A 43-year-old Hispanic female presented with a chief complaint of reduced near acuity that had persisted for six months. Her last eye exam was several years ago and, at that time, she didn’t require any optical correction. Her medical history was unremarkable. The patient reported a 20-year history of smoking, but added that she quit five years ago.
 |
On examination, entering distance acuities measured 20/20 OU. She read J2 OU at near, and improved to J1+ with +1.25D of correction OU. Extraocular motility testing was normal. Confrontation visual fields were full to careful finger counting OU. The pupils were equally round and strongly reactive, with no evidence of afferent defect in either eye. The anterior segment examination was unremarkable.
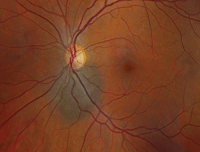
Dilated fundus exam of the right eye was completely normal. The left eye, however, exhibited a clinically significant change (figure 1). So, we obtained a spectral-domain optical coherence tomography (SD-OCT) scan of her left eye (figure 2). The maculae and peripheral retinae were normal in both eyes.
Take the Retina Quiz
1. What is the likely diagnosis?
a. Choroidal nevus.
b. Choroidal melanoma.
c. Melanocytoma.
d. Metastatic carcinoma.
2. What additional testing would be most helpful for this patient?
a. Fluorescein angiogram.
b. Ultrasound.
c. Liver function panel.
d. Chest X-ray.
3. How should this patient be managed?
a. Observation.
b. Enucleation.
c. Plaque radiotherapy.
d. Chemotherapy.
4. What is the estimated likelihood that the lesion will grow over the next five years?
a. Very unlikely.
b. Unlikely––approximately a 25% chance.
c. Likely––approximately a 50% chance.
d. Very likely.
5. What is the overall prognosis for this patient?
a. Very poor.
b. Moderate.
c. Excellent.
d. Unknown.
For answers, see the bottom of the article.
Discussion
The slate gray-colored lesion located adjacent to the optic nerve likely is a choroidal nevus––a benign developmental tumor usually observed as an incidental finding during a routine eye examination.
Ninety-five percent of choroidal nevi will be flat, slate gray in appearance and less than three disc diameters in size.1 They are comprised of benign spindle cells and branched melanocytes. By contrast, most melanomas are usually more than 3.0mm in thickness, can be variably pigmented, and may have overlying orange pigment, which represents lipofuscin––a worrisome finding suggestive of an increased potential for malignancy.
The diagnosis is usually straightforward, with little or no concern that the lesion is a choroidal melanoma. However, that’s not always the case. Occasionally, choroidal nevi can be difficult to distinguish from small malignant melanomas––especially if the lesions aren’t flat, as was the case in our patient. Even though stereoscopic clinical exam didn’t reveal any elevation, we could definitely see that the lesion exhibited some degree of thickness. Indeed, we estimated that the lesion measured 6.0mm x 5.0mm x 1.1mm using both ultrasound and SD-OCT.
Other SD-OCT findings also were quite interesting. We noted retinal pigment epithelium (RPE) irregularity above the lesion, as well as mild anterior bowing secondary to the lesion’s elevation. Further, the scan revealed shallow subretinal fluid located underneath the inferior RPE, which is a risk factor for growth and/or transformation.
|
|
|
1. A fundus photograph of our patient's left eye. Note the lesion located adjacent to the optic nerve.
|
Using the enhanced-depth imaging module on Spectralis OCT (Heidelberg Engineering), we also noted acoustic shadowing within the choroid, which was seen as a darker, optically empty space. This is due to the inability of low coherent light to pass through the lesion secondary to increased melanin density within the tumor.
Additional clues that may be helpful in differentiating a suspicious nevus from a small melanoma include the presence of drusen, RPE hyperplasia, bone spicule pigment, RPE atrophy and choroidal neovascularization. Any of those findings are indicative of chronicity and suggest that the lesion has been present for some time. An actively growing melanoma, on the other hand, does not have time to develop these more chronic changes.
Ultimately, the best way to determine if the lesion is a nevus or a melanoma is to photodocument the presentation over time. Choroidal nevi will rarely exhibit any significant growth.
An interesting question to consider: Do melanomas develop from a malignant transformation of preexisting nevi, or are they completely separate entities? Most experts agree that the vast majority of melanomas manifest as separate entities.2-4 Malignant transformation from preexisting nevi is exceedingly rare, with an incidence of one in 4,800 to one in 8,800 individuals.2
In 1995, ophthalmologists Carol and Jerry Shields and associates at the Wills Eye Institute in Philadelphia identified five common risk factors associated with small choroidal melanocytic lesion growth in 1,329 patients:3
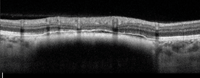 | |
| 2. Enhanced-depth imaging scan of the lesion on Spectralis OCT. What do you see? |
• Tumor thickness greater than 2.0mm.
• Presence of subretinal fluid.
• Visual symptoms.
• Presence of orange pigment.
• Posterior tumor margin touching the disc.
The researchers observed lesion growth in just 4% of patients who had no risk factors. However, 36% of patients who had one risk factor and 50% of those who had three or more risk factors experienced lesion growth.3
In a subsequent study, the Shields research team noted that patients were at an increased risk for metastasis if they exhibited posterior tumor margin touching the disc, documented growth and/or increased tumor thickness (greater than or equal to 1.1mm).4
Even though we believe our patient’s lesion is a choroidal nevus, she has a few risk factors for growth and/or malignant transformation. These include the close proximity to the optic nerve, its thickness and the presence of subretinal fluid. Because of the relatively small lesion size and uncertainty for growth potential, we elected to follow her every four to six months. We also prescribed a pair of reading glasses to address her near vision difficulties.
After three years of follow-up evaluations, our patient’s lesion has yet to show any signs of growth.
1. Gass JD. Problems in the differential diagnosis of choroidal nevi and malignant melanomas. Am J Ophthalmol. 1977 Mar;83(3):299-323.
2. Singh AD, Kalyani P, Topham A. Estimating the risk of malignant transformation of a choroidal nevus. Ophthalmology. 2005 Oct;112(10):1784-9.
3. Shields CL, Shields JA, Kiratli H, et al. Risk factors for growth and metastasis of small choroidal melanocytic lesions. Ophthalmology. 1995 Sep;102(9):1351-61.
4. Shields, CL, Cater JC, Shields JA, et al. Combination of clinical factors predictive of growth of small choroidal menalocytic lesions tumors. Arch Ophthalmol. 2000 Mar;118(3):360-4.

