 |
Q:
I have an 11-year-old patient with refractory severe vernal keratoconjunctivitis (VKC) and significant corneal staining, mostly in the left eye. I tried the typical topical agents such as low-dose steroids and mast-cell stabilizer/antihistamine drops. There is no shield ulcer yet, but I’m concerned it might happen. Are there any heroic options for this case?
A:
“VKC is a chronic issue, typically lasting several years with seasonal exacerbation,” says Aaron Bronner, OD, of Pacific Cataract and Laser Institute. “That means even the most effective treatment regimen possible won’t truly eradicate it, though it will burn out eventually.” Also, it most typically occurs in children and adolescents, “which raises the stakes for both permanent sequelae of the disease, such a corneal scarring, and treatment, such as steroid-induced cataract development or increased intraocular pressure.”
At its root, the condition is an inflammatory and allergic process, so reducing the inflammatory response is important. However, concerns about inconveniencing the patient or risk of treatment sequelae can get in the way of this step.
“In this case, the clinician treating the patient has raised concerns with potential for a shield ulcer, a problem that can cause permanent reduction in vision, should it develop,” says Dr. Bronner. “This risk should trump any concerns over patient inconvenience or treatment sequelae risk. There is potential for the VKC to present a direct threat to vision, and that threat needs to be eliminated.”
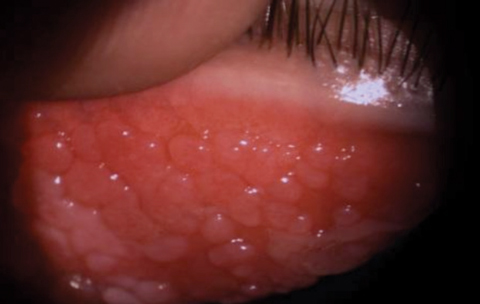 |
| VKC requires careful long-term therapy. Photo: M.S. McMeekin, OD |
What Next?
Since a weaker steroid has already failed in this case, Dr. Bronner recommends a high-dose, high-potency corticosteroid such as Durezol (difluprednate, Novartis). Aggressive dosing is imperative to eliminate the inflammation. “Though there is a greater risk of steroid-related side effects with difluprednate compared with weaker steroids (especially in the juvenile population), its dosing duration should be short,” says Dr. Bronner, “just long enough to control inflammation acutely before transitioning to the longer-term therapy with weaker steroids and antihistamine/mast-cell stabilizers. If a shield ulcer has already formed, the acute steroid therapy should be paired with an antibiotic.”
Next up is what Dr. Bronner calls the long-term goal: keeping exacerbations as infrequent and as mild as possible. To do this, ODs should rapidly taper the steroid and move to a combination of the lowest dose and weakest steroid that maintains control. Mast-cell stabilizers/antihistamines should also be added to this treatment. “While short dosing of steroids is safe and effective, we know that the risk of cataracts and ocular hypertension rises with increased duration and frequency of steroid use,” says Dr. Bronner. “Ideally, these patients will be tapered off of steroids for all periods other than acute flare-ups.”
If the patient experiences a flare-up each time the steroid is reduced or eliminated, consider steroid-sparing therapies. “Compounded topical cyclcosporin A or tacrolimus have been shown to be effective at diminishing both signs and symptoms of VKC. However, keep in mind that stringent regulations have made it more difficult to find pharmacies to compound ophthalmic agents,” says Dr. Bronner, “and there are also expected burdens with cost and insurance coverage.”
Additionally, Dr. Bronner notes that “Restasis (cyclosporine 0.05%, Allergan) is generally too weak to be effective for cases of VKC.”
Xiidra (lifitegrast, Shire) could be considered as an off-label, adjunctive treatment because “intercellular adhesion molecule-1 has also been shown to be upregulated in VKC,” Dr. Bronner says.
“Though there are no clinical reports of Xiidra for maintenance therapy of VKC, it would likely be a safe approach and one with some scientific rationale; barring success with other, more standard therapy, I wouldn’t hesitate to try it after counseling the patient appropriately.”

