 |
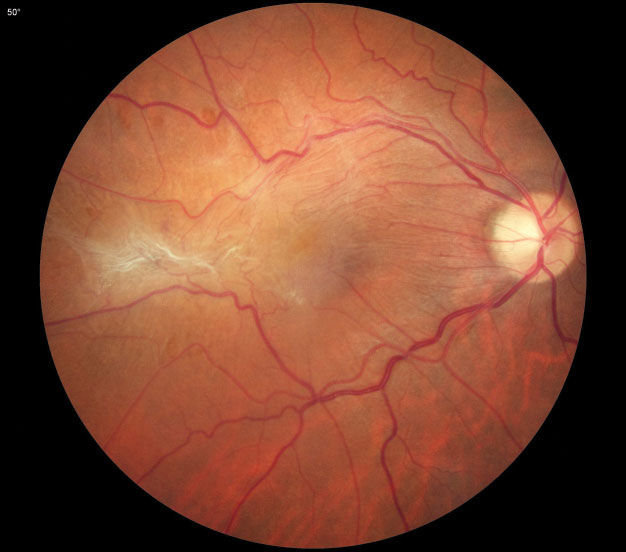
The presence and progression of pathological lesions in the macula, such as the ERM seen here, greatly affect patients’ visual function. Photo: Diana Shechtman, OD. Click image to enlarge. |
With increased axial length (AL), vision-threatening structural changes are more likely to occur in the posterior pole of the highly myopic eyeball, including posterior staphyloma, epiretinal traction and retinal stretching. These changes can lead to a series of pathological lesions in the macula, such as epiretinal membrane (ERM), myopic retinoschisis and macular hole, known collectively as myopic tractional maculopathy, one of the most common and vision-threatening complications associated with high myopia. Its progression may influence the visual function of highly myopic patients, but few studies have consistently tracked it. A recent analysis, published in Retina, demonstrated in highly myopic patients that long-term visual acuity of eyes with ERM was relatively stable but significantly affected by progression of myopic retinoschisis and macular hole.
Researchers in China assessed 610 highly myopic eyes (AL ≥26mm) of 610 patients 18 and older. All participants underwent detailed ophthalmic examinations at enrollment and at the two-year follow-up or anytime they received vitreoretinal surgery within the two years, which included best-corrected visual acuity (BCVA), slit lamp, fundoscopy and OCT scans.
The prevalence of ERM, myopic retinoschisis and macular hole increased from 26.7%, 12.1% and 4.4% at enrollment to 41.1%, 18.2% and 9.5% at the two-year follow-up, respectively. ERM progressed in 21.8% of eyes, but visual acuity did not decline significantly in these eyes. Myopic retinoschisis progressed in 6.8% of eyes, and macular hole progressed in 14.8% of eyes. The researchers detected significantly greater BCVA reduction in the eyes with myopic retinoschisis or macular hole progression than the rest. Multivariate analysis showed longer AL, more severe posterior staphyloma and absence of dome-shaped macula were associated with myopic tractional maculopathy progression.
ERM, myopic retinoschisis and macular hole progression were all related to a lower rate of dome-shaped macula. Logistic regression analyses showed the absence of dome-shaped macula increased the risk of ERM progression by 1.8-fold, myopic retinoschisis progression by 7.6-fold and macular hole progression by 5.6-fold.
“A possible explanation may be that dome-shaped macula, acting as a macular buckle, alleviates tractional forces over the fovea,” the researchers wrote in their paper. “The influence of macular atrophy and choroidal neovascularization on myopic tractional maculopathy were not investigated in this study, but future studies with these complications included are also needed.”
Meng J, Chen Y, Cheng K, et al. Long-term progression pattern of myopic tractional maculopathy: outcomes and risk factors. Retina. March 27, 2023. [Epub ahead of print]. |

