 |
History
A 55-year-old Caucasian male presented to our office urgently with a chief complaint of a foreign body sensation in his right eye for a duration of two hours.
The patient explained that, before calling the office, he tried cold compresses and artificial tears, but could not find relief. He denied toxic exposure, trauma of any kind and any allergies.
His history was positive for systemic hypertension and hypercholesterolemia, for which he was medicated and compliant.
Diagnostic Data
His best-corrected entering visual acuities were 20/20 OU at distance and near. His external examination was normal, although there seemed to be mild excessive lacrimation in the left eye without conjunctival injection.
We observed no evidence of afferent pupil defect. The pertinent biomicroscopic examination of the anterior segment is demonstrated in the photograph. Goldmann applanation tonometry measured 15mm Hg OU. The dilated fundus findings were normal peripherally and centrally with normal nerves and maculae.
Your Diagnosis
Does the case presented require any additional tests, history or information? What steps would you take to manage this patient? Based on the information provided, what would be your diagnosis? What is the most likely prognosis?
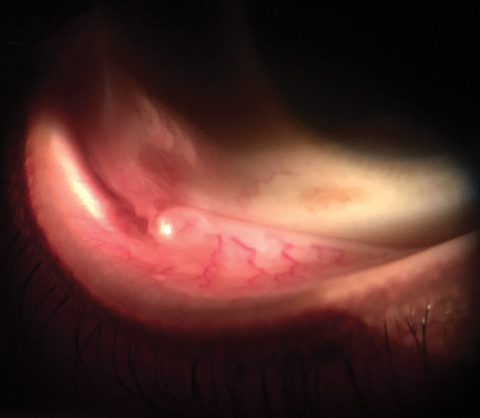 |
| A 55-year-old patient presented urgently with a foreign body sensation in his right eye. Can this image help explain his issue? Click image to enlarge. |
Additional studies included examination of the eyelids for their ability to close, examination of the Bell’s reflex and its ability to cover the cornea when employed, sodium fluorescein instillation to assess for corneal and conjunctival compromise and corneal sensitivity testing to assess the integrity of tissue’s physiologic response.
Diagnosis and Discussion
The diagnosis in this issue is conjunctival retention/inclusion cyst of the left lower fornix.
Conjunctival cysts may be congenital or acquired.1-6 A conjunctival cyst is a thin-walled sac or vesicle that contains fluid.7 This vesicle may develop either on or under the conjunctiva and are rarely drug induced.7 They are dilated lymphatic channels that fill with fluid after becoming entangled following injury, surgery or injection.1-5 In some cases the process happens surrounding a gland of Krause.6 Acquired cysts occur when conjunctival cells, adjacent to scars after injury or surgeries become reorganized permitting pockets that permit the gathering of extracellular fluid.1-5 Injuries of the conjunctiva and tenon’s fascia, including blunt trauma, toxic exposure, anesthetic or therapeutic injections and eye rubbing can all initiate the process.1-5 Chronic ocular inflammation from allergy, antigen antibody disease (Steven/Johnson [SJS], poly arteritis nodosa) or even dry eye syndrome are other common sources that may set up the conditions for the formation of conjunctival cysts.1
Conjunctival surface inflammation of any kind has the potential to induce tissue adhesions between the tarsal and bulbar conjunctival surfaces. This process causes the manipulation of the conjunctival epithelium, allowing it to roll secondary to the stressors of eye movements or blinking. As lymphatic channels become trapped and or kinked the fluid they contain, along with any new fluid produced becomes entrapped in the tissue pocket. These lesions are commonly referred to clinically as “retention cysts”.1
In the case of chronic inflammatory disease such as SJS, extensive surface denudation and the induction of inflammatory cells lead to conjunctival tissue adhesions (alternative to tissue rolling), which lead to cyst formation.
The cysts themselves are vulnerable to replication (having more added), complications (lobulation) or enlargement when they are frictionally broken either by accident (eyelid rubbing) or on purpose via procedures like glass rod insertion.1 The presence of fallen and entrapped cilia and concretions (hair, dust and debris) can also promote cyst formation.1
Fornix cysts are not a cosmetic issue, however, cysts on the bulbar conjunctiva maybe. Larger ones can act like space-occupying lesions, restricting ocular motility or interfereing with ocular surface homeostasis.1
In this instance, since conservative treatment (cold compress and lubrication) did not alleviate the symptoms of foreign body sensation and lacrimation, needling was performed. Here, the eye is made numb with a topical anesthetic. A drop of topical antibiotic is instilled to reduce the risk of infection and a sterile 30 gauge needle on a tuberculin syringe (for extended reach) is used to create multiple holes in the redundant and sequestered conjunctiva. These lesions do no rupture like a water balloon, rather, they leak over time flattening out over hours. Care should be taken so as to not cause extensive subconjunctival hemorrhage. After the procedure, another drop of topical antibiotic can be instilled.1-5 In the event this does not work or in the event additional tissue roll or redundancy does not allow for the lesion to evacuate, a larger more distinct tissue opening can be created with a Wescott scissor.3
Surgical interventions like excision and marsupialization are suggested for larger cysts.1
The patient underwent uneventful needling of the small lesion and left the office feeling better. They have not returned indicating there has been no recurrence.
1. Singh G, Rajaraman R, Raghavan A, Palanisamy M. Bilateral conjunctival retention cysts in the aftermath of Stevens-Johnson syndrome. Indian J Ophthalmol. 2008;56(1):70-2. |

