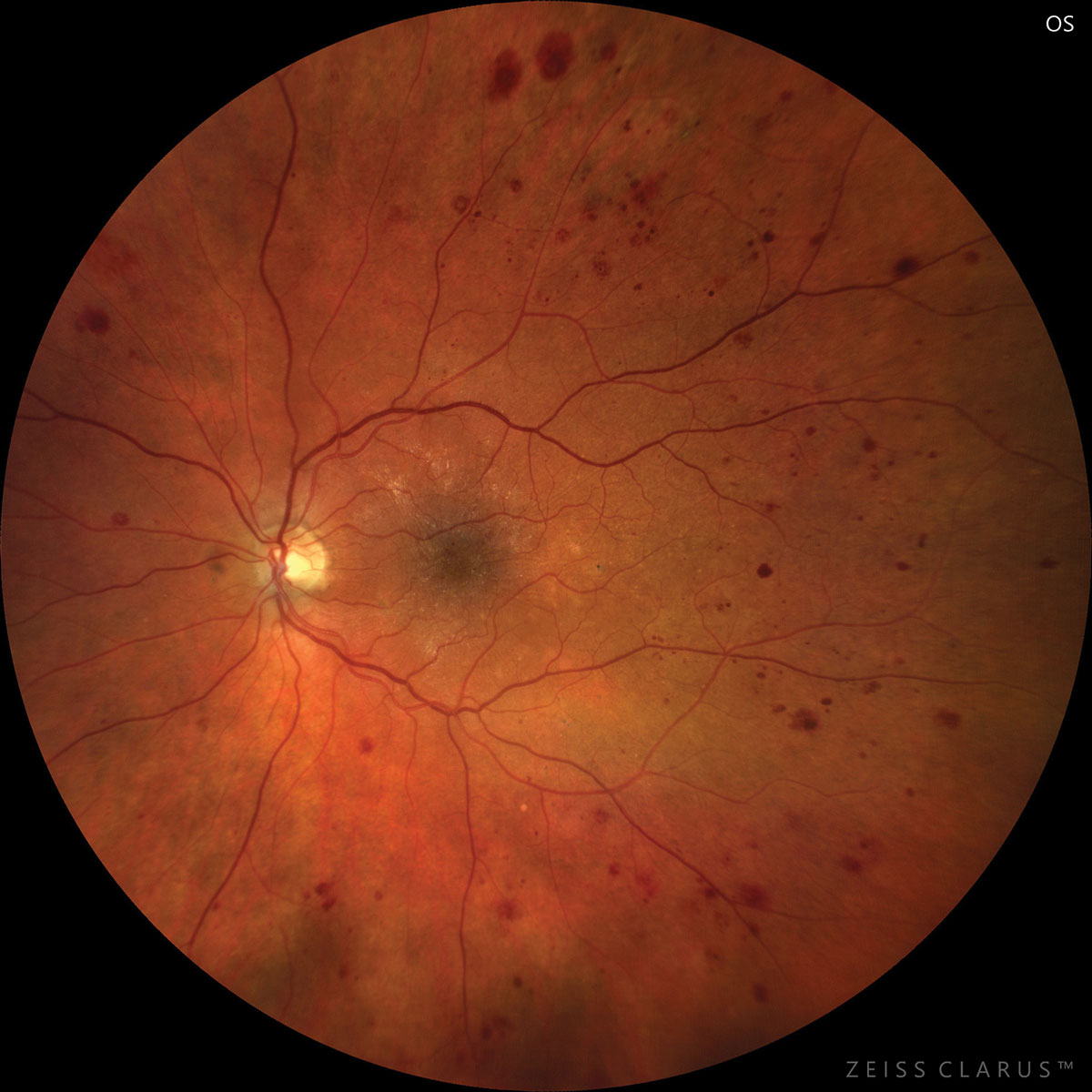
Improvement in microaneurysms is one clinical indicator of successful response to therapy for diabetic retinopathy, the study found. Photo: Jay Haynie, OD . Click image to enlarge. |
A new retrospective study analyzing Korean patients with diabetic eye disease looked at those who underwent therapy of intravitreal bevacizumab or panretinal photocoagulation (PRP). A total of 320 patients with diabetic retinopathy (DR) were included and were treated with either or both options. To compare the number of microaneurysms and area of capillary non-perfusion, two consecutive fluorescein angiographies (FAs) of each eye of the patient were performed and subsequently calculated with software. FA baselines and changes in the ocular and systemic factors were also analyzed.
The researchers defined microvascular recovery as “a marked reduction in the numbers of microaneurysms (<20%) or a marked reduction in the area of capillary non-perfusion (<50%) in 45-degree fields or a complete regression of new vessels in ETDRS 7 standard fields.”
Out of the 320 total eyes, only 8.8% (28 eyes) met microvascular recovery criteria after completed treatment. The follow-up period revealed that diffuse capillary telangiectasia and late disc leaking found on baseline FA, as well as glycated hemoglobin reduction were all predictive characteristics of microvascular recovery.
The researchers’ proposed explanation for these findings: an instance of telangiectasia may indicate recent VEGF upregulation and this could be neutralized by timely inhibition of VEGF. As for late disc leaking, the researchers consider that this could be classified as evidence of diabetic papillopathy, which can effectively regress after IVB.
The last finding the researchers sought to elaborate upon is glycated hemoglobin reduction. They explain that baseline HbA1c levels were not associated with any microvascular recovery. HbA1c reduction during treatment, however, did substantially predict recovery. The authors of the study do point out that DR worsening has been associated with rapid improvement of diabetic control, but in this study the recovery group only displayed a -0.74% HbA1c level reduction over 12 months. Comparatively, baseline glycemic control did not differ compared with other studies. As such, the researchers proffer that “appropriate diabetic control is the only modifiable factor during the treatment of this study.”
The authors reiterate that their findings are important because diabetic retinopathy can cause vision-threatening complications. As such, “to avoid neuronal dysfunction in diabetes and the risk of visual loss, preventative or regenerative treatments for the microvascular abnormalities are the primary treatments for DR,” they observed in their paper on the work. By identifying the common indications of microvascular improvement, further research may build on this to identify why and help those who do not exhibit these findings.
Lee J, Kim YJ, Lee JY, Yoon YH, Kim JG. Predictive factors for microvascular recovery after treatments for diabetic retinopathy. BMC Ophthalmol. 2023. [Epub ahead of print]. |

