 |
A 55-year-old man presented urgently after being struck in the right eye. Playing wiffleball with his son the day before, the patient took a direct, high-speed hit to his right globe. He noted no pain to the eye initially, but some discomfort to the periorbital region with associated bruising. He did note that his vision was immediately blurry, but waited to seek medical care, expecting that “it would clear up.”
Examination
He felt that his vision did improve and he presented with acuity of 20/25 in the eye. His right pupil was mid-dilated and unreactive to light and accommodation. He had moderate conjunctival injection in his right eye and a moderately heavy anterior chamber reaction with both white and red blood cells. He also had a mild accumulated hyphema. Gonioscopy was deferred due to the recent nature of the trauma. His intraocular pressure (IOP) was 15mm Hg in the right eye and 12mm Hg in the left. His crystalline lens was clear and centered and a dilated fundus exam showed no abnormalities.
 |
| After his son confused the meaning of “keep your eye on the ball,” this dad’s traumatic ocular injury developed into uveitis and hyphema. |
Diagnosis
He was diagnosed with a traumatic uveitis and hyphema, as well as a tonic pupil due to iris sphincter damage. He was cyclopleged with atropine 1% BID and treated with difluprednate 0.05% (Durezol, Alcon) QID. He was instructed to relax and stay in bed as much as possible. By the next day, his vision improved to 20/20 and his anterior chamber reaction was greatly diminished with near-complete resolution of hyphema. Medications were tapered accordingly over the ensuing week and the patient had a great outcome, though he has a small degree of angle recession and a permanently dilated pupil from the iris sphincter tear.
Discussion
Hyphema is accumulated blood in the anterior chamber (AC).1-4 The presence of non-layered red blood cells circulating in the anterior chamber is referred to as microhyphema. Hyphema can occur as a result of:
- Blunt or lacerating ocular or adnexal trauma
- Following intraocular surgery
- Secondary to conditions that induce iris neovascularization, such as diabetes
- Venous occlusion or iris melanomaSecondary systemic conditions, such as juvenile xanthogranuloma or myotonic dystrophy
- As a complication of keratouveitis (e.g., herpes zoster)
- As a complication of other blood disorders such as leukemia, hemophilia, von Willebrand disease and in association with the use of substances that alter platelet or thrombin function (e.g., ethanol, aspirin, warfarin).1-3
Complications of traumatic hyphema include increased IOP with secondary glaucoma,
peripheral anterior synechiae, decreased visual acuity and corneal dysfunction (blood being in the AC and corneal blood staining) and rebleeding with secondary hemorrhaging.1-3
Patients may present with the classic signs and symptoms of associated uveitis, including conjunctival hyperemia, blurred vision, eye and orbital pain, photophobia, lacrimation and blepharospam as well as blood in the AC.1-3 Any time IOP is elevated following blunt traumatic ocular injury, hyphema should be suspected whether blood is visible in the anterior chamber or not. The most common concurrent ocular injuries associated with traumatic hyphema is corneal injury and uveitis; however, adnexa ecchymosis and lacerations of the eyelid are also possible.4-6
Hyphemas are classically graded by the amount of visible blood occupying the AC. Less than 33% of the AC is grade 1, 33% to 50% is grade 2 and greater than 50%, but less than 100%, is grade 3. Complete AC filling is grade 4. The term “8-ball hemorrhage” connotes complete filling of the AC with blood, appearing black like a billiard 8-ball.
There are two postulated mechanisms regarding traumatic hyphema formation. Either direct, concussive forces cause mechanical tearing of the fragile vasculature of the iris or angle, or concussive trauma creates rapidly rising intravascular pressure within these vessels, resulting in their rupture.6 The most common traumatic cause of hyphema is a tear in the anterior face of the ciliary body.
A minor quantity of blood in the AC is not, by itself, necessarily harmful to the ocular environment. However, when quantities are sufficient, macrophages ingest the hemoglobin from the lysed red blood cells. These hemoglobin-laden macrophages obstruct the outflow of aqueous humor by physically blocking access to the drainage area, resulting in IOP rise.7 This is known as hemolytic glaucoma.7
Patients with the sickle trait have a greater risk for elevated IOP.8 Sickled red blood cells are not as malleable as normal red blood cells. Hyphema involving any sickled cells further impedes the flow of aqueous humor, slowing both aqueous and oxygen transfer. The hypoxic environment encourages red blood cells encoded with the sickle trait to undergo the sickle transformation, which further obstructs aqueous outflow.8
Circumstances surrounding the event and current medicines are important pieces of data. Bleeding in the eye warrants concern for systemic blood disorders such as antiphospholipid antibody disease (protein S and protein C), hyperhomocysteinemia, dysfunction of the clotting factors, sickle cell anemia, hemophilia and von Willebrand’s disease.1,2 Testing for sickle cell anemia is also a consideration.
Ocular examination should include evaluation of the adnexa. Imaging should be ordered when appropriate to rule out fracture or entrapment (x-ray, CT scan).
The cornea should also be evaluated for abrasion, laceration or penetrating injury. A ruptured globe usually includes poor visual acuity, ocular hypotony, and shallowing of the AC.9 The iris should be inspected for iridodialysis and sphincter tears, and the lens for luxation. A dilated fundus exam should be completed to rule out vitreous hemorrhage and retinal tears or detachments. If a clear view of the fundus is obstructed by the hyphema or vitreous hemorrhage, B-scan ultrasonography should be attempted to best assess posterior segment damage.1,2 Eventually, gonioscopy should be performed to look for angle recession. This is typically performed four to six weeks after the initial trauma.
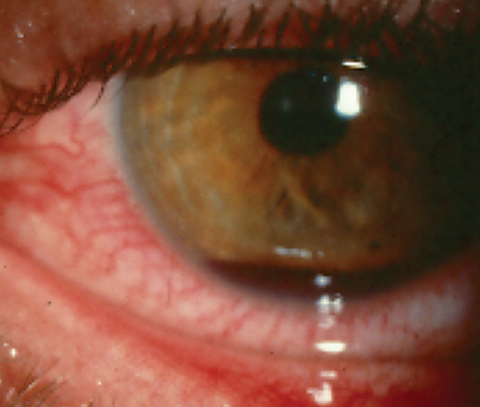 |
| Traumatic hyphema patients may suffer from increased IOP, secondary glaucoma, corneal dysfunction and other compounding factors. |
Treatments
Management of hyphema is directed towards enhancing blood resorption and minimizing complications such as glaucoma and corneal blood-staining. Controversy is ongoing whether these individuals should be managed as in- or out-patients.10 While some advocate strict bed rest and even hospital admission, there is no evidence that outcomes for such measures are better than quiet ambulation. Most practitioners manage microhyphema and uncomplicated grade 1 and 2 hyphema conservatively without hospitalization. Hospitalization is typically reserved for severe hyphema, sickle cell trait/disease, noncompliant patients, children and those with bleeding disorders. Rest with head elevation allows blood to settle inferiorly and prevents clot formation and blood-staining over the visual axis.10 Patients should be instructed to wear a protective shield at all times, especially while sleeping, to prevent inadvertent repeat trauma. Aspirin and nonsteroidal anti-inflammatory medications increase the risk of rebleeding and should not be used if at all possible.10
Although studies have not found cycloplegic usage to affect final visual acuity, their use is considered advantageous by reducing the risk of secondary hemorrhage by immobilizing the iris and ciliary body. Also, their use reduces risk of posterior synechiae, increases uveoscleral outflow and enhances patient comfort.10 Adequate cycloplegia is accomplished using atropine 1%, BID–TID for two weeks, though less frequent dosing may achieve adequate cycloplegia for mild hyphema.
Local inflammation is controlled via topical prednisolone acetate 1%, Q2H-QID or difluprednate 0.05% BID-QID.10 Additionally, they stabilize the blood-ocular barrier and may decrease the frequency of secondary hemorrhage.10 However, in a recent study topical steroids failed to demonstrate any benefit over supportive therapy consisting simply of bed rest, head elevation and hydration.11
If IOP is elevated above 24mm Hg, it can be reduced with the use of topical aqueous suppressants such as an alpha-2 agonist, beta-blocker or carbonic anhydrase inhibitor in standard dosing. When IOP is exceptionally high (greater than 35mm Hg) requiring acute attention, acetazolamide tablets, 500mg (2 x 250mg) BID can be prescribed along with topical aqueous suppressants. Acetazolamide lowers plasma pH, which promotes sickling of red blood cells; thus, methazolamide is preferable in patients with sickling disorders.10 Follow up should be set no later than a week for uncomplicated cases and should be set for consecutive days, as necessary, in cases where there are vision-threatening issues.1,3
Referral for surgical evacuation is indicated in the following cases:
- if there is corneal blood staining;
- if the hyphema fails to reduce to less that 50% of AC volume within eight days;
- if IOP is greater than 60mm Hg for two days;
- if there is an 8-ball hemorrhage;
- if the IOP remains greater than 25mm Hg for five or more days (to prevent blood-staining); or
- if IOP remains greater than 24mm Hg over 24 hours in a patient with a sickling disorder.1-3,10
The most common surgical procedure is limbal paracentesis and blood aspiration. AC washout can be done if the blood has not yet layered.10
The use of oral antifibrinolytic medications such as tranexamic acid tablets have demonstrated superior properties for stabilizing bleeding and maintaining clot performance, reducing the risk for rebleeding and injury worsening.12,13 Topical tranexamic acid is as effective as the oral version in preventing secondary hemorrhage.13
Though hyphema is a common entity, there exists no consensus on management. The use of hospitalization, bed rest, head elevation and use of cycloplegic steroid and antifibrinolytic agents must be decided on a case-by-case basis.
The authors would like to thank Dr. Lindsay Baker-Howse for her contribution of the case and suggestion of topic.
1. Walton W, Von Hagen S, Grigorian R, et al. Management of traumatic hyphema. Surv Ophthalmol. 2002;47(4):297-334. |

